Eating Light but Not Losing Weight? A TCM Edema-Type Case Study
Eating light yet the scale will not budge — only the puffiness in the face, ankles and waistline persists? This case study follows Ya-lin (pseudonym), a 38-year-old office worker, through six months and explains how "eating clean but still not losing weight" often comes from a stack of small issues: salt, low protein, constipation, premenstrual fluid retention, phlegm-damp constitution, or internal disease. It also lists scenarios that warrant seeing a Western doctor first.
Medical review: Dr. Au Kwok Po, Arthur,Registered Chinese Medicine Practitioner #009884
1-Minute Quick Answer
Eating light yet not losing weight, while only getting puffier, is rarely just dampness; it usually stacks excess salt, low protein, constipation, prolonged sitting and premenstrual fluid retention. This composite case study of a 38-year-old woman (reviewed by Dr Au, CMCHK 009884) covers common patterns and red flags that need a Western doctor first.
Eating Light but Still Not Losing Weight? A TCM Case Study of Edema-Type Weight-Loss Difficulty in a 38-Year-Old Woman
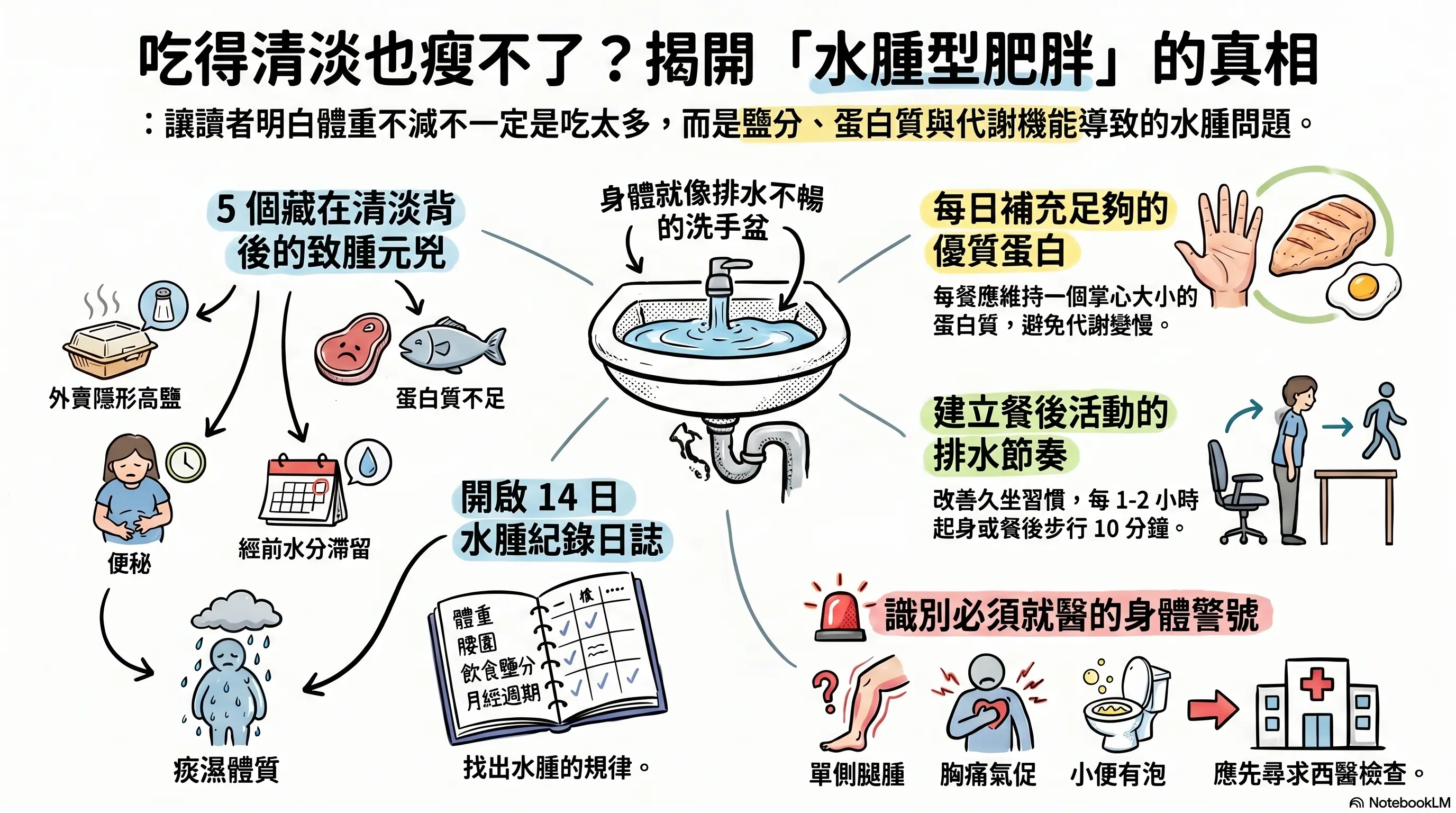 For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
Medical review: Dr Au Kwok-bo (CMCHK 009884; TCM weight management, nutrition, flu, hair loss; qualified nutritionist)
"I already eat so plainly — why is my face and ankles still puffy and the scale unmoved?" This had been Ya-lin's most frustrating question for the past six months. (Ya-lin is a pseudonym; her case is a composite drawn from a common clinical pattern.)
Ya-lin is 38, working in office administration. Her weight rose from 58 kg to 64 kg over the past six months — BMI around 25. What troubled her was not the scale itself but the sense of being "puffy all over": face swollen in the morning, shoes tighter in the afternoon, an extra kilogram added in the week before her period that would not budge. Her routine looked sensible on paper — black coffee, one egg and half a banana for breakfast; a salad or rice noodle soup takeaway for lunch with no extra sauce or rice; a low-rice, low-meat, vegetable-heavy dinner with the occasional meal-replacement shake; about 1 litre of water and one to two black coffees a day; and 30 minutes of treadmill running once or twice a week.
