A 75-Year-Old Mother Keeps Forgetting to Turn Off the Stove: A TCM Assessment Approach to Dementia Warning Signs
Ms Lee’s 75-year-old mother has recently begun repeating the same questions, mixing up her medication, and even forgetting to turn off the stove. Is this ordinary forgetfulness, poor sleep, or an early dementia warning sign? This article explains how TCM can assess an older adult’s memory changes step by step through the lenses of safety, cognitive function, vascular risk, sleep, constitution, and family caregiving.
Medical review: Dr. Chan Wing Kiu, Joanne,Registered Chinese Medicine Practitioner #009463
A 75-Year-Old Mother Keeps Forgetting to Turn Off the Stove: A TCM Assessment Approach to Dementia Warning Signs
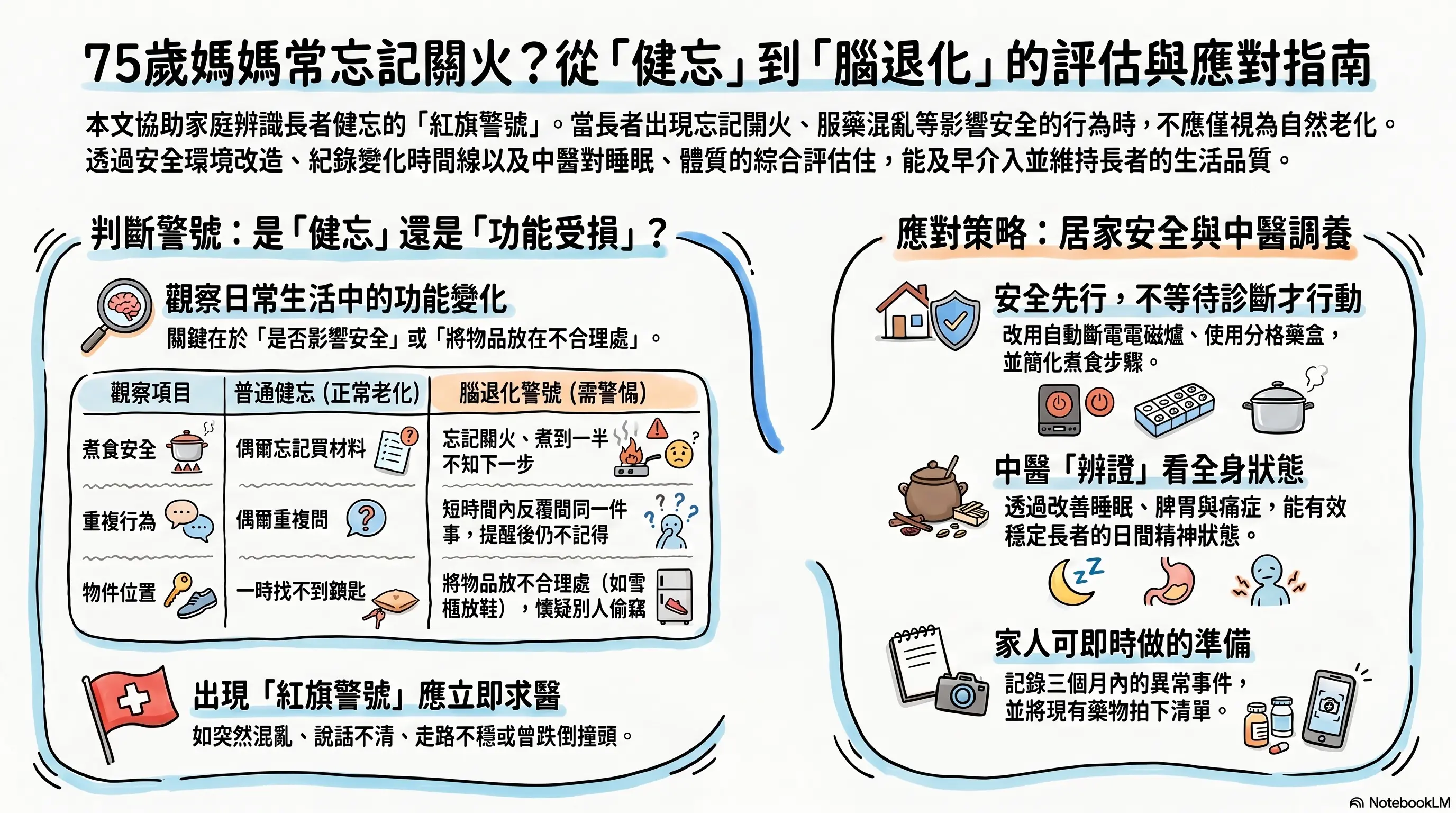 To help readers grasp the article more quickly, the cover image was generated with NotebookLM. Some Chinese text may not render perfectly.
