TCM vs Western Medicine: 6 Common Conditions Compared
Is TCM or Western medicine better? The honest answer: it depends on your condition and needs. This article fairly compares both approaches across six common conditions — cough, eczema, pain, insomnia, digestive issues, and menstrual irregularities — to help you make the right choice.
Medical review: Dr. Tai Wai Ho, Samson,Registered Chinese Medicine Practitioner #008702
1-Minute Quick Answer
TCM or Western medicine — which is right for you? It depends on your condition. Dr Tai (CMCHK 008702) at Aspira TCM Lai Chi Kok fairly compares both approaches across 6 common conditions: cough, eczema, pain, insomnia, digestive issues, and menstrual irregularities.
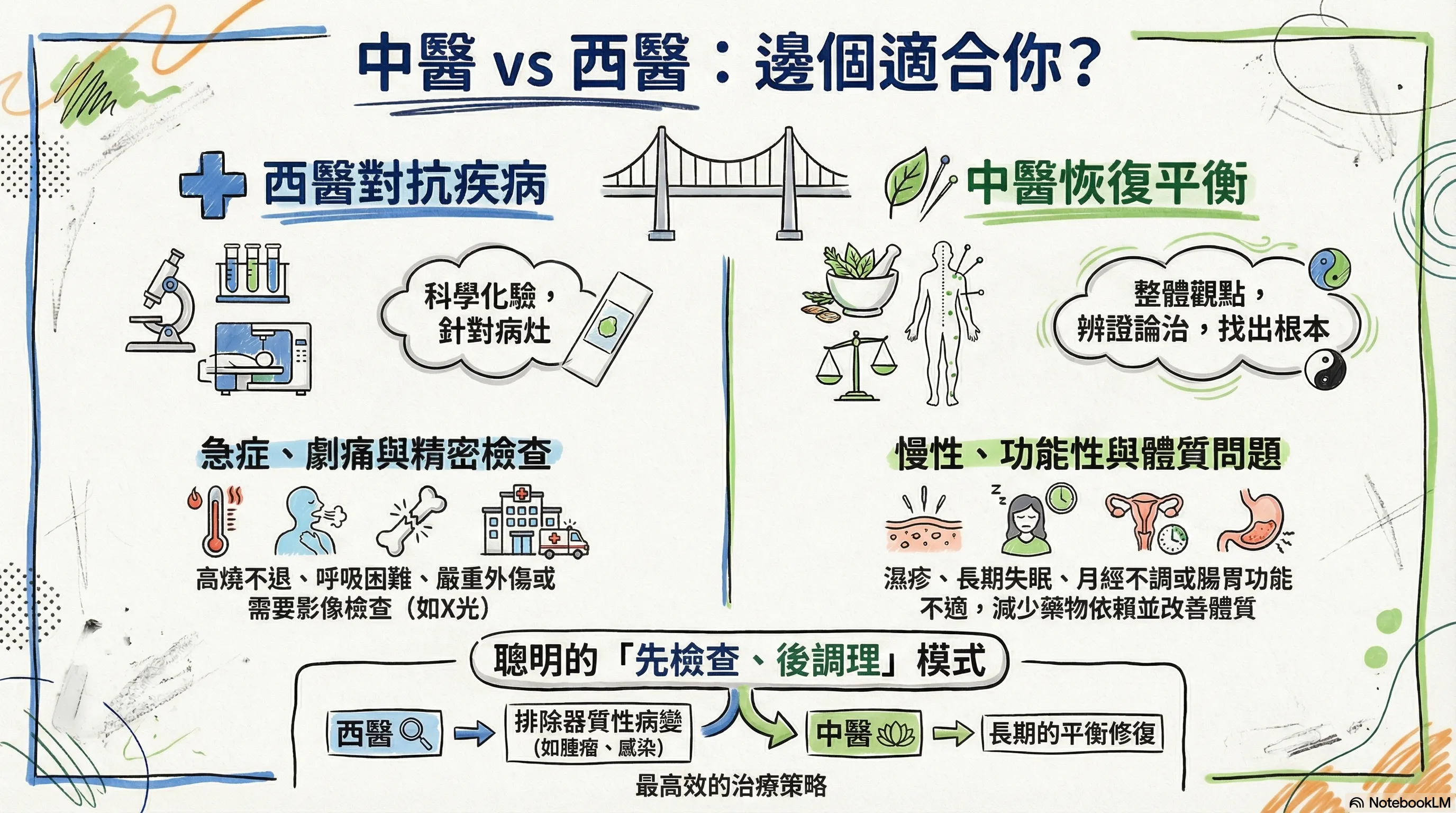 To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
"Should I see a Chinese medicine doctor or a Western doctor for this?"