After two months the scale had moved 0.5 kg, with no change in waist circumference. Convinced the problem was "too much dampness", she added damp-dispelling herbal tea and cut her staples and meat further. Her bowel pattern dropped from once a day to once every two or three days; she felt dizzy and shaky in the afternoons, her periods grew lighter, and the swelling actually worsened. A friend referred her to Aspira TCM Clinic for an assessment with Dr Au.
Why Does Eating Light Still Lead to Swelling?
Dr Au's first-visit history-taking covered diet, periods, bowel habits, sleep and working pace. The "light eating" picture turned out to have important holes: takeaway noodle soups carry salty broth that pushed her daily sodium intake well above target; one egg and a small portion of shredded chicken on her salad gave her only about 0.6 g of protein per kilogram of body weight a day, plainly insufficient; bowel movement had dropped to once every two to three days; periods had become noticeably lighter over the previous six months, with worse facial and ankle swelling in the week before menstruation; sleep was 5–6 hours a day; the job kept her seated for over 8 hours; her tongue was pale with teeth marks and a slightly thick white coating.
Dr Au's working impression was that this was not "one big dampness problem" but rather a stack of overlapping issues — excess salt + insufficient protein + constipation + prolonged sitting + premenstrual fluid retention + phlegm-damp obstructing the spleen. "Light eating" had reduced oil and sugar, but the salt, protein and activity issues had not been addressed. In everyday terms: the body was a basin with a slow drain — water kept flowing in (salty takeaways; coffee triggers diuresis but also more thirst) while the outlet was blocked (constipation, low activity, premenstrual hormones holding water). It is hardly surprising the basin would not empty.