To help readers grasp the article more quickly, the cover image was generated with NotebookLM. Some Chinese text may not render perfectly.
Ms Lee’s 75-year-old mother has recently begun repeating the same questions, mixing up her medication, and even forgetting to turn off the stove. Is this ordinary forgetfulness, poor sleep, or an early warning sign of dementia? This article shows how TCM can assess such a situation step by step through the lenses of safety, cognition, vascular risk, sleep, constitution, and caregiving.
Ms Lee’s mother is 75 years old and used to cook, buy groceries, and take medication independently in a very orderly way. Over the past six months, however, Ms Lee has started noticing clear changes. Her mother repeatedly asks, “Will you come home for dinner tonight?” and asks again ten minutes later. There are repeated grocery purchases in the fridge. Most worrying of all, she has forgotten to turn off the stove twice after making soup, and the family only noticed in time by chance.
Her mother feels that “memory naturally gets worse with age” and is somewhat resistant to seeking medical advice. Ms Lee, on the other hand, is increasingly worried: is this simple forgetfulness, or could it be an early sign of dementia?
When an older adult has memory problems and starts forgetting to turn off the stove, Aspira TCM does not jump straight to “brain tonics”. The assessment starts with safety, then cognition, then the wider body, sleep, vascular risks, and constitution.
Step 1: Distinguish “Forgetfulness” from “Functional Impairment”
Many families get stuck on the same question at the start: is an older person’s memory decline still normal? Occasional forgetfulness is not always alarming. The key issue is whether everyday function is being affected.
| Family observation | More typical of ordinary forgetfulness | More concerning for dementia |
|---|---|---|
| Misplacing objects | Temporarily cannot find keys, then later finds them | Puts objects in unreasonable places and suspects others of stealing them |
| Asking questions | Occasionally repeats a question | Repeats the same question within a short time and still does not remember after reminders |
| Cooking | Occasionally forgets to buy one ingredient | Forgets to turn off the stove or no longer knows what step comes next |
| Medication | Occasionally takes it later than intended | Repeats doses, misses doses, or confuses morning and evening medication |
| Going out | Needs company in a new place | Gets lost in familiar places or does not know how to get home |
| Money handling | Calculates more slowly | Pays twice, buys things irrationally, or becomes easier to deceive |
In Ms Lee’s mother’s case, forgetting to turn off the stove is no longer just poor memory. It directly affects home safety. Even if the eventual assessment does not show dementia, it still deserves prompt attention.
Step 2: Address Safety First Rather Than Waiting for a Diagnosis
When caring for an older adult with memory decline, action does not have to wait until a formal diagnosis is made. Once high-risk behaviour appears, the priority is to reduce the chance of harm.
For stove-related risk, families can start with practical measures:
- Switch to an induction cooker or timer with automatic shut-off
- Avoid letting the older person manage soup or open-flame cooking alone
- Use short, clear kitchen reminders rather than covering the walls with notes
- Simplify routine cooking steps by fixing cooking times and using familiar cookware
- Reassign cooking responsibility if forgetting to turn off the stove has already happened multiple times
For medication, a weekly pill organiser, a weekly family check, and a photographed medication list can help prevent missed or repeated doses. Extra care is needed if the person is taking diabetes medication, blood pressure medication, anticoagulants, or sleeping pills.
Step 3: Clarify the Timeline of Change
When Dr Chan assesses this kind of case, some early questions are especially important:
| Question | Why it matters |
|---|---|
| Did the memory decline appear suddenly or gradually? | Sudden confusion raises concern for infection, stroke, medication, or metabolic causes |
| Has there been any fall, head injury, or hospital admission in recent months? | Head trauma or post-illness decline can worsen cognition |
| Is there a history of hypertension, diabetes, high cholesterol, or stroke? | Vascular risk affects brain health |
| Has sleep worsened or become day-night reversed? | Poor sleep can worsen daytime confusion and may also reflect cognitive decline |
| Has mood changed, such as low mood, anxiety, or suspiciousness? | Depression, anxiety, and dementia can all affect memory |
| Have hearing or vision worsened? | Reduced sensory input can lower stimulation and be mistaken for memory decline |
| What medications and supplements are being taken? | Polypharmacy or side effects may affect mental state |
If an older adult becomes suddenly confused, drowsy, unsteady when walking, unclear in speech, feverish, or develops painful urination over a few days, this is not a routine TCM regulation scenario. Western medical review or urgent care should come first.
