Night-Time Itchy Skin in Older Adults: A TCM Damp-Heat Case Study
When spring and summer arrive, many elderly people see their itchy skin flare up, particularly at night, and topical creams alone become less effective. Through the composite case of "Madam Chan", a 78-year-old, this article explains how TCM assesses elderly itch through the lens of damp-heat in the skin and blood-deficiency wind, walks through a phased approach to relief, and lists the warning signs (scabies, drug eruption, severe skin disease) that need a Western dermatology or internal-medicine assessment first.
Medical review: Dr. Tai Wai Ho, Samson,Registered Chinese Medicine Practitioner #008702
1-Minute Quick Answer
Night-worse itchy skin in older adults often barely responds to creams; TCM treats it as surface damp-heat and root blood-deficiency wind. Through a composite case ("Madam Chan", 78; reviewed by Dr Tai, CMCHK 008702), it covers a phased clear-heat-and-nourish-blood plan, lukewarm bathing, prompt moisturising, and the warning signs that need a Western doctor first.
Night-Time Itchy Skin in a 78-Year-Old in Spring/Summer: A TCM Case Study on Damp-Heat, Blood-Deficiency Wind and Home Care
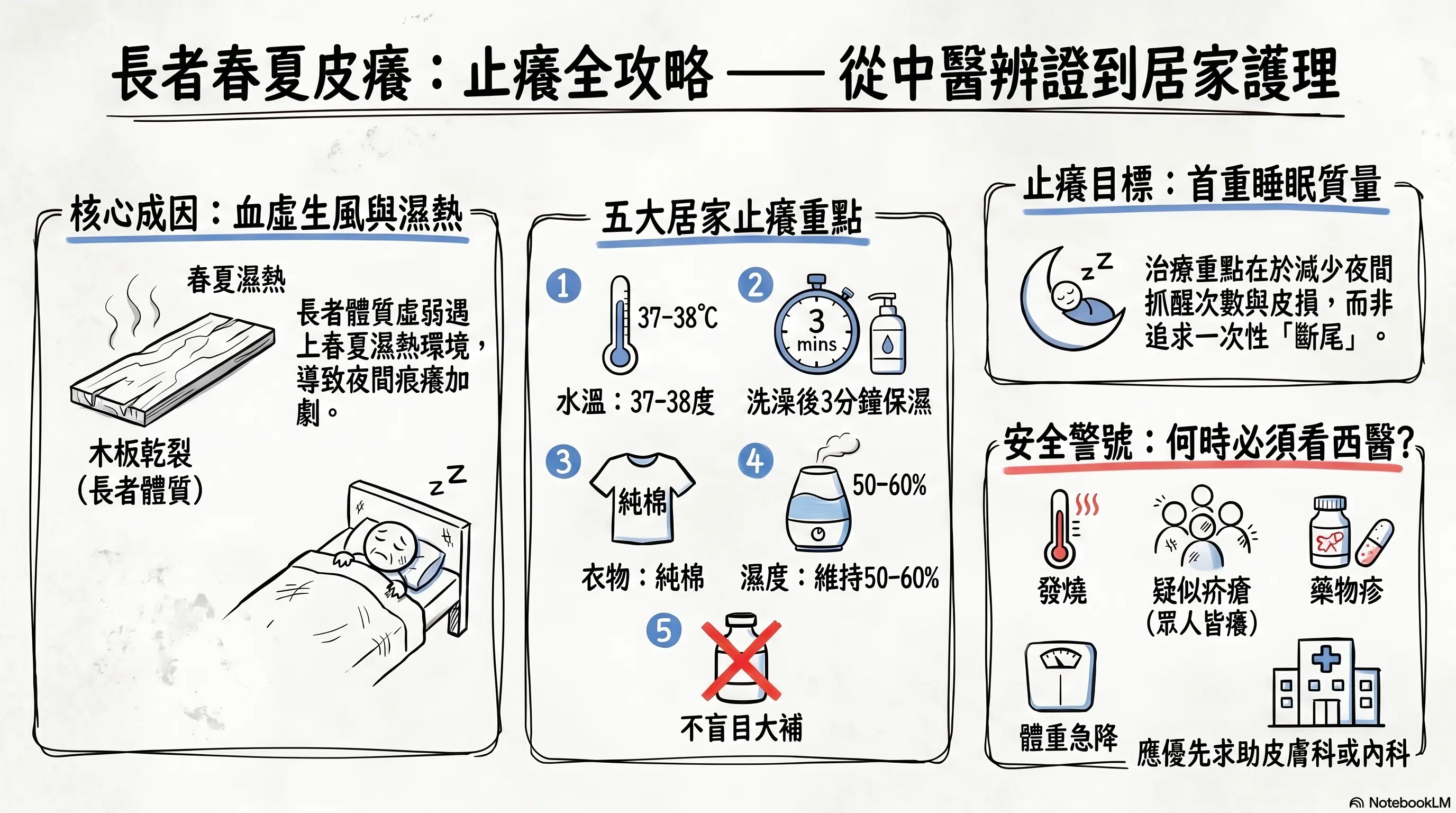 For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
Medical review: Dr Tai Wai-ho (CMCHK 008702; internal and external medicine, dermatology, men's health, gastroenterology, cough)
"As soon as spring and summer arrive, my mother-in-law scratches all night until the skin breaks — the back of her hands, her shins and her lower back are covered with red marks. Topical cream helps for three days and then the itching is back; sometimes she just cannot sleep." This was the question Madam Chan's family put to Dr Tai at Aspira TCM Clinic. (Madam Chan is a pseudonym; her case is a composite drawn from a common clinical pattern.)
