Weak Limbs and Reduced Grip Strength Are Not Just Ageing: A TCM Guide to 6 Warning Signs of Sarcopenia, Testing and Prevention
If you or an older family member has weaker limbs, poorer grip strength, slower walking, or more frequent falls, it may not be ageing alone. This guide explains common causes of sarcopenia, the risks it brings, how to screen for it, and how exercise, protein intake, and early assessment may help reduce muscle loss.
Medical review: Dr. Wong Ka Fai,Registered Chinese Medicine Practitioner #009985
Weak Limbs and Reduced Grip Strength Are Not Just Ageing: A TCM Guide to 6 Warning Signs of Sarcopenia, Testing and Prevention
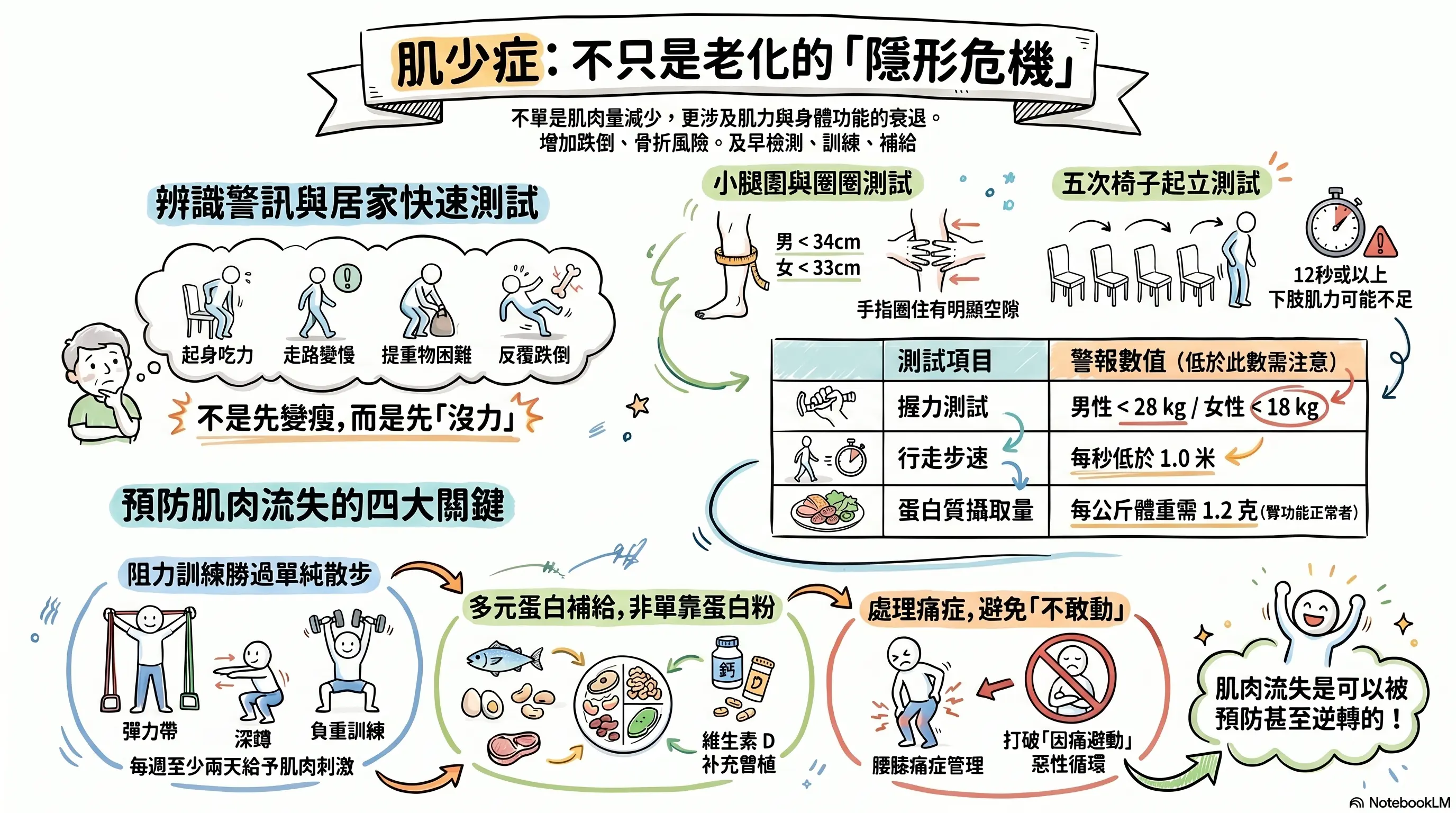 To help readers grasp the content quickly, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
To help readers grasp the content quickly, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
If you or an older family member has recently become weaker in the limbs, slower to stand up, slower to walk, or more prone to falling, it may not be ageing alone. These changes can be related to sarcopenia.
