Sciatica Recovery — Combined Acupuncture and Bone-Setting Treatment
A professional driver in his 50s suffered from recurring sciatica for six months that severely impacted his work. After six sessions of combined acupuncture and bone-setting treatment by Dr Wong, his pain significantly improved and he returned to work.
Medical review: Dr. Tai Wai Ho, Samson,Registered Chinese Medicine Practitioner #008702
1-Minute Quick Answer
A professional driver in his 50s suffered recurring sciatica for 6 months that crippled his work. After Dr Wong (CMCHK 009985) at Aspira TCM Lai Chi Kok delivered 6 sessions combining acupuncture and bone-setting, his pain dropped dramatically and he returned to work.
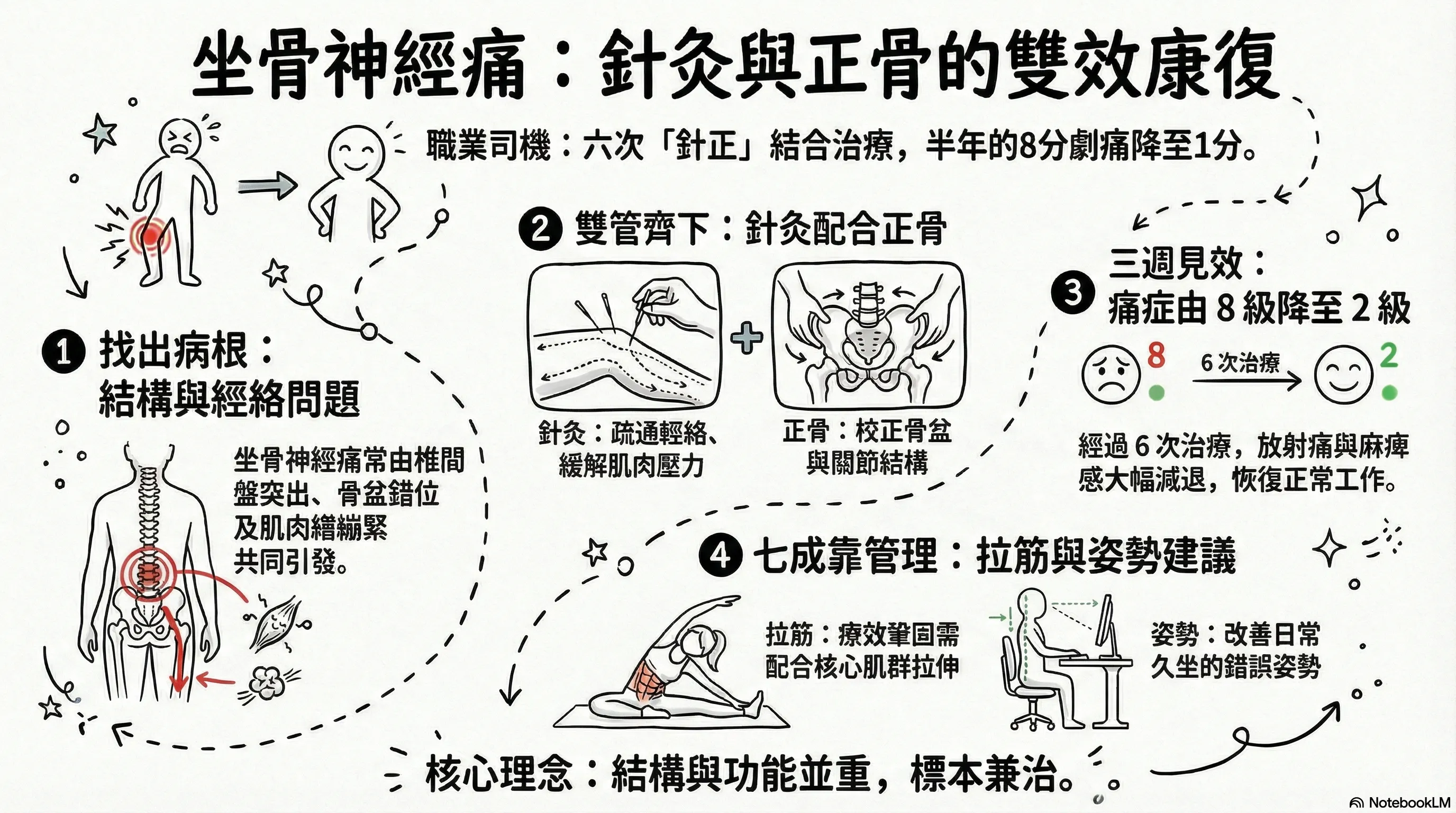 To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
Six Months of Back and Leg Pain, Almost Unable to Work
Mr Cheung (pseudonym) is a professional driver in his 50s who spends long hours sitting behind the wheel every day. Six months ago, he began experiencing pain in his right lower back. At first, he thought it was ordinary back stiffness that would resolve with rest. Instead, the pain gradually spread down the back of his right leg, radiating from the buttock all the way to the calf and sole of the foot.
