Overthinking and Sleepless Nights — Ms Lee's TCM Journey to Restful Sleep
A female office worker in her 30s struggled with difficulty falling asleep, frequent dreaming, and waking easily due to chronic work stress and anxiety. After six sessions over four weeks combining herbal medicine and acupuncture prescribed by Dr To, her sleep quality improved significantly and she regained her energy and quality of life.
Medical review: Dr. Tai Wai Ho, Samson,Registered Chinese Medicine Practitioner #008702
1-Minute Quick Answer
A female office worker in her 30s struggled with chronic insomnia, difficulty falling asleep, and frequent dreaming due to work stress. After Dr To (CMCHK 009330) at Aspira TCM Lai Chi Kok prescribed calming-spirit herbs and acupuncture across 6 sessions in 4 weeks, her sleep markedly improved.
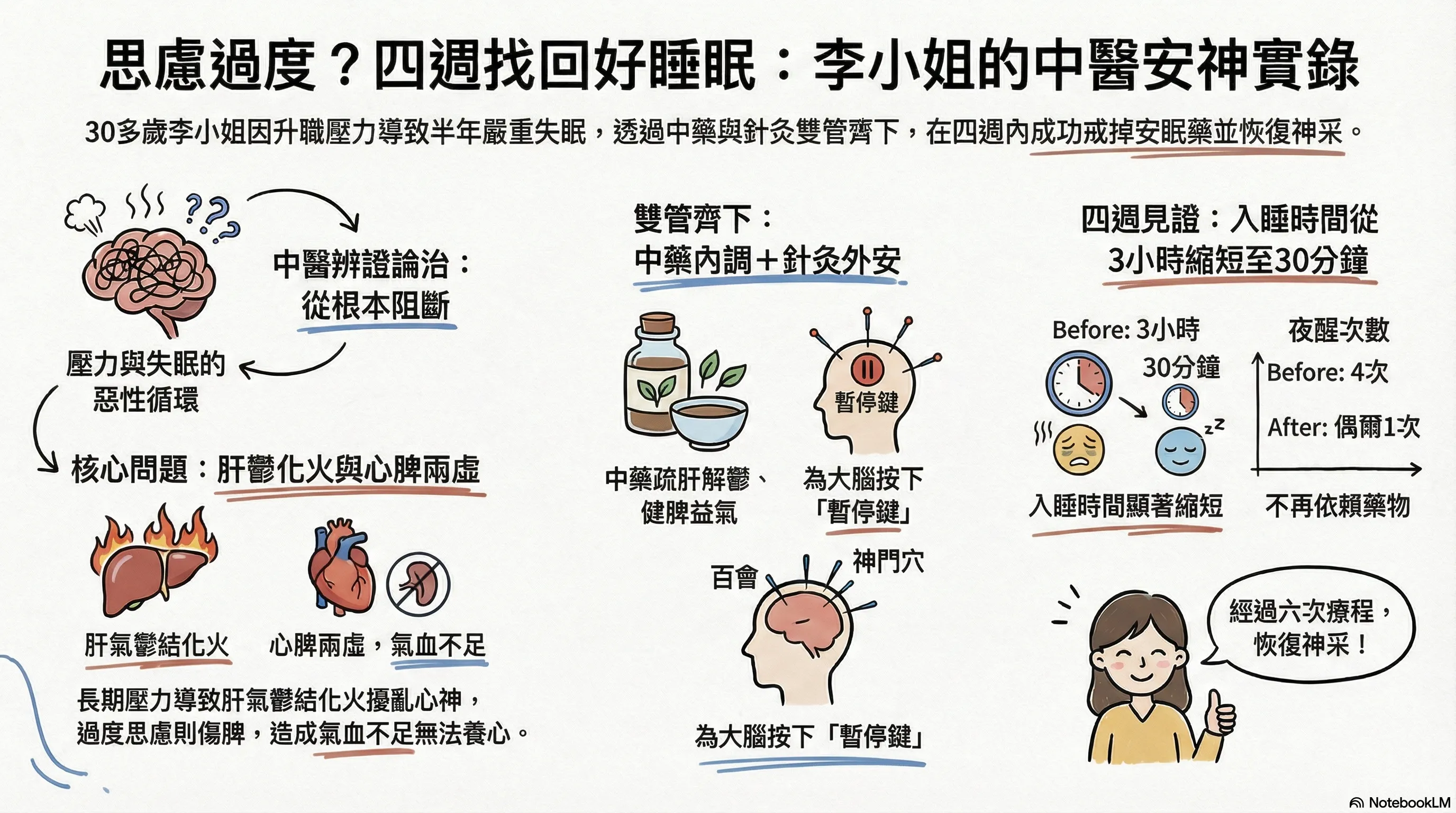 To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
Six Months of Insomnia, Exhausted in Body and Mind
Ms Lee (pseudonym) is an administrative manager in her 30s with a demanding and high-responsibility role. Six months ago, after receiving a promotion that required her to manage multiple projects and teams simultaneously, her stress levels surged. What began as the occasional restless night gradually became a nightly ordeal.