Sarcopenia is not defined simply by whether someone looks thin. Some people do not appear underweight at all, and may even look overweight, yet their muscle mass has already fallen and their daily function is declining. The real question is not body weight, but whether a person has become less able to generate force, keep balance, and manage ordinary life.
This article explains four practical things: how sarcopenia develops, what risks it brings, how it can be screened for, and what can be done in daily life to reduce further decline.
Why Is It Not Just “Normal Ageing”?
Muscle does naturally decline with age. NIH has noted that people may lose around 3% to 5% of muscle mass per decade from around the age of 30. CUHK Medical Centre also notes that muscle mass may decline by about 1% per year after 30, and faster after 50. The issue is not muscle loss alone, but when it comes together with weaker strength, slower gait, more difficulty standing up, and poorer balance.
From a TCM point of view, this is not treated as “inevitable ageing” alone. In practice, several factors often appear together: long periods of sitting, reduced movement, weakness after illness, poor digestion and absorption, chronically poor appetite, or pain in the low back, knees, or bones that causes further inactivity. In other words, sarcopenia usually has more than one cause. Age, activity level, nutrition, and chronic illness may all reduce the body’s reserve at the same time.
A key point: many people do not first become visibly thin. They first become weaker, slower, and more afraid of falling.
Six Common Causes of Sarcopenia
| Common cause | What you may notice | What clinicians pay special attention to |
|---|---|---|
| Ageing and hormonal change | Lower stamina, slower walking, poorer recovery | Whether decline is accelerating beyond expected ageing |
| Long periods of sitting and lack of resistance training | Difficulty standing up, trouble climbing stairs, easy fatigue | Whether work pattern, retirement, or lack of strength stimulus is driving decline |
| Pain leading to avoidance of movement | Less activity after low back pain, knee pain, or neck and shoulder pain | Whether pain-avoidance is steadily weakening the lower limbs and core |
| Low protein or poor overall nutrition | Poor appetite, rapid weight loss, marked weakness after illness | Whether the person has long been eating too little, or has chewing or swallowing difficulty |
| Hospitalisation, surgery, or prolonged bed rest | Slower rising, unsteady walking, easy breathlessness after discharge | Whether function and muscle have fallen rapidly over a short period |
| Chronic illness or obesity with low muscle mass | Not necessarily thin in appearance, but increasingly weak | Whether diabetes, inflammation, metabolic issues, or sarcopenic obesity is present |
What Risks Does Sarcopenia Bring?
Sarcopenia directly affects daily function. When muscle mass and muscle strength decline together, common consequences include:
- Greater risk of falling, and greater risk of fracture after a fall
- More difficulty standing up, walking, carrying things, and climbing stairs
- Lower activity capacity and poorer independent living ability
- Slower recovery after illness, with higher risk of admission or readmission
- Links to frailty, osteoporosis, metabolic problems, and even higher mortality risk
CUHK Medical Centre notes that sarcopenia can increase the risks of falls, fractures, poorer mobility, osteoporosis, and pneumonia. NIH also links it to falls, hip fractures, limited activity, and hospitalisation. Do not wait until a person is no longer able to walk. The right time to pay attention is when function first starts to fall.
How Can You Screen for Sarcopenia Risk?