Madam Chan is 78 and lives with her son and daughter-in-law. Most meals are home-cooked, with the occasional yum-cha outing. Her skin has flared every spring and summer for years, but this season was clearly worse. The family describes the itch as concentrated on the back of the hands, forearms, fronts of the shins and lower back; mild during the day, sharply worse from dusk through the night, peaking at 1–3 a.m.; the skin is dry, with scratch marks and patches of post-inflammatory pigmentation. She is woken up scratching 4–5 times a night, with poor daytime energy and reduced appetite. She has used two mid-strength topical steroid creams and a sedating night-time antihistamine — initially helping for three days, then only one. Her co-morbidities include hypertension, pre-diabetes and mild knee osteoarthritis; she takes antihypertensives, calcium and vitamin D. She bathes twice a day with hot water and a strong cleanser; the living room and bedroom run air-conditioning constantly with windows closed. The family worried whether this was "blood-damp" or "liver wind" — but feared that tonifying foods would only add heat. They booked an assessment instead.
Why Does It Get Worse Every Spring and Summer?
At first visit, Dr Tai noted a slightly red tongue with a thin, slightly greasy yellow coating; a wiry, fine and slightly rapid pulse; a dry, scratched skin without the classic scabies pattern of other household members itching at night; a dry stool every two days; and a diet leaning towards stewed soups, with cooling herbal teas favoured in summer.
The pattern was assessed as blood-deficiency wind as the root, with damp-heat in the skin as the surface manifestation, peaking in spring and summer. The skin barrier is already thin and the body fluids depleted in old age; spring–summer damp-heat from the environment, combined with constant air-conditioning that further dries the skin, leaves the body unable to nourish and moisten the skin properly. The result is "blood-deficiency wind" itch, particularly intense at night. In everyday terms: the skin is like a dry wooden floorboard that is then exposed to muggy weather and a dehumidifying air-conditioner — the cracks recur. The remedy is not just oil (nourishing blood and moistening dryness) and not just drying (clearing heat and resolving damp). Both must be done together.