Five Common Patterns Behind "Eating Light but Not Losing Weight"
| Pattern | Common features | What to look for |
|---|---|---|
| Salt-from-takeaway | Face and ankles puffy the day after noodle soup or takeaway; weight bumps up briefly | Cuts to broth and sauces produce visible improvement within 1–2 days |
| Protein-deficient | A vegetable-heavy diet with falling muscle mass, easy fatigue, and lighter periods | Improves once eggs, soy products, lean meat and fish are added |
| Constipation-driven | Bowel movements every few days, lower abdominal fullness, waistline fluctuating with the day | Abdominal girth and bloating drop noticeably after a bowel movement |
| Premenstrual fluid retention | Weight up 1–2 kg in the 5–7 days before menstruation, breast tenderness, mood swings | Recedes gradually once menstruation begins |
| Phlegm-damp obstructing the spleen | Body feels heavy, sticky mouth, thick tongue coating, sticky stools, recurrent swelling | Linked to sweets, cold drinks, long sitting and weak spleen-stomach |
Ya-lin showed all five at once — a textbook profile of "eating light but not losing weight". The cause is rarely a single factor; rather, several smaller issues stack up. A TCM assessment looks at menstruation, bowel habits, diet, sleep and emotion together before deciding whether to strengthen the spleen, soothe the liver, moisten the bowels or first replenish qi and blood — the same "swelling" can come from dampness, qi stagnation, constipation, cyclical fluid retention, or qi-and-blood deficiency from prolonged restrictive eating.
Treatment Plan and Two-Month Observation
Dr Au designed a three-phase plan based on pattern differentiation. Phase 1 (weeks 1–3) centred on strengthening the spleen, resolving damp and reducing swelling, paired with acupuncture (along Yinlingquan, Sanyinjiao, Zusanli, Zhongwan and similar points). On the dietary side, she stopped the takeaway broth and added quality protein; she also got up to move every 1–2 hours and walked at least 30 minutes a day. Phase 2 (weeks 3–6) added a blood-nourishing, bowel-moistening direction, with one palm-sized portion of protein per meal, lower salt and sugar in the week before menstruation, and a cycle log. Phase 3 (from week 7) focused on consolidating the spleen-stomach with a sustainable dietary structure and monthly review.
Observations after two months (qualitative): morning facial puffiness eased; bowel pattern returned to once a day; period flow increased slightly; total weight dropped about 2 kg; waist circumference dropped about 3 cm. The most meaningful changes for Ya-lin, in her own words, were the energy and menstrual recovery. Dr Au's reminder: for an oedema-type body, waist circumference, body fat percentage, menstrual regularity and bowel rhythm reflect progress better than the scale.
When Swelling Should Not Be Treated as Just a Weight-Loss Issue
The following are red flags that warrant seeing a Western doctor first:
- Sudden unilateral calf pain, redness or warmth
- Swelling with chest pain, shortness of breath, inability to lie flat or fainting
- Markedly reduced urine output, foamy urine or blood in the urine
- A rapid increase in weight with prominent facial and ankle swelling
- Pre-existing cardiac, renal, liver or thyroid disease, or current use of diuretics or antihypertensives
- Sudden swelling, headache or rising blood pressure during pregnancy
- Constipation with blood in stool, black stool, persistent abdominal pain, vomiting or unexplained weight loss
TCM cannot replace cardiac, renal, hepatic, thyroid or obstetric–gynaecological evaluation. If an internal or emergency condition is suspected, see a Western doctor or attend the emergency department immediately.
Three Practical Things You Can Do Now
- Keep a 14-day swelling log. Record weight, waist, location of swelling, bowel movement, menstruation and takeaway meals on the same chart, so you can tell whether the swelling is premenstrual, post-takeaway or non-patterned.
- Reset salt intake without cutting whole meals. Reduce broth, sauces, processed meats and ready-to-eat foods, while still keeping protein and vegetables; aim for one palm-sized protein portion per meal.
- Tackle constipation first and build an activity rhythm. Increase fluids, fibre and a moderate amount of healthy fats; avoid long-term reliance on damp-dispelling teas; get up to move every 1–2 hours and walk for 10–20 minutes after meals.
How Aspira TCM Clinic Approaches Edema-Type Weight-Loss Difficulty
We will go over the location and timing of swelling, your menstrual cycle, bowel habits, dietary salt, takeaway frequency, sleep, stress, weight and waist measurements, and tongue and pulse. Dr Au will distinguish between spleen-deficiency-with-damp, phlegm-damp, qi stagnation with fluid retention, constipation, and qi-and-blood deficiency. Where TCM can reasonably help, the plan may include Chinese herbal medicine, acupuncture, ear-acupressure, dietary adjustment and lifestyle changes. Where there is concern about the heart, kidneys, liver, thyroid, unilateral swelling or pregnancy red flags, we will recommend Western medical investigations first.
