Insomnia in Older Adults: Waking at Night, Dreaming, Early Waking
Does sleeping less in older age always mean insomnia? Waking easily at night, vivid dreaming, early waking, and waking tired may relate to nocturia, pain, mood, medication, sleep apnoea, or sleep habits. This article explains common causes, warning signs, and how TCM interprets insomnia patterns such as heart-spleen deficiency, disharmony between heart and kidney, and liver fire.
Medical review: Dr. Chan Wing Kiu, Joanne,Registered Chinese Medicine Practitioner #009463
1-Minute Quick Answer
Sleeping fewer hours in older age isn't always insomnia — sleep naturally shortens and lightens. What matters is waking easily, vivid dreaming, early waking, or waking tired in ways that affect daytime energy and safety. Insomnia is usually multi-factorial: nocturia, pain, stress, medication, and sleep apnoea. Reviewed by Dr Chan, CMCHK 009463.
Older Adults Waking Easily at Night, Dreaming More, or Waking Too Early: How TCM Distinguishes Causes and Sleep Patterns
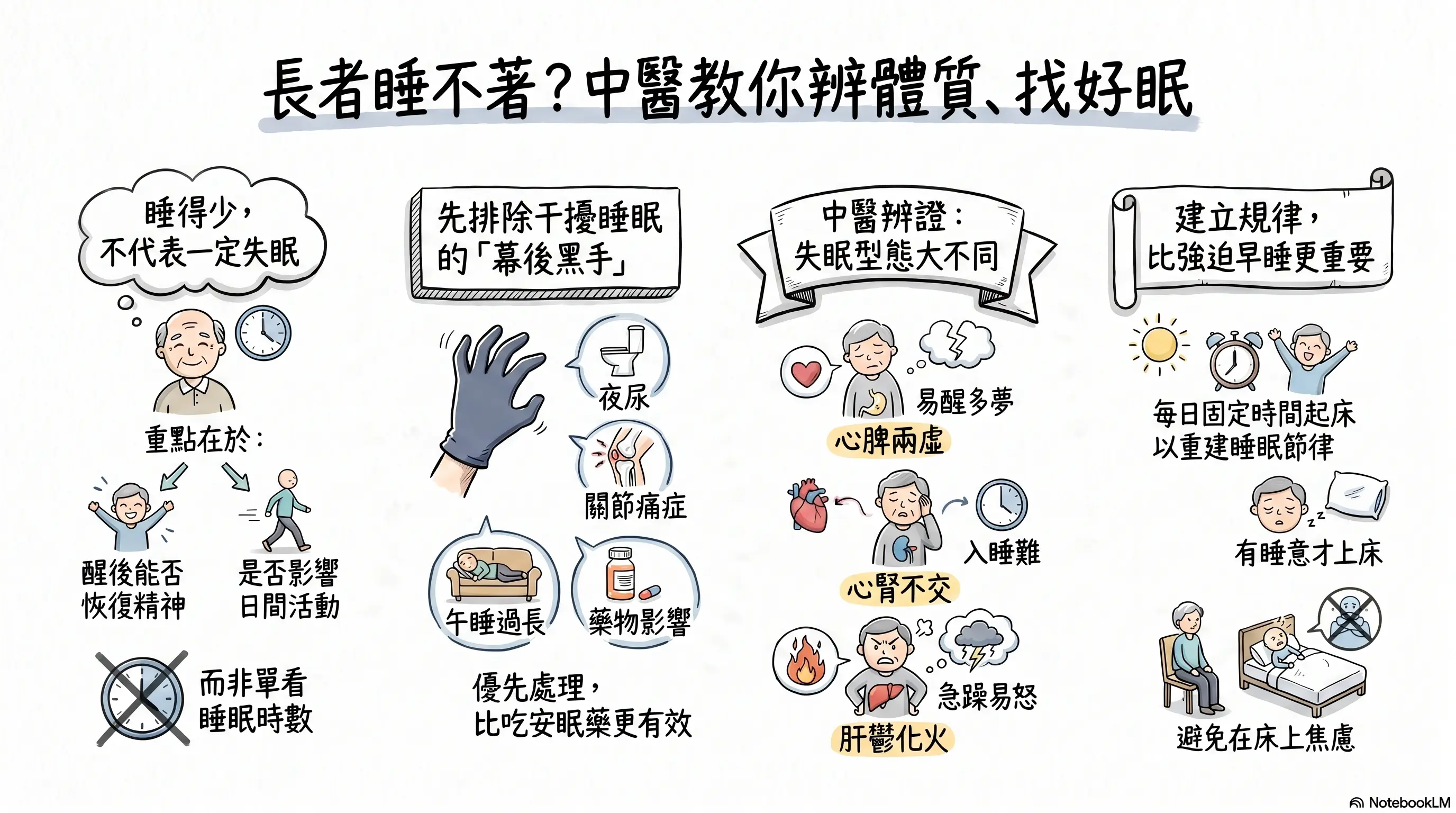 To help readers understand the topic quickly, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
To help readers understand the topic quickly, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
Many older adults feel that “sleeping less is normal with age.” Some go to bed at nine but still cannot fall asleep by midnight. Some wake several times in the night and find their minds becoming more active. Others wake at four or five in the morning and then feel tired, heavy-headed, or forgetful during the day.