Sarcopenia cannot be judged by appearance alone, and certainly not by looking at one photo of the legs. In Asia, early screening usually considers strength, physical performance, and muscle mass together.
| Test | What it mainly assesses | When to be more alert |
|---|---|---|
| Self-observation | Whether standing up is harder, walking is slower, falls are more common, or lifting becomes harder | When the changes last for weeks or are progressively worsening |
| Calf circumference or finger-ring test | Whether calf muscle has clearly declined | Calf circumference below 34 cm in men or 33 cm in women, or a clear gap when the fingers encircle the widest part of the calf |
| Grip strength | Overall upper-limb strength | Below 28 kg in men or 18 kg in women |
| Five-times chair stand test | Lower-limb strength and sit-to-stand function | Taking 12 seconds or longer to complete five repetitions |
| Six-metre gait speed | Walking speed and functional performance | Slower than 1.0 metre per second |
| BIA or DXA muscle mass measurement | Whether true low muscle mass is present | When screening is abnormal or further confirmation is clinically needed |
One important reminder: one abnormal result does not mean you can diagnose yourself with sarcopenia. But if grip strength, walking speed, chair-stand speed, or calf size is showing warning signs, a fuller assessment is worthwhile.
What Are Functional Movement Tests Really Looking At?
These tests are not about diagnosing based on a single movement. They are mainly looking at whether lower-limb strength is adequate, whether sit-to-stand transitions are smooth, whether the centre of gravity is controlled well, and whether balance has already started to decline.
In other words, these tests measure day-to-day function. Before many people realise they are losing muscle, they often say things like: “I am slower getting up recently”, “my walking is not as steady as before”, “stairs tire me out”, or “my legs feel weak if I stand too long”. This is why proper assessment usually combines grip strength, walking speed, chair-rise testing, and sometimes direct muscle-mass measurement.
How Can Muscle Loss Be Slowed? Protein, Resistance Training, and Balance All Matter
1. Walking alone is not enough — strength training matters
Walking is useful, but if the goal is to prevent sarcopenia, walking alone is usually not enough. CDC guidance for older adults recommends at least 150 minutes of moderate aerobic activity per week, plus muscle-strengthening activity on at least two days per week, along with balance training. For sarcopenia, resistance training is especially important because it directly affects muscle strength and retention.
Simple starting options include resistance bands, wall-supported squats, sit-to-stand training, water-bottle weights, and leg raises. The key is not doing too much at once, but giving muscles repeated stimulation over time.
2. Protein intake matters, but not only protein powder
If intake remains too low, or appetite is poor after illness, muscle is hard to preserve. CUHK Medical Centre notes that older adults with normal kidney function may aim for around 1 to 1.2 g of protein per kilogram of body weight per day. For a 60 kg person, that means about 60 to 72 g of protein daily.
Protein does not have to come only from supplements. Fish, eggs, beans, dairy, and lean meat all count. For some older adults, however, the problem is not lack of awareness, but poor chewing, swallowing problems, poor appetite, or reduced cooking ability. These barriers also need to be addressed. Calcium and vitamin D are worth reviewing at the same time.
3. When pain is present, deal with why the person is afraid to move
Many people are not inactive because they are lazy, but because movement causes pain. Low back pain, knee pain, foot pain, and neck or shoulder pain all make people move less, and the less they move, the faster muscle can decline. In these cases, simply telling someone to “exercise more” is often unrealistic. A more useful approach is to identify which pain or postural problems are limiting function, then gradually rebuild activity.
4. After illness, surgery, or hospitalisation, rebuilding function should be taken seriously
CUHK Medical Centre notes that muscle loss can speed up markedly if an older adult stays in hospital for more than two weeks. After discharge, many people first notice a clear fall in stamina, slower rising, and weaker legs. If this stage is met only with rest and no active rebuilding of function, decline can easily continue.
5. Repeated falls, slower walking, or weight loss should not be ignored
The real warning sign is not just a number on a report, but functional decline. If you or a family member has been falling repeatedly, walking more slowly, struggling more to stand up, losing weight suddenly, or staying weak for a long time after illness, a full assessment is more appropriate than guesswork.
When Should Western Medical Review Come First?
