A Self-Check Guide to 4 Types of Menstrual Pain and Relief Tips
Menstrual pain is not something you simply have to endure. This guide explains the difference between primary and secondary dysmenorrhea, outlines four common TCM patterns, highlights five warning signs that need medical review, and offers practical relief strategies for everyday care.
Medical review: Dr. To Ching, Jenny,Registered Chinese Medicine Practitioner #009330
1-Minute Quick Answer
Menstrual pain first divides into primary (functional, often soon after menarche) and secondary (caused by endometriosis, fibroids, adenomyosis or pelvic inflammation). TCM recognises four patterns, each with its own pain quality. This guide (reviewed by Dr To, CMCHK 009330) lists red flags, including pain after age 25 and during intercourse, that need gynecological assessment first.
A Self-Check Guide to 4 Common Types of Menstrual Pain and Relief Strategies
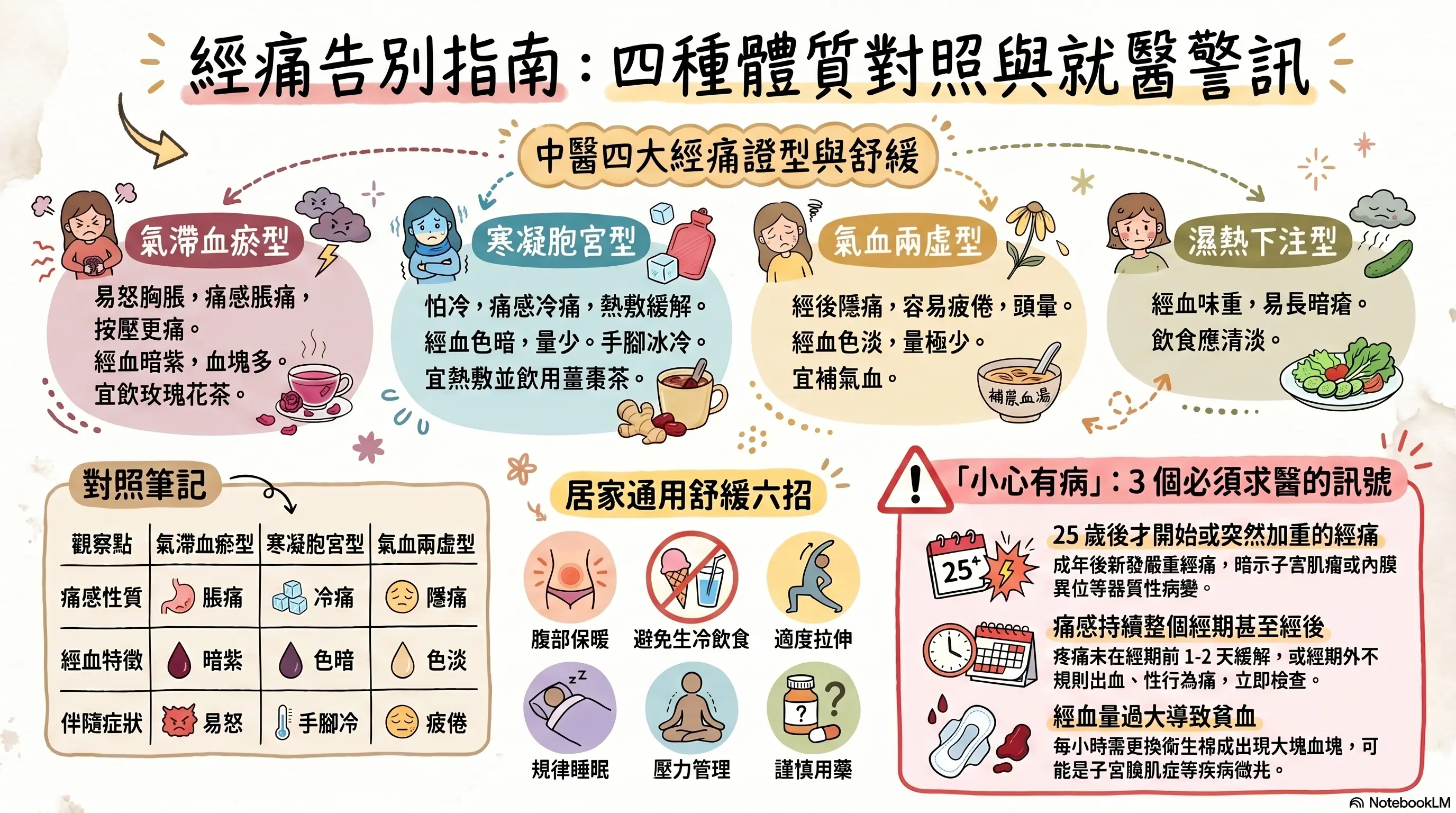 This image was generated with NotebookLM to help readers grasp the article quickly. Some Chinese text in the image may not display perfectly.