Sleep does change with age. Total sleep time may shorten, light sleep may increase, and older adults may wake more easily to noise. But these changes do not automatically mean insomnia. What truly deserves attention is when sleep problems begin to affect daytime energy, mood, activity, or safety.
This article explains how to tell whether shorter sleep is still within normal ageing, which physical problems may keep insomnia recurring, how TCM differentiates different sleep patterns, and when Western medicine or specialist review should come first.
Sleeping Less Does Not Automatically Mean Insomnia
Some older adults actually get enough total sleep, but go to bed too early or nap too long in the day, so they do not feel sleepy enough at night. Others are inactive during the day, spend too long lying awake in bed, and become more anxious the more they try to force sleep.
Situations that deserve closer assessment include:
- Difficulty falling asleep on a regular basis despite lying in bed for a long time
- Waking in the night and struggling to fall back asleep
- Waking very early in the morning and then feeling tired or low in mood
- Vivid dreams, palpitations, or startling awake that affects daytime function
- Waking because of nocturia, pain, cough, bloating, or breathing problems
- Long-term reliance on sleeping pills, alcohol, or self-bought sleep products
The key point is not simply the number of hours slept, but whether a person feels restored in the morning and whether daytime life is being affected.
Common Causes of Insomnia in Older Adults: Not Just “Too Much Heat”
Insomnia is often caused by several factors at once. If someone tries to manage it only with a calming tea or tonic, the real triggers may be missed.
| Common trigger | Possible presentation | Main direction |
|---|---|---|
| Unstable sleep habits | Going to bed too early, long naps, low daytime activity | Fix waking time and reduce long daytime sleep |
| Nocturia | Waking to pass urine and then failing to fall back asleep | Assess the cause of nocturia and fall risk too |
| Pain conditions | Knee pain, back pain, neck or shoulder pain disturbing turning in bed | Address pain and sleeping posture |
| Emotional stress | Worrying about family, money, or health, with more thoughts at night | Review anxiety, low mood, and life stress |
| Medication or stimulants | Tea, coffee, alcohol, or medicines affecting alertness | Do not stop medication by yourself; ask the doctor first |
| Sleep apnoea | Loud snoring, pauses in breathing, severe daytime sleepiness | Consider Western medical or sleep review |
| Cognitive or psychiatric change | Reversed day-night pattern, confusion, hallucinations, major mood change | Seek medical assessment promptly |
This is why TCM assessment of insomnia also starts by clarifying these background factors. If nocturia, pain, breathing, or emotional distress is not addressed, “calming the mind” alone may not be enough.
How Does TCM Understand Insomnia?
In TCM, insomnia is described as “bu mei,” a state in which the mind is not settled and yin and yang do not alternate smoothly. The spleen, stomach, liver, kidney, qi, and blood may all influence the ability to sleep. Different insomnia patterns call for different treatment directions.
| TCM pattern | Common presentation | Main treatment focus |
|---|---|---|
| Heart-spleen deficiency | Easy waking, many dreams, palpitations, forgetfulness, pale complexion, fatigue, poor appetite | Tonify qi, strengthen the spleen, nourish blood, calm the mind |
| Disharmony between heart and kidney | Difficulty falling asleep, irritability, dry mouth, low back weakness, tinnitus, nocturia | Nourish yin, clear deficiency heat, reconnect heart and kidney |
| Liver depression transforming into fire | Difficulty sleeping, irritability, bitter taste, chest or rib-side tightness, pressure | Soothe the liver, relieve stagnation, clear heat, calm the mind |
| Phlegm-heat disturbing internally | Bloating, phlegm, head heaviness, sticky or bitter mouth, restless sleep | Resolve phlegm, clear heat, harmonise the stomach, calm the mind |
| Heart-gallbladder qi deficiency | Easy startling, timidity, tension, light sleep | Support qi, settle fright, calm the spirit |
The same complaint of “easy waking” may come from heart-spleen deficiency, or from nocturia, pain, or anxiety. The value of TCM is that it places insomnia back into the context of the whole body rather than asking only, “Can you sleep or not?”
When Should Western Medicine or Specialist Review Come First?
The following situations should not rely on TCM alone:
- Severe long-term insomnia with obvious low mood, hopelessness, or self-harm thoughts
- Loud snoring, suspected breathing pauses during sleep, or marked daytime sleepiness
- Sudden insomnia with rapid heart rate, chest pain, breathlessness, tremor, or rapid weight loss
- A sudden reversal of day and night, confusion, hallucinations, or major behavioural change in an older adult
- Significant night-time safety problems related to falls, pain, nocturia, or dizziness
- Long-term use of sleeping pills, sedatives, painkillers, or multiple medications
Sleeping pills, anti-anxiety medicines, or psychiatric medicines should never be changed or stopped without medical supervision. TCM may support the body’s overall state, but medication changes remain the responsibility of the primary doctor.