Common TCM Patterns
Elderly spring-summer itch often involves a mix of the following patterns:
| Pattern | Common features | Treatment focus |
|---|---|---|
| Damp-heat in the skin | Reddened skin, exudate, bitter taste, yellow greasy tongue coating | Clear heat and resolve damp; avoid premature heavy tonifying |
| Blood-deficiency, wind-dryness | Dry, flaking skin, night-worse itch, pale tongue | Nourish blood, moisten dryness, settle wind to relieve itch |
| Yin-deficiency with internal heat | Dry mouth, nocturia, "five-centre heat", red tongue with thin coating | Nourish yin and clear heat, with cooling-blood support |
| Heart-vexation, blood-heat | Itch worse with emotion, restless mind, insomnia | Clear heart-fire, cool blood, calm the spirit |
Madam Chan presented with damp-heat in the skin, blood-deficiency wind-dryness and heart-vexed insomnia at the same time — a fairly typical mid-to-late-stage elderly itch profile, which neither pure heat-clearing nor pure tonifying can address.
Treatment Plan and Two-Month Observation
Dr Tai built a three-phase plan around the pattern. Phase 1 (weeks 1–3) balanced clearing damp-heat and nourishing blood while moistening dryness, supported by herbal washes or compresses. The family was asked to lower bath-water temperature to 37–38 °C, switch to a low-irritation cleanser, and keep each bath to 5–10 minutes. The previously prescribed antihistamine and topical steroid continued under Western-medicine guidance. Phase 2 (weeks 3–6) strengthened the blood-nourishing, dryness-moistening focus, with whole-body moisturiser applied within three minutes after bathing; clothing switched to pure cotton; less direct air-conditioning on the skin; and a discussion with the Western doctor about whether topical steroid frequency could be reduced. Phase 3 (from week 7) consolidated with blood-nourishing, spleen-strengthening, yin-nourishing and dryness-moistening care, building a year-round routine for bathing, moisturising, clothing, air-conditioning and sleep. As tolerated, acupuncture was added — along Xuehai, Sanyinjiao, Hegu, Quchi and similar points — to support itch relief and calm the spirit.
Observations after two months (qualitative): scratching-awakenings dropped from 4–5 times a night to 1–2; longest continuous sleep extended from 1–2 hours to 4–5 hours; scratch marks reduced markedly with no new flare-ups; appetite and mood improved together; topical steroid use was gradually reduced under Western-medicine guidance. Dr Tai's reminder: elderly itch is a chronic condition; the first goal is to reduce skin damage and night-time sleep disruption, not to eliminate the itch in one stroke.
Dr Tai's clinical observation: "Elderly itch may look like 'just a skin issue', but it is also tied to medication, the home environment, bathing habits, sleep, nutrition and emotion. Tonifying alone, or clearing heat alone, often will not work. Our aim is to rule out serious causes first, then handle the rest in layers."
── Dr Tai Wai-ho | Registered TCM practitioner, registration number 008702
What Families Most Often Overlook
In practice, families often focus on "which cream is best" or "which soup to drink", and miss the environmental factors that shape elderly itch most:
- Keep bath water lukewarm. Use 37–38 °C water; bathe no more than 1–2 times a day, 5–10 minutes each time; switch to a low-irritation, fragrance-free, slightly acidic cleanser.
- Moisturise immediately after bathing. Within three minutes of towelling dry, apply moisturiser over the whole body.
- Avoid direct air-conditioning and consider humidifying. Use a humidifier where appropriate; keep the bedroom at 50–60% relative humidity.
- Switch to loose pure cotton clothing. Avoid wool, blended fabrics and rough fibres; keep nails trimmed and filed smooth.
- Eat moderately. Reduce very hot, very spicy and very oily foods; avoid heavy "tonifying" diets.
These adjustments matter as much as the herbs — without the home conditions improving, herbal medicine alone struggles to keep things stable.
When Western Dermatology or Internal Medicine Must Take Over
The following are red flags that need a dermatologist or internist first; do not treat them as ordinary "elderly itch":
- Pustules, crusting, obvious infection or fever on the skin
- Multiple household members itching at the same time, particularly at night and in the finger webs, wrists, axillae or buttocks (suspected scabies)
- Sudden onset of itch with widespread rash, possibly linked to a new medication (suspected drug eruption)
- Itch with jaundice, severe fatigue or rapid weight loss (possible liver, gallbladder, thyroid or lymphatic involvement)
- Itch with prominent vesicles, heavy exudate or skin sloughing (severe eczema or acute skin disease)
- Redness, warmth or pus over a scratch site (suspected bacterial infection)
TCM assessment and care are about support, not replacement. For any suspected infection, drug eruption or systemic disease, the first step is always Western medicine.