This is perhaps the most common healthcare question in Hong Kong. Online searches for "TCM vs Western medicine" remain consistently high, yet most articles are biased toward one side or the other, making it hard to get an objective picture.
Our position in this article is straightforward: TCM and Western medicine each have distinct strengths. There is no "which is better" — only "which is more suitable for your specific situation." We will compare both approaches across six of the most common health conditions in Hong Kong, examining treatment methods, speed of results, long-term outcomes, and potential risks to help you make an informed decision.
Understanding the Core Difference: Two Medical Philosophies
Before comparing individual conditions, understanding the fundamental difference between these two systems will help you make sense of everything that follows.
Western medicine (modern medicine):
- Built on scientific evidence, using tests and investigations to identify specific causes
- Targets pathogens or pathological changes directly (e.g. antibiotics for infection, surgery for structural problems)
- Excels at emergency care, precise diagnosis, and standardised treatment protocols
- Medications undergo rigorous clinical trials with well-documented efficacy and side effects
Traditional Chinese Medicine (TCM):
- Built on a holistic view of the body as a dynamic, interconnected system
- Uses pattern differentiation (bian zheng) to identify the root cause of imbalance, not just eliminate symptoms
- Excels at chronic disease management, constitutional improvement, and functional disorders
- Treatment plans are highly individualised — the same disease in different people may require different approaches
In simple terms: Western medicine excels at "fighting disease"; TCM excels at "restoring balance." They are not opposing forces — they are complementary.
6 Common Conditions: TCM vs Western Medicine
1. Cough / Common Cold
One of the most debated questions: is TCM or Western medicine faster for treating a cold and cough?
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Cough suppressants, expectorants, antipyretics; antibiotics for bacterial infection | Pattern differentiation (wind-cold / wind-heat / phlegm-damp), treated with herbal formulas |
| Speed of results | Fever and cough relief typically within 1-2 days | Generally 2-3 days; some acute cold formulas work equally fast |
| Long-term outcomes | Manages symptoms; does not change underlying constitution | Regulates constitution, reducing frequency of recurrence |
| Side effect risks | Cough medicine may cause drowsiness; antibiotic overuse can lead to resistance | Relatively fewer side effects, but accurate pattern diagnosis is essential |
| Best suited for | High persistent fever, suspected bacterial infection, need for rapid symptom control | Recurring colds, lingering cough, constitutionally weak individuals |
The honest take: For an ordinary cold, TCM and Western medicine actually have comparable response times. Western medicine's advantage lies in rapid fever control and ruling out complications (such as pneumonia). TCM's advantage lies in constitutional regulation that reduces future recurrence. If you catch a cold every time the weather changes, or your cough always lingers for weeks, TCM is well worth considering.
2. Eczema
Eczema is one of the most distressing skin conditions and one of the most debated areas between TCM and Western medicine.
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Topical corticosteroids, emollients; severe cases may use immunosuppressants or biologics | Pattern differentiation (damp-heat / blood deficiency with wind-dryness / spleen deficiency with dampness), internal herbs plus external washes |
| Speed of results | Corticosteroids typically show clear improvement within days | Generally takes 2-4 weeks for noticeable improvement |
| Long-term outcomes | Risk of rebound (flare after stopping medication); long-term steroid use can thin the skin | Addresses root constitutional issues; results tend to be more lasting, but treatment takes longer |
| Side effect risks | Steroid side effects (skin atrophy, pigmentation); biologics are extremely expensive | Fewer side effects, though short-term detox reactions may occur during treatment |
| Best suited for | Acute flares requiring rapid control, severe eczema needing potent treatment | Recurring eczema, desire to reduce steroid dependence, seeking long-term stability |
The honest take: There is no single cure-all for eczema. Western medicine is genuinely powerful at controlling acute flares — corticosteroids can quickly stop itching and inflammation. But the risks of long-term steroid dependence are equally real. TCM's strength lies in addressing the underlying constitution, particularly for chronic recurring eczema where herbal medicine can gradually reduce flare frequency and severity. Ideally, use Western medicine to control acute flares, then transition to TCM for constitutional regulation.