If you have been "eating light but still not losing weight", consider keeping a 14-day swelling log first, then booking an assessment for spleen-stomach and oedema-type weight management.
FAQ
1. Why does the scale not move even when I eat plainly?
"Light" does not equal "nutritionally complete" — and certainly does not equal "low salt". Soup bases, sauces and processed foods are high in sodium; cutting protein too far reduces muscle mass and slows metabolism; sustained low-calorie eating leads to qi-and-blood deficiency, lighter periods and worse swelling.
2. Does swelling always mean too much dampness?
Not always. It can be linked to salt, the menstrual cycle, constipation, sleep, medication or internal disease. TCM differentiates between phlegm-damp, spleen deficiency, qi-stagnation-with-fluid-retention and qi-and-blood deficiency, and decides accordingly whether dampness needs to be cleared.
3. Is gaining 1–2 kg before a period normal?
For some women, premenstrual fluid retention, bloating and appetite changes raise weight, which usually settles after menstruation begins. If the swelling is severe or persists, an evaluation is sensible.
4. Do men get oedema-type obesity too?
Yes. Middle-aged men with prolonged sitting, frequent eating out, high salt intake and many social meals also commonly notice facial and ankle puffiness and a soft mid-section. The cause may also lie in the heart, kidney, liver or medication, and investigations may be appropriate.
5. Can I just drink damp-dispelling tea on my own?
Not as a long-term self-prescription. For those with cold-leaning constitution, stomach pain, loose stools or qi-and-blood deficiency, over-aggressive damp clearing can make things worse. The constitution should be clarified first.
6. Will weight come back once I stop TCM treatment?
Whether weight rebounds is less about stopping the herbs or acupuncture, and more about whether dietary structure, activity, sleep and stress management are sustained afterwards. If the herbs were used to push the scale down without any change in lifestyle, weight tends to climb again. By contrast, in oedema-type weight management, where salt intake, protein, activity and cycle care have already been reset during treatment, the gains hold for a while after stopping. The role of TCM is to make sustainable change easier — not to manage every meal for you.
Related reading:
- Eating Little but Not Losing Weight? TCM on Weak Digestion →
- Bloated and Heavy? Phlegm-Damp Obesity and Water Retention in TCM →
- Weight Stable but Belly Fat Visible? Distinguishing Water Retention, Constipation, and Real Fat in TCM →
Disclaimer: This article is for general health education only and does not replace individual diagnosis, gynaecological evaluation, kidney-function testing or treatment. If you experience unilateral leg swelling, chest pain or shortness of breath, urine changes, blood in urine, pregnancy-related swelling, high blood pressure, blood in stool or black stools, please seek medical attention promptly. Note: the case above is a composite anonymous scenario for educational use, not a single real patient record.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Can I See a TCM Practitioner While on a GLP-1 Injection?
GLP-1 weight-loss injections are now a major talking point in Hong Kong. This article compares the roles of prescribed GLP-1 medication and TCM care across three phases — before treatment, during treatment and after stopping — covering medical monitoring, side-effect relief and post-discontinuation rebound, and identifying scenarios that should not be managed by TCM alone.

Does Black Coffee Help with Weight Loss? Timing and Side Effects
Black coffee may briefly raise metabolism and suppress appetite, but for those with acid reflux, palpitations, insomnia, chronic fatigue or premenstrual symptoms, it can do more harm than good. This article looks at the evidence and the TCM perspective, identifies five body types that should drink with care, and explains how to arrange timing and quantity sensibly.

168 Fasting vs Low-Carb vs Keto: A TCM Guide to the Differences
168 fasting, low-carb diets, and keto are all popular weight-loss approaches, but they restrict different things — and their effects on digestion, sleep, blood glucose, bowels, menstruation, and mood differ accordingly. This article compares the three, explains which TCM constitutions need extra caution, and flags situations that warrant prior assessment by a Western doctor or registered dietitian.