This point matters. Sarcopenia can be related to ageing and reduced activity, but it can also be the surface sign of another illness. The following situations should not simply be treated as ordinary “muscle loss”:
- Sudden one-sided weakness, numbness, slurred speech, or facial drooping, where stroke must be excluded
- Rapid weight loss, very poor appetite, or swallowing difficulty over a short period
- Repeated falls together with dizziness, fainting, chest tightness, or breathlessness
- Very rapid strength decline, or decline accompanied by fever, night pain, or persistent significant pain
- Severe weakness after surgery, infection, or hospitalisation to the point that basic rising is difficult
TCM can help with recovery support, pain management, constitutional regulation, and rebuilding activity. But acute neurological, cardiopulmonary, endocrine, or other serious internal medical conditions should first be judged through Western medicine.
Doctor’s Note
Sarcopenia does not always first show up as looking thinner. More often it appears as slower rising, poorer grip strength, slower walking, and easier falling. The earlier it is recognised, the easier it is to rebuild function through training, nutrition, and early intervention.
Assessment First
If you are unsure whether you have simply “slowed down” or already have meaningful sarcopenia risk, assessment is a good starting point. At Aspira TCM, we first look at activity level, pain restrictions, nutrition, and recovery status, then explain honestly whether Western medical review should come first or whether TCM regulation and functional rebuilding are reasonable next steps.
What matters is not labelling everyone as having a problem, but helping clarify whether the main issue is strength, balance, nutrition, or overall recovery capacity.
FAQ
1. Does sarcopenia only happen in older adults?
No. Risk is higher in older adults, but muscle loss begins gradually after about the age of 30. People who are inactive, recently hospitalised, living with chronic illness, or undernourished may also develop earlier decline.
2. Is daily walking enough to prevent sarcopenia?
Not always. Walking helps with cardiovascular health and overall activity, but preserving strength usually still requires resistance training and lower-limb work such as sit-to-stand drills, resistance bands, and leg exercises.
3. Can an overweight person also have sarcopenia?
Yes. This is often called sarcopenic obesity. Body weight may not be low, but fat proportion is higher and muscle proportion is too low, so appearance alone is misleading.
4. Can protein drinks or protein powder alone improve sarcopenia?
Usually not enough. Protein matters, but if there is no activity stimulus, no resistance training, no balance training, and no attention to pain-related inactivity or post-illness weakness, the effect is often limited.
5. If I can do the chair-rise test at home, does that mean I am fine?
Not necessarily. Sarcopenia is not judged from one test alone. Grip strength, walking speed, chair-stand speed, calf size, and sometimes muscle-mass measurement all matter. Being able to complete the test does not mean risk is absent. Taking longer, feeling unstable, or performing clearly worse than before are all important signs.
Disclaimer: This article is for health education only and does not replace individual consultation, testing, or treatment advice. If you or a family member already has marked weakness, repeated falls, rapid weight loss, or other unusual symptoms, please seek medical care promptly.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Memory Lapses or Normal Ageing? TCM Explains 6 Early Dementia Warning Signs, Assessment and Prevention
Memory lapses in older adults do not always mean dementia. But when a person repeatedly asks the same question, forgets recent events, gets lost, makes mistakes with cooking, or shows clear personality changes, it should not be dismissed as ageing alone. This guide explains the differences between normal ageing and dementia, six early warning signs, common assessment methods, and how TCM may support prevention and overall function.

Feeling Tired After Meals and Waking to Urinate at Night: Are These Early Signs of Diabetes? A TCM Guide to 6 Warning Signs, Testing and Prevention
Diabetes does not always begin with dramatic symptoms. Many people notice tiredness after meals, more night urination, dry mouth, increasing abdominal fat, itchy skin, or slow wound healing before they are diagnosed. This article explains early warning signs of diabetes, who should be tested early, and how TCM may support people in the prediabetes stage.

A 75-Year-Old Mother Keeps Forgetting to Turn Off the Stove: A TCM Assessment Approach to Dementia Warning Signs
Ms Lee’s 75-year-old mother has recently begun repeating the same questions, mixing up her medication, and even forgetting to turn off the stove. Is this ordinary forgetfulness, poor sleep, or an early dementia warning sign? This article explains how TCM can assess an older adult’s memory changes step by step through the lenses of safety, cognitive function, vascular risk, sleep, constitution, and family caregiving.