3. Pain Conditions (Lower Back Pain / Neck and Shoulder Pain)
The universal complaint of urban dwellers — the bane of screen addicts and desk workers everywhere.
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Painkillers (NSAIDs), muscle relaxants, physiotherapy; surgery for severe cases | Acupuncture, tuina massage, herbal medicine, cupping, heat therapy |
| Speed of results | Painkillers typically work within 30 minutes | Acupuncture provides high immediate relief rates; significant improvement after 2-3 sessions |
| Long-term outcomes | Painkillers provide only temporary relief; physiotherapy offers better long-term results | Acupuncture combined with tuina and herbs shows good long-term outcomes for chronic pain |
| Side effect risks | Long-term NSAID use can damage the stomach and kidneys; surgery carries inherent risks | Acupuncture has virtually no side effects (occasional minor bruising) |
| Best suited for | Need to rule out structural issues (e.g. disc herniation), acute severe pain, surgical candidates | Chronic pain, preference to avoid long-term painkillers, those who prefer non-pharmaceutical treatment |
The honest take: Pain management is one of TCM's traditional strengths. The World Health Organization has long recognised acupuncture's efficacy for various pain conditions. However, one critical point: if you experience acute severe pain, or suspect a structural problem (such as a herniated disc compressing a nerve), you must get Western medical investigations first (X-ray, MRI) to rule out conditions requiring surgery before deciding on a treatment plan.
4. Insomnia
Sleep quality in Hong Kong has always been poor, and the number of people seeking treatment for insomnia continues to rise.
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Sleeping pills (benzodiazepines or non-benzodiazepines), Cognitive Behavioural Therapy for Insomnia (CBT-I) | Pattern differentiation (heart-spleen deficiency / liver fire / heart-kidney disharmony), herbal medicine for calming the spirit, acupuncture |
| Speed of results | Sleeping pills work the same night | Generally 1-2 weeks for gradual sleep quality improvement |
| Long-term outcomes | Sleeping pills do not address root causes; CBT-I has good long-term results but takes time | Addresses underlying organ function, reducing insomnia recurrence |
| Side effect risks | Sleeping pills carry dependency and withdrawal risks; may affect daytime alertness | Fewer side effects, but accurate pattern diagnosis is essential for effectiveness |
| Best suited for | Severe insomnia significantly affecting daily function, those needing immediate relief | Chronic light sleep with excessive dreaming, those wanting to avoid sleeping pill dependency, those with accompanying symptoms |
The honest take: The speed of sleeping pills is unmatched — you take one and you sleep. But the dependency problem is equally undeniable: many patients need increasing doses and find themselves unable to stop. TCM's advantage in treating insomnia is that it does not just make you "fall asleep" — it investigates why you cannot sleep well (Is it stress causing liver fire? Or overthinking injuring the spleen?), then treats the source. The downside is slower results, requiring one to two weeks of patience. If you are currently taking sleeping pills, we recommend gradually incorporating TCM under medical guidance rather than stopping medication on your own.
5. Digestive Issues (Stomach Pain, Bloating, Diarrhoea, Constipation)
"I can't eat" and "my stomach constantly feels full" are among the most common health complaints in Hong Kong.
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Antacids (PPIs, H2 blockers), anti-diarrhoeal or laxative medications; gastroscopy/colonoscopy for investigation | Pattern differentiation (spleen-stomach cold deficiency / liver-stomach disharmony / food stagnation), herbal medicine to regulate digestive function |
| Speed of results | Antacids typically relieve symptoms within hours | Generally 1-2 weeks for gradual digestive improvement |
| Long-term outcomes | Symptoms often return after stopping medication; long-term PPI use is controversial | After regulating spleen-stomach function, recurrence rates are lower |
| Side effect risks | Long-term PPI use may affect calcium absorption and increase infection risk | Fewer side effects, though those with weak digestion may need formula adjustments initially |
| Best suited for | Need to rule out organic disease (ulcers, tumours), acute symptoms requiring quick relief | Functional digestive problems, recurring issues, those not responding to dietary changes alone |
The honest take: Digestive symptoms absolutely require Western medical investigation first — especially if you have warning signs such as weight loss, black stools, or persistent vomiting, which necessitate ruling out stomach ulcers, H. pylori infection, or other organic conditions. Once serious conditions have been excluded, for functional dyspepsia (where tests are normal but you still feel unwell), TCM's approach to regulating spleen-stomach function is often more effective and more sustainable than long-term antacid use.