Seven Sleep Habits Older Adults Can Start With
-
Keep a fixed waking time
This matters more than trying to force an early bedtime. A regular waking time helps rebuild sleep rhythm gradually. -
Go to bed only when sleepy
If you lie awake in bed for a long time, get up and do a quiet low-stimulation activity, then return to bed when sleepy again. -
Keep naps short
If a nap is needed, keep it brief and avoid sleeping so late in the day that night-time sleep drive is lost. -
Stay active in the day
Walking, simple stretching, tai chi, or older-adult exercise can help rebuild sleep pressure and stabilise mood. -
Reduce tea, coffee, and alcohol later in the day
Many older adults become more sensitive to caffeine. Strong tea, coffee, and alcohol can all make sleep lighter. -
Address nocturia and pain at the same time
If the person is waking mainly because of urination or pain, insomnia is the result, not the only issue. -
Do not self-prescribe calming tonics
Older adults with hypertension, diabetes, kidney disease, blood thinners, or multiple medications should check with a practitioner before using Chinese patent medicines, medicinal wine, or supplements.
How Does Aspira TCM Assess Insomnia in Older Adults?
At Aspira TCM, Dr Chan first reviews the pattern of insomnia: difficulty falling asleep, frequent waking, vivid dreaming, early waking, or waking tired. The doctor also asks about nocturia, pain, appetite, bowel habit, emotions, blood sugar and blood pressure, cognition, medication use, and daytime activity.
If TCM treatment is suitable, herbs, acupuncture, ear acupoints, or lifestyle advice may be considered according to the constitution pattern. The goal is not to label every older adult with insomnia as having “heart fire,” but to determine whether the picture fits heart-spleen deficiency, disharmony between heart and kidney, liver fire, phlegm-heat, or a mixed situation.
If you or an older family member has long-term insomnia, frequent waking, vivid dreams, or daytime fatigue, a 7-day record of sleep, nocturia, pain, and tea or coffee intake can be useful before a TCM review. If the doctor suspects sleep apnoea, psychiatric illness, medication risk, or cognitive decline, Western medical assessment may also be recommended.
Related reading:
- Is Frequent Night Urination in Older Adults Normal? →
- Memory Problems vs Dementia: 6 Early Warning Signs and Prevention →
- TCM vs Sleeping Pills: Which Comes First for Insomnia? →
FAQ — Insomnia in Older Adults
Q1: Is sleeping less always a problem in older adults?
Not necessarily. Sleep patterns change with age, and not every older adult needs eight hours. If the person still wakes feeling reasonably restored and daytime life is not affected, there may be no major problem. But persistent fatigue, low mood, poorer concentration, or increased fall risk should be assessed.
Q2: Does insomnia simply mean “too much heat,” so cooling herbal tea should help?
Not necessarily. Insomnia may relate to heart-spleen deficiency, disharmony between heart and kidney, liver fire, phlegm-heat, heart-gallbladder qi deficiency, nocturia, pain, sleep apnoea, or medication effects. Self-prescribing cooling drinks is not always suitable, especially in older adults with weak digestion.
Q3: Can TCM treatment for insomnia conflict with sleeping pills?
It needs individual review. Bring all medication names and timing to the consultation so the practitioner can judge whether herbs or acupuncture are appropriate, and whether any timing separation is needed. Do not stop sleeping pills by yourself.
Q4: If I wake in the night, should I exercise to make myself tired again?
No. Vigorous exercise at night may make the mind more alert. A better approach is to leave the bed, do a calm low-stimulation activity, and return when sleepiness comes back.
Q5: Is insomnia related to dementia?
Poor sleep can make memory and concentration worse during the day, but that does not automatically mean dementia. If sleep difficulty is accompanied by repeated questioning, forgetting to turn off the stove, getting lost, medication confusion, or decline in everyday function, further assessment should be arranged.
Disclaimer: This article is for health education only and does not replace individual consultation, investigation, medication advice, or treatment planning. If insomnia is accompanied by severe low mood, self-harm thoughts, suspected sleep apnoea, sudden confusion, chest pain, breathlessness, or ongoing use of sleeping pills and multiple medications, seek medical advice promptly. Any medication change should only be made after consulting the primary doctor.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Overthinking and Sleepless Nights — Ms Lee's TCM Journey to Restful Sleep
A female office worker in her 30s struggled with difficulty falling asleep, frequent dreaming, and waking easily due to chronic work stress and anxiety. After six sessions over four weeks combining herbal medicine and acupuncture prescribed by Dr To, her sleep quality improved significantly and she regained her energy and quality of life.

Insomnia: Sleeping Pills or TCM? An Honest Comparison of Both Approaches
Sleeping pills offer immediate relief but carry dependency risks; TCM treats insomnia at the root but requires patience. This article honestly compares both approaches — benefits, risks, costs, and who each is best suited for — to help you find the right solution for your sleepless nights.

A Self-Check Guide to 4 Types of Menstrual Pain and Relief Tips
Menstrual pain is not something you simply have to endure. This guide explains the difference between primary and secondary dysmenorrhea, outlines four common TCM patterns, highlights five warning signs that need medical review, and offers practical relief strategies for everyday care.