This was not ordinary soreness — it was a sharp, electric-like shooting pain accompanied by numbness. Prolonged sitting made it worse, and bending, coughing, or sneezing triggered intense pain. As a professional driver who sits six to eight hours a day, the pain made it nearly impossible to complete a full day's work.
Mr Cheung consulted an orthopaedic specialist. An MRI revealed mild disc protrusion at L4-L5, compressing the right sciatic nerve. The orthopaedic surgeon recommended physiotherapy first, with surgery as a backup option if conservative treatment failed.
He underwent two months of physiotherapy, including electrotherapy and lumbar traction. The pain eased somewhat but the improvement was limited — he felt better for two or three days after each session, then the pain returned. He was reluctant to take painkillers long-term due to concerns about side effects.
A fellow driver recommended he try TCM acupuncture, having resolved his own back pain that way. Mr Cheung came to Aspira TCM with a "let's give it a try" mindset.
How Does TCM Approach Sciatica?
During the initial consultation, Dr Wong conducted a thorough physical examination and movement assessment. Beyond confirming the disc protrusion shown on MRI, Dr Wong discovered that Mr Cheung's pelvis was slightly misaligned, with restricted mobility in the right sacroiliac joint and significant tension in the lower back and gluteal muscles.
Dr Wong explained that sciatica usually has more than one contributing cause. In Mr Cheung's case, mild disc protrusion combined with pelvic misalignment was jointly compressing the sciatic nerve, and prolonged poor posture from driving was continuously aggravating the problem.
From a TCM perspective, this corresponded to "kidney deficiency affecting the Du meridian, with cold-dampness obstructing the channels." The lower back is the house of the kidneys; kidney qi insufficiency combined with cold-dampness invasion impairs qi and blood flow through the meridians — and where there is obstruction, there is pain.
Treatment needed a dual approach: bone-setting techniques to correct the pelvic misalignment and improve joint mobility, combined with acupuncture to unblock the meridians, relieve muscle tension, and reduce nerve compression.
Treatment Process: Acupuncture Combined with Bone-Setting
Dr Wong scheduled twice-weekly sessions, each approximately 45 minutes, incorporating both acupuncture and bone-setting techniques.
Sessions 1-2: Relieving Acute Pain
The first two sessions focused on acute pain relief. Dr Wong selected acupoints including Huantiao (GB30), Weizhong (BL40), Yanglingquan (GB34), and Kunlun (BL60), enhanced with electroacupuncture stimulation. This was followed by gentle bone-setting manoeuvres to make minor pelvic adjustments.
After the first session, Mr Cheung immediately felt the tightness in his back and leg ease. After the second session, he reported that the radiating pain had shortened in range — the numbness that previously reached his foot had retreated to the calf.
Sessions 3-4: Structural Correction and Meridian Clearing
From session three, Dr Wong applied targeted treatment to correct the sacroiliac joint misalignment and improve mobility in the right hip joint. The acupuncture protocol was also adjusted, adding Shenshu (BL23) and Mingmen (GV4) to tonify the kidneys and strengthen the lower back.
After session four, Mr Cheung reported that his pain level had dropped from 8/10 to roughly 3-4/10. The most noticeable change was that sitting no longer caused as much pain — he could drive continuously for three to four hours before needing a break, compared to barely one hour before treatment.
Sessions 5-6: Consolidation and Recurrence Prevention
The final two sessions focused on consolidation. Dr Wong continued acupuncture and bone-setting while teaching Mr Cheung a set of stretching exercises for the lower back and core muscles, recommending he perform them twice daily for fifteen minutes.