6. Menstrual Irregularities (Period Pain, Cycle Disruption, Abnormal Flow)
Many women endure menstrual problems for years, tolerating each episode until the condition progressively worsens.
| Dimension | Western Medicine | TCM |
|---|---|---|
| Treatment approach | Oral contraceptives for cycle regulation, hormone replacement therapy, painkillers; surgery for severe cases | Pattern differentiation (qi stagnation with blood stasis / qi-blood deficiency / kidney deficiency), herbal medicine to regulate qi and blood, acupuncture |
| Speed of results | Contraceptive pills typically show results within 1-2 menstrual cycles | Generally requires 2-3 menstrual cycles for gradual regulation |
| Long-term outcomes | Problems may return after stopping medication; concerns about long-term hormone use | Constitutional regulation tends to produce more lasting results |
| Side effect risks | Hormonal medication may cause weight gain, mood swings, and blood clot risk | Fewer side effects, but the longer treatment course requires patience |
| Best suited for | Need to rule out organic issues (fibroids, PCOS), severe period pain requiring rapid relief | Functional menstrual irregularities, preconception care, those wanting to avoid long-term hormone medication |
The honest take: Like digestive issues, menstrual irregularities warrant a gynaecological examination first to rule out fibroids, polycystic ovary syndrome (PCOS), and endometriosis. Once serious pathology has been excluded, TCM has exceptionally rich experience in menstrual regulation, particularly for women trying to conceive — herbal regulation of qi and blood is a gentler approach than hormonal medication.
The Smartest Approach: Integrating TCM and Western Medicine
Having read the six comparisons above, you may have noticed a pattern: for many conditions, the best approach is actually an integration of both.
This is not diplomatic fence-sitting — it is clinical reality. Each system has its blind spots:
- Western medicine's blind spot: For functional disorders (where tests are normal but symptoms persist) and chronic constitutional issues, it often can only prescribe the same categories of medication repeatedly without achieving a cure
- TCM's blind spot: For emergencies (heart attack, stroke, severe infection) and conditions requiring precision investigation (such as tumour screening), Western medicine is indispensable
A practical integration model:
- Western investigation first, to rule out serious conditions — blood tests, imaging, and endoscopy are Western medicine's strengths
- Western medicine for the acute phase — high fever, severe pain, and acute allergic reactions require Western medication to stabilise quickly
- Transition to TCM for the stabilisation phase — once symptoms are controlled, TCM addresses constitutional root causes, reducing recurrence and medication dependence
- Long-term TCM maintenance — periodic regulation to maintain balance and prevent illness
At Aspira TCM, we will never tell you that "Chinese medicine is definitely better than Western medicine." If your condition is better served by seeing a Western doctor first, we will tell you directly. Because truly caring for patients means helping you find the most appropriate treatment pathway — not keeping every patient within our own clinic.
When to See a Western Doctor First? When Can You Go Directly to TCM?
Here is a simple decision reference:
See a Western doctor first if you have:
- Persistent high fever (above 38.5 degrees Celsius)
- Severe chest pain or breathing difficulty
- Sudden severe headache
- Traumatic bleeding or fractures
- Unexplained rapid weight loss
- Blood in stools or black stools
- Newly discovered lumps
- Suspected serious infection (wound with redness, swelling, and pus)
You can see a TCM practitioner directly if you have:
- Recurring colds or lingering cough
- Chronic skin conditions (eczema, acne)
- Chronic pain (lower back, neck and shoulder, headache)
- Insomnia, fatigue, low energy
- Indigestion, bloating, constipation
- Menstrual irregularities, period pain
- Weak constitution, prone to illness
- Stress-related symptoms
- Preconception care
Consider Western investigation first, then complement with TCM if you have:
- Worsening symptoms with unknown cause
- New symptoms after age 40
- Family history of serious illness
- Existing chronic conditions (diabetes, hypertension) requiring monitoring
Remember, this is general guidance only. If you are unsure, feel free to contact us. After understanding your situation, we can recommend the most appropriate care pathway.