This image was generated with NotebookLM to help readers grasp the article quickly. Some Chinese text in the image may not display perfectly.
Medical review: Dr. To Ching, Jenny (CMCHK 009330 | Gynecology, Chinese medical aesthetics, postpartum abdominal binding, pediatrics)
For some women, the first one to three days of each cycle mean sweating, nausea, missing work, and lying in bed with a hot-water bag. Yet many still hear the same response: “Just bear with it.”
Menstrual pain is often dismissed as a matter of constitution, but persistent or worsening pain is not something to ignore. In some cases, the problem may be linked to conditions such as endometriosis, fibroids, adenomyosis, or pelvic inflammatory disease.
This article helps you sort out three important questions: how primary and secondary dysmenorrhea differ, which of four common TCM patterns your symptoms may resemble, and when you should arrange a gynecological assessment instead of relying on self-care alone.
First Distinguish Two Main Categories: Primary vs Secondary Dysmenorrhea
Before discussing constitution or pattern, it is important to decide whether the pain is more likely to be primary or secondary dysmenorrhea.
| Type | Main feature | Typical timing |
|---|---|---|
| Primary dysmenorrhea | Functional menstrual pain without obvious structural disease of the uterus or ovaries | Often begins within 1 to 2 years after menarche; pain is usually worst before the period and during the first 1 to 2 days |
| Secondary dysmenorrhea | Menstrual pain caused by an underlying condition such as endometriosis, fibroids, adenomyosis, or pelvic inflammation | More likely to begin after age 25, or to suddenly worsen; pain may last throughout the whole period or continue afterwards |
When people say “be careful, there may be an underlying problem”, they are mainly referring to secondary dysmenorrhea. TCM has a clear approach for functional, primary menstrual pain, but suspected secondary pain should first be assessed with appropriate medical investigation.
Four Common TCM Patterns of Menstrual Pain
1. Liver Qi Stagnation with Blood Stasis
This pattern often includes breast fullness before the period, irritability, dark-purple menstrual blood with clots, and lower abdominal pain that feels fixed in one place. Pressure tends to worsen the pain, while passing clots may bring some relief.
It is commonly associated with long-term stress, emotional suppression, sleep deprivation, and a rushed lifestyle. The usual TCM direction is to regulate liver qi and move blood.
2. Cold Congealing in the Uterus
Typical features include cold hands and feet, pain that clearly improves with heat, worsening pain after cold drinks, dark menstrual blood with clots, and periods that tend to come late.
This pattern is often linked to repeated exposure to cold, eating chilled food during menstruation, heavy air-conditioning, inadequate warmth, or getting wet and cold without proper recovery. The TCM approach focuses on warming and dispelling cold.
3. Qi and Blood Deficiency
This pattern often causes a dull, lingering pain that appears later in the period or after bleeding ends. Menstrual flow may be light and pale. Fatigue, dizziness, pale complexion, and prolonged weakness after menstruation are common.
It is more often seen in people who have been dieting for a long time, recovering after childbirth, living with chronic illness, or losing sleep and energy over a long period. Here, the key issue is not only pain relief