Given Mr Cheung's occupation, Dr Wong also provided specific driving posture advice: adjusting the seat angle, getting out to move for five minutes every ninety minutes, and using a lumbar support cushion.
Treatment Outcome
After six sessions over approximately three weeks, Mr Cheung's sciatica symptoms improved dramatically. His pain score dropped from 8/10 to 1-2/10, the radiating pain and numbness in his right leg had essentially resolved, and he was able to work normally.
At a follow-up six weeks later, Mr Cheung confirmed he had been consistently doing the stretching exercises and adjusting his driving posture as advised. The pain had not returned. Occasionally, after particularly long driving days, he would feel mild lower back stiffness, but this resolved with rest and stretching.
Dr Wong's Commentary
Sciatica is one of the most common conditions in pain management, particularly among people who sit for extended periods at work. Many patients become anxious when their MRI shows a disc protrusion, worried that surgery is inevitable. In reality, most mild to moderate disc protrusions can be managed effectively with conservative treatment.
My approach to pain management emphasises "structure and function together." Acupuncture alone for pain relief is insufficient — if structural problems such as pelvic misalignment and restricted joint mobility are not addressed, the pain will inevitably recur. Conversely, bone-setting alone without clearing the meridians yields diminished results. Combining acupuncture with bone-setting creates the best therapeutic outcome.
Another crucial factor in Mr Cheung's case was his active participation in self-management — consistently performing stretching exercises and improving his work posture. Pain treatment is not confined to the clinic. I often tell patients: treatment accounts for 30%, self-management accounts for 70%.
If you are experiencing sciatica or other lower back and leg pain, I recommend seeking treatment early rather than waiting. The sooner treatment begins, the better the outcomes tend to be.
— Dr Wong Ka-fai | Registered Chinese Medicine Practitioner (Reg. No.: 009985)
Back or Leg Pain Affecting Your Life? Book a Consultation
If you are also struggling with sciatica, lower back pain, neck pain, or other pain conditions, you are welcome to book a consultation with Dr Wong. Dr Wong specialises in treating various pain conditions using combined acupuncture and bone-setting techniques, and will provide personalised rehabilitation advice based on your occupation and lifestyle.
How to book:
- WhatsApp: Book here
- Phone: 2110 9337
- Address: Unit 2706, Saxon Tower, 7 Cheung Shun Street, Lai Chi Kok
Further reading: Complete TCM Guide to Pain Treatment →
Disclaimer: Every patient's constitution and condition are different, and treatment outcomes vary accordingly. The above case is for reference only. Please consult a practitioner for a treatment plan tailored to your specific situation. If you are experiencing severe back or leg pain, lower limb weakness, or bowel/bladder dysfunction, please seek hospital examination to rule out serious conditions before considering TCM treatment.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Night-Time Itchy Skin in Older Adults: A TCM Damp-Heat Case Study
When spring and summer arrive, many elderly people see their itchy skin flare up, particularly at night, and topical creams alone become less effective. Through the composite case of "Madam Chan", a 78-year-old, this article explains how TCM assesses elderly itch through the lens of damp-heat in the skin and blood-deficiency wind, walks through a phased approach to relief, and lists the warning signs (scabies, drug eruption, severe skin disease) that need a Western dermatology or internal-medicine assessment first.

Eating Light but Not Losing Weight? A TCM Edema-Type Case Study
Eating light yet the scale will not budge — only the puffiness in the face, ankles and waistline persists? This case study follows Ya-lin (pseudonym), a 38-year-old office worker, through six months and explains how "eating clean but still not losing weight" often comes from a stack of small issues: salt, low protein, constipation, premenstrual fluid retention, phlegm-damp constitution, or internal disease. It also lists scenarios that warrant seeing a Western doctor first.

Overthinking and Sleepless Nights — Ms Lee's TCM Journey to Restful Sleep
A female office worker in her 30s struggled with difficulty falling asleep, frequent dreaming, and waking easily due to chronic work stress and anxiety. After six sessions over four weeks combining herbal medicine and acupuncture prescribed by Dr To, her sleep quality improved significantly and she regained her energy and quality of life.