Aspira TCM's Approach
At Aspira TCM Clinic, our philosophy is "the healer gives their all; the physician follows their conscience." In practice, this means:
- We never disparage Western medicine — if your condition requires Western medical intervention, we will tell you directly
- We prioritise precise pattern differentiation — every patient's treatment plan is tailored to their individual constitution and diagnostic findings
- We emphasise treating the root cause — not just relieving symptoms, but identifying and addressing the underlying issues
- We track outcomes — through continuous follow-up to ensure treatment is on the right track
Aspira TCM Clinic is located in Lai Chi Kok, staffed by a team of five registered Chinese medicine practitioners and one registered physiotherapist, covering internal medicine, dermatology, gynaecology, pain management, and more. Whatever your health concern falls under, we can provide a professional assessment and honest advice.
Frequently Asked Questions (FAQ)
Q: Can I take Chinese herbs and Western medication at the same time? Will they interact?
This is a common concern. Some Chinese herbs and Western medications can indeed interact, so we recommend: (1) Always inform your TCM practitioner of all Western medications you are taking; (2) Take Chinese herbs and Western medication at least two hours apart; (3) Never stop Western medication on your own — any adjustments should be made under medical guidance. At Aspira TCM, our practitioners carefully assess the risk of drug interactions.
Q: Do I need Western medical tests before seeing a TCM practitioner?
Not necessarily, but we encourage patients to bring any recent Western medical reports they may have. This objective data helps your TCM practitioner build a more complete picture of your health. If you have not had relevant tests and we identify potential concerns during consultation, we will recommend you get Western investigations first.
Q: How long does TCM treatment usually take to show results?
This varies by condition and individual constitution. Generally, acute conditions (such as colds or acute lower back pain) may respond within 2-5 days. Chronic conditions (such as eczema, insomnia, or menstrual irregularities) typically show initial improvement in 2-4 weeks, with complete regulation potentially taking 2-3 months. Your practitioner will outline an approximate treatment plan and timeline after your first consultation.
Q: Is there scientific evidence for TCM?
Increasingly, yes. The World Health Organization has included acupuncture in its recommended treatments for numerous conditions, and leading medical journals (such as JAMA and The Lancet) have published substantial TCM clinical research. TCM's research methodology differs from Western medicine — TCM emphasises individualised treatment (pattern differentiation), which makes standardised randomised controlled trials more challenging, but this does not mean TCM lacks efficacy.
Q: How much does Aspira TCM charge? Do you accept the Health Care Voucher?
Aspira TCM Clinic accepts the Elderly Health Care Voucher. Specific fees vary by treatment type (herbal medicine, acupuncture, tuina, etc.) — please contact us directly for the latest pricing details. We are committed to transparent pricing with no hidden charges.
If you are deliberating whether to see a TCM practitioner or a Western doctor, feel free to contact us directly. After an initial understanding of your situation, we can recommend the most appropriate treatment direction — even if the answer is "you should see a Western doctor for investigation first."
WhatsApp Booking: Book Now Aspira TCM Clinic — Unit 2706, Saxon Tower, 7 Cheung Shun Street, Lai Chi Kok
-- Reviewing Practitioner -- Dr Tai | Registered Chinese Medicine Practitioner (Reg. No.: 008702) Aspira TCM Clinic — Internal Medicine, Dermatology, Gastroenterology
This content is for health education purposes only and does not constitute medical diagnosis or treatment advice. Individual conditions vary, and treatment plans should be tailored accordingly. The comparisons between TCM and Western medicine are based on general clinical observations; treatment outcomes for individual cases may differ. If you have a health concern, we recommend booking a consultation so a qualified practitioner can assess your specific situation.
Related at Aspira TCM: TCM limitations: 5 times to see a Western doctor first · Cough (TCM) overview
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Low Back Pain: 6 Common Causes & TCM Treatment Approaches
Low back pain is not always simply “kidney deficiency” or muscle fatigue. It may also be related to muscle strain, disc herniation, degenerative lumbar disease, kidney stones, urinary tract infection, or pelvic inflammation. This article explains six common causes of low back pain from a TCM perspective and outlines key distinctions and treatment directions.

TCM Limitations: 5 Times to See a Western Doctor First
TCM has genuine strengths in chronic care and holistic wellness, but it is not the right first choice for every situation. This article honestly discusses 5 scenarios where Western medicine should come first, what TCM truly excels at, and how to make informed decisions between the two.

Is Aspira TCM Clinic Good? Doctors, Services & Real Reviews
Searching "Is Aspira TCM good?" means you're doing your homework — and we respect that. This article presents our doctor team, five clinic differentiators, real patient feedback, and our honest limitations, so you can decide if Aspira is right for you.