Step 4: Look for Early Dementia Warning Signs
In medical assessment, dementia is not judged by memory alone. It may affect memory, understanding, language, learning, calculation, judgment, and daily function, and can also bring emotional or behavioural changes. Families can observe the following:
-
Recent memory
Does the person forget what just happened, what was just eaten, or what was just said? -
Executive function
Has it become harder to manage familiar chores, cooking, bills, or transport? -
Orientation to time and place
Does the person get lost in familiar places, confuse morning and afternoon, or mix up dates? -
Language and communication
Does the person often struggle to find words, speak vaguely, or fail to follow longer instructions? -
Judgment and safety
Does the person forget to turn off the stove, eat spoiled food, or fail to notice danger? -
Mood and personality
Has the person become more withdrawn, anxious, suspicious, irritable, or socially disengaged?
In Ms Lee’s mother’s case, repeated questioning, duplicated grocery purchases, and forgetting to turn off the stove already reach the threshold for further assessment. This does not prove dementia, but it should no longer be dismissed as ageing alone.
Step 5: TCM Assessment Looks Beyond “Memory”
TCM does not assess an older adult’s forgetfulness by asking only whether they remember things. Many factors that drag down concentration and memory are hidden in the person’s wider physical state.
Common questions include:
- Sleep: difficulty falling asleep, waking easily, vivid dreams, day-night reversal
- Appetite: poor intake, bloating, strong fatigue after meals
- Bowels: constipation, loose stool, or bowel motion only every few days
- Urination: frequent night urination, urgency, or frequency
- Energy: fatigue, low voice, low motivation, daytime heaviness
- Mood: anxiety, low mood, irritability, suspiciousness
- Pain: low back pain, headaches, neck and shoulder pain, reduced mobility
- Vascular risk: whether blood sugar, blood pressure, and lipids are stable
This is then combined with pulse, tongue, and overall TCM pattern differentiation, such as kidney essence deficiency, spleen qi and blood deficiency, phlegm turbidity disturbing the head, blood stasis, or poor nourishment of the spirit.
| TCM pattern | What may be seen in older adults | Treatment direction |
|---|---|---|
| Kidney essence deficiency | Weak low back and knees, tinnitus, night urination, low energy, memory decline | Nourish the liver and kidneys, replenish essence |
| Spleen qi and blood deficiency | Poor appetite, fatigue, pale complexion, weak concentration | Strengthen the spleen, boost qi, nourish blood, calm the mind |
| Phlegm turbidity disturbing the head | Heavy-headedness, chest oppression, obesity, excess phlegm, brain fog | Strengthen the spleen, transform phlegm, improve metabolism |
| Blood stasis obstructing the channels | Headache, dark tongue, numb limbs, poor circulation | Move blood and unblock the channels, after acute issues are ruled out |
| Poorly nourished spirit | Insomnia, vivid dreams, palpitations, anxiety, being easily startled | Nourish the heart, calm the mind, stabilise sleep |
These patterns do not replace Western diagnosis. They help the practitioner understand why the person’s overall condition is declining, what modifiable factors may be present, and what should first be referred onward.
Step 6: When Should Western Medical Review Be Recommended?
At Aspira TCM, the following situations would prompt advice for timely Western medical assessment or memory testing:
- Ongoing decline in memory and daily functioning
- Recurrent forgetting to turn off the stove, getting lost, or medication confusion
- Sudden confusion, unsteady walking, or unclear speech
- Cognitive decline after a fall or head injury
- Hallucinations, delusions, aggressive behaviour, or serious safety risk
- The family can no longer maintain safety through reminders alone
Depending on the situation, doctors may arrange cognitive testing, blood tests, medication review, brain imaging, or specialist referral. Dementia diagnosis requires history, functional change, and appropriate examination findings. It cannot be made by a single online test.
What Can TCM Contribute in This Situation?
Once acute problems have been excluded, or while formal assessment is pending, TCM may support care in several ways:
-
Improving sleep and day-night rhythm
Poor sleep at night can make daytime confusion, falls, and mood instability worse. TCM may regulate insomnia, vivid dreams, irritability, or night urination according to constitution. -
Improving appetite and bowel function
Poor intake, constipation, and bloating can lower both energy and alertness. In older adults, better digestion often supports a steadier day-to-day state. -
Managing pain and inactivity
Knee pain, low back pain, and neck or shoulder pain can reduce outings, social contact, and activity, indirectly affecting mental and physical function. -
Supporting vascular risk management
Poorly controlled diabetes, hypertension, and high cholesterol increase vascular and brain health risk. TCM may help constitutional support, but medication changes must be made by the treating Western doctor. -
Helping caregivers stabilise daily routines
Fixed routines for sleep, medication, outings, and simplified household steps are often more effective than blaming the person for being “forgetful”.