She described her situation: "The moment I lie down, my mind starts racing — tomorrow's meetings, unfinished reports, colleagues' problems. The more I think, the more awake I become. I often cannot fall asleep until two or three in the morning." What troubled her even more was that even when she did manage to fall asleep, she would wake easily in the middle of the night, and her sleep was filled with vivid dreams, leaving her more exhausted in the morning than before bed.
Over six months, Ms Lee noticed a marked decline in her memory, an inability to concentrate during the day, and increasing irritability. Colleagues and family observed her complexion deteriorating. She frequently suffered from headaches, and her appetite had diminished considerably.
She had tried various remedies: warm milk before bed, white noise, melatonin supplements, and even sleeping pills. While the pills helped her fall asleep, she would wake feeling groggy, and she was concerned about long-term dependency. A friend suggested she try Traditional Chinese Medicine, which led her to Aspira TCM Clinic.
Why Does Overthinking Cause Insomnia?
From a TCM perspective, the causes of insomnia go far beyond simply "not being able to sleep." During the initial consultation, Dr To conducted a comprehensive assessment through inquiry, observation, tongue diagnosis, and pulse diagnosis.
Dr To explained that Ms Lee's condition was a case of "liver qi stagnation transforming into fire, with dual deficiency of heart and spleen." In simpler terms, prolonged work stress and overthinking first impaired the liver's function of maintaining the smooth flow of qi, leading to liver qi stagnation. Over time, this stagnation generated internal fire that disturbed the heart spirit, resulting in difficulty falling asleep and excessive dreaming. Simultaneously, excessive worry had weakened the spleen, impairing the production of qi and blood. With insufficient heart blood to nourish the spirit, she would wake easily and sleep restlessly.
Tongue diagnosis revealed a slightly red tongue body with a thin, yellowish coating. Her pulse was wiry and thin on the left, and slightly weak on the right — clear indicators of liver stagnation with fire, and deficiency of heart and spleen qi and blood, perfectly consistent with her symptoms.
Treatment Plan: Herbal Medicine for Calming the Spirit + Acupuncture
Based on the differential diagnosis, Dr To formulated a treatment plan centred on "soothing the liver and resolving stagnation, nourishing the heart and calming the spirit, and strengthening the spleen to boost qi," combining herbal medicine and acupuncture for a dual approach.
Week 1 (Sessions 1-2): Soothing the Liver, Clearing Fire, and Initial Spirit-Calming
The initial prescription focused on soothing the liver, resolving stagnation, and clearing heart fire to calm the spirit. Dr To selected a targeted herbal formula based on Ms Lee's constitution, with the primary goal of restoring the smooth flow of liver qi and clearing stagnant fire. One dose daily for five days.
Concurrently, acupuncture treatment was administered. Key acupoints included Baihui (GV20, crown of the head — calming the spirit and settling the mind), Shenmen (HT7, wrist — tranquillising the heart), Taichong (LR3, dorsum of the foot — soothing the liver and regulating qi), and Sanyinjiao (SP6, lower leg — harmonising the liver, spleen, and kidneys). Dr To described the role of acupuncture: "It is like pressing a 'pause button' for the brain, allowing an overactive mind to gradually settle."
After the first acupuncture session, Ms Lee reported that her "mind finally felt a little quieter" that evening. Although she still had some difficulty falling asleep, the time spent tossing and turning was noticeably shorter.
Week 2 (Sessions 3-4): Strengthening Heart and Spleen Nourishment
At the follow-up, Ms Lee reported that her time to fall asleep had shortened from two to three hours to approximately one hour. She still woke once or twice during the night but was able to fall back asleep more quickly. The frequency of dreaming had also decreased.
Dr To adjusted the prescription, continuing the liver-soothing herbs while increasing the proportion of heart blood-nourishing and spleen qi-strengthening components to help restore the body's normal production of qi and blood.
For acupuncture, Xinshu (BL15) and Pishu (BL20) on the back were added to enhance the heart and spleen-tonifying effects. Ms Lee mentioned that during the second acupuncture session, she fell asleep on the treatment bed — "I had not felt that relaxed in a very long time."