How Aspira TCM Clinic Approaches Elderly Spring/Summer Itch
At the first visit, Dr Tai asks elderly itch patients to bring along: the Western prescription list (topical steroids, antihistamines, oral anti-itch drugs); chronic-disease records and recent investigations; a list of all creams and moisturisers tried in the past (photos help); the patient's daily bathing time, water temperature and frequency; and the home air-conditioning and humidification setup. Based on pattern differentiation, the doctor decides on the herbal and topical wash direction, and adds acupuncture as needed for itch relief and sleep. The whole programme is built around supporting Western medical care and is never marketed as "instant relief" or "permanent cure".
FAQ
1. Is elderly itchy skin always "blood-deficiency wind"?
Not always. Damp-heat, blood deficiency, yin deficiency, spleen deficiency and heart-vexation patterns commonly co-exist. A TCM assessment looks at the skin appearance, tongue and pulse, bowel and urine, sleep and emotion together.
2. Can the family brew their own damp-clearing soups or cooling herbal teas to relieve itch?
Self-prescribing is not advised. Older adults often present with a deficiency–excess overlap; aggressive damp-clearing or tonifying too early can make the itch worse. Some cooling herbal teas may bring short-term relief, but the elderly often lean towards cold-deficient constitutions, and long-term use frequently brings on diarrhoea and reduced appetite. A registered TCM practitioner should assess the constitution first.
3. Should "trigger foods" (fish, prawns, eggs) all be avoided?
Not blanket-avoided. Older adults already tend to under-eat protein, and indiscriminate dietary restriction undermines nutrition and the skin barrier. Observe whether specific foods clearly correlate with flare-ups, then adjust accordingly.
4. Are antihistamines and sleeping pills safe for the elderly?
Some traditional antihistamines (especially the night-time forms) are sedating and increase fall risk; newer-generation antihistamines are far less so. Long-term sleeping-pill use in older adults also carries fall and cognitive risks. Any change in medication must be made by the prescribing doctor; the better first step is to address the source of the itch and the home environment, and to consider short-term sleep aids only afterwards.
5. Does acupuncture help with itch?
Some elderly patients feel a relaxation effect and short-term relief; individual responses vary. Acupuncture's role is to support herbal treatment and lifestyle adjustment — not to relieve itch on its own.
Related reading:
- Breaking Free from Steroid Dependence — An Eczema Recovery Story →
- Eczema Diet Guide — TCM Tips on Triggers, Foods to Avoid & Daily Care →
- Complete TCM Guide to Eczema Treatment →
Disclaimer: This article is for general health education only and does not replace individual diagnosis, dermatological evaluation or treatment. The case is a composite anonymous scenario, not a single real patient. For widespread rash, fever, skin infection, suspected drug eruption, suspected scabies or any concurrent systemic symptoms, see a Western doctor or dermatologist immediately.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Eating Light but Not Losing Weight? A TCM Edema-Type Case Study
Eating light yet the scale will not budge — only the puffiness in the face, ankles and waistline persists? This case study follows Ya-lin (pseudonym), a 38-year-old office worker, through six months and explains how "eating clean but still not losing weight" often comes from a stack of small issues: salt, low protein, constipation, premenstrual fluid retention, phlegm-damp constitution, or internal disease. It also lists scenarios that warrant seeing a Western doctor first.

Overthinking and Sleepless Nights — Ms Lee's TCM Journey to Restful Sleep
A female office worker in her 30s struggled with difficulty falling asleep, frequent dreaming, and waking easily due to chronic work stress and anxiety. After six sessions over four weeks combining herbal medicine and acupuncture prescribed by Dr To, her sleep quality improved significantly and she regained her energy and quality of life.

Two Months of Coughing, Relief in Three Sessions — Mr Chan's Story
A male office worker in his 40s suffered from persistent coughing for over two months with no improvement from Western medication. After three sessions of herbal medicine prescribed by Dr Tai, his cough significantly improved and he regained normal work and sleep.