Eight Things Families Can Do Right Away
If an older family member has already started forgetting the stove or mixing up medication, the following steps may help:
- Record specific events from the past three months, including date, time, what happened, and the consequence
- Photograph all current medication and prepare a medication list
- Check open flames, gas, power points, and floor clutter at home
- Use a pill organiser instead of mixing multiple medication bags together
- Arrange a general health check or memory assessment
- Keep daily routine and activity timing more stable
- Preserve safe and manageable household tasks rather than removing all independence at once
- Divide responsibilities among family members for appointments, medication, cooking, and finances
Caring for an older person at risk of dementia should not rest on one person alone. Earlier division of roles usually means fewer conflicts later.
How Can Families Bring Up Assessment?
Many older adults strongly resist the word “dementia” because it feels like a label. It is often better to avoid leading with that label and instead use gentler language:
"You have not been sleeping very well recently, and there was that incident with the stove. Let us go together and see whether sleep, medication, or general health might be affecting things. It would be more reassuring to sort it out earlier."
"This does not mean you definitely have an illness. Let us just do a memory and health check to see whether anything can help you feel clearer and sleep better."
The key is to frame assessment as a way to find causes and improve daily life, not as proof that something is “wrong” with the person.
Aspira TCM’s Assessment Priorities
For a case like Ms Lee’s mother, Aspira TCM would focus first on three areas:
- Safety risk: whether cooking, medication, going out, falls, or finances already involve danger
- Medical risk: whether stroke, infection, medication side effects, unstable diabetes or hypertension, or other internal medical problems must first be excluded
- Constitutional state: whether sleep, digestion, qi and blood, liver-kidney balance, phlegm and stasis, pain, or mood are dragging down overall function
If TCM regulation is appropriate, Dr Chan will tailor the plan to the person’s constitution. If Western medical review or memory assessment is needed first, this will also be explained clearly to the family. For older adults, the most important goal is not rushing to a label, but stabilising safety and general health as early as possible.
FAQ
1. If someone forgets to turn off the stove once, does that already mean dementia?
Not necessarily. A single event may be related to fatigue, distraction, poor sleep, or emotional strain. But if it happens repeatedly, or comes together with repeated questioning, getting lost, medication confusion, or disorganised cooking steps, assessment should be arranged promptly.
2. If the older adult refuses Western medical care, can TCM be the first step?
Yes, TCM can sometimes serve as an entry point. But if the practitioner judges that there is acute risk or clear concern for cognitive decline, Western medical assessment should still be recommended. TCM should not replace necessary cognitive testing, blood work, or brain investigation.
3. Does dementia always worsen quickly?
Progress varies greatly depending on type and individual circumstances. Early diagnosis, management of diabetes and hypertension, better sleep and nutrition, ongoing activity and social contact, home safety planning, and caregiving support can all help preserve quality of life.
4. Should the family immediately stop the older adult from cooking?
That depends on risk. If forgetting to turn off the stove has happened multiple times, the person should stop using open flame alone. But that does not mean all independence must be removed. Safer stoves, accompanied cooking, or lower-risk kitchen tasks may still be possible.
5. How soon might TCM regulation make a difference?
That depends on what is driving the problem. If poor sleep, weak digestion, constipation, or chronic pain are major contributors, some people feel more alert in the daytime once those factors improve. If dementia is already present, the goal is usually more about stabilising function, improving quality of life, and supporting caregiving arrangements.
Disclaimer: This article is for health education only and does not replace individual consultation, cognitive assessment, or treatment advice. If an older adult develops sudden confusion, stroke symptoms, head injury, severe hallucinations, or immediate safety risk, seek medical care immediately.
Article note: The case example in this article has been anonymised for health education purposes and does not contain identifiable personal information.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Memory Lapses or Normal Ageing? TCM Explains 6 Early Dementia Warning Signs, Assessment and Prevention
Memory lapses in older adults do not always mean dementia. But when a person repeatedly asks the same question, forgets recent events, gets lost, makes mistakes with cooking, or shows clear personality changes, it should not be dismissed as ageing alone. This guide explains the differences between normal ageing and dementia, six early warning signs, common assessment methods, and how TCM may support prevention and overall function.

Feeling Tired After Meals and Waking to Urinate at Night: Are These Early Signs of Diabetes? A TCM Guide to 6 Warning Signs, Testing and Prevention
Diabetes does not always begin with dramatic symptoms. Many people notice tiredness after meals, more night urination, dry mouth, increasing abdominal fat, itchy skin, or slow wound healing before they are diagnosed. This article explains early warning signs of diabetes, who should be tested early, and how TCM may support people in the prediabetes stage.

How to Choose a Clinic for Acupoint Embedding? 2026 Hong Kong Pricing Guide + 7 Questions to Ask Before Booking
Hong Kong acupoint embedding fees range from a few hundred to over three thousand dollars per session — but why? This guide breaks down 2026 market price ranges, six factors driving the fee differences, seven questions to ask before booking, four red-flag warnings, and a transparent line-by-line look at Aspira TCM's three packages — to help you choose what genuinely suits you.