Weeks 3-4 (Sessions 5-6): Consolidating Results and Constitutional Adjustment
By the third week, Ms Lee's complexion had noticeably improved. She shared happily: "These past few days, I have finally been able to fall asleep before midnight, and I sleep through until morning. I feel so much more refreshed when I wake up." Her appetite had returned, and her concentration at work had markedly improved.
Dr To continued to fine-tune the prescription, focusing on consolidating the therapeutic effects and adjusting her overall constitution. Fire-clearing herbs were reduced while qi-tonifying and yin-nourishing components were increased. By the final session, Ms Lee's pulse had improved significantly — the wiry quality on the left was diminished, and the right pulse was stronger than before.
Treatment Outcome
After four weeks of combined herbal medicine and acupuncture treatment across six sessions, Ms Lee's insomnia showed significant improvement:
- Time to fall asleep: Reduced from 2-3 hours to 20-30 minutes
- Night-time awakenings: Decreased from 3-4 times per night to occasionally once
- Dreaming: Improved from vivid dreams throughout the night to occasional dreams that no longer disrupted sleep
- Daytime energy: Normal work capacity restored; headaches and irritability resolved
- Appetite: Returned to normal; complexion visibly healthier
At a follow-up one month later, Ms Lee reported that her sleep remained stable and she no longer relied on any sleep aids. She had also incorporated the pre-sleep acupoint massage and breathing relaxation techniques that Dr To had taught her into her daily routine.
Dr To's Commentary
Insomnia is an extremely common problem among urban residents, particularly in the high-pressure age group of 30 to 50. Office workers in this demographic make up the majority of my insomnia patients.
Many people initially dismiss insomnia, thinking they can simply "push through it," or resort directly to sleeping pills. However, sleeping pills only temporarily suppress symptoms. Long-term use may lead to dependency, and they do not address the root cause of insomnia.
The advantage of TCM in treating insomnia lies in "differential diagnosis and treatment." The same symptom of insomnia can have very different underlying causes: liver stagnation transforming into fire, heart-kidney disharmony, phlegm-heat internal disturbance, or heart-spleen deficiency, among others. Identifying the true cause and prescribing accordingly is the only way to achieve lasting improvement.
Ms Lee's case is highly representative. Stress led to liver qi stagnation, which generated fire that disturbed the heart spirit. Concurrently, excessive worry weakened the spleen, resulting in insufficient qi and blood to nourish the heart — creating a vicious cycle. We used herbal medicine to regulate organ function internally, combined with acupuncture to unblock the meridians and calm the spirit externally. This integrated inside-out approach produced excellent results within four weeks.
If you are struggling with insomnia, I encourage you not to keep putting it off. The sooner you seek treatment, the more effective the results, and the easier it is to restore a normal sleep rhythm.
— Dr To Ching | Registered Chinese Medicine Practitioner (Reg. No.: 009330)
Experiencing a Similar Problem? Book a Consultation
If you are struggling with difficulty falling asleep, frequent dreaming and waking, poor sleep quality, or chronic stress-related exhaustion, you are welcome to book a consultation with Dr To.
How to book:
- WhatsApp: Book here
- Phone: 2110 9337
- Address: Unit 2706, Saxon Tower, 7 Cheung Shun Street, Lai Chi Kok
Further reading: Complete TCM Guide to Insomnia Treatment →
Disclaimer: Every patient's constitution and condition are different, and treatment outcomes vary accordingly. The above case is for reference only. Please consult a practitioner for a treatment plan tailored to your specific situation. Prescription details are shared for TCM academic purposes only and do not constitute prescribing advice. Do not self-prescribe.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Insomnia in Older Adults: Waking at Night, Dreaming, Early Waking
Does sleeping less in older age always mean insomnia? Waking easily at night, vivid dreaming, early waking, and waking tired may relate to nocturia, pain, mood, medication, sleep apnoea, or sleep habits. This article explains common causes, warning signs, and how TCM interprets insomnia patterns such as heart-spleen deficiency, disharmony between heart and kidney, and liver fire.

Insomnia: Sleeping Pills or TCM? An Honest Comparison
Sleeping pills offer immediate relief but carry dependency risks; TCM treats insomnia at the root but requires patience. This article honestly compares both approaches — benefits, risks, costs, and who each is best suited for — to help you find the right solution for your sleepless nights.

Night-Time Itchy Skin in Older Adults: A TCM Damp-Heat Case Study
When spring and summer arrive, many elderly people see their itchy skin flare up, particularly at night, and topical creams alone become less effective. Through the composite case of "Madam Chan", a 78-year-old, this article explains how TCM assesses elderly itch through the lens of damp-heat in the skin and blood-deficiency wind, walks through a phased approach to relief, and lists the warning signs (scabies, drug eruption, severe skin disease) that need a Western dermatology or internal-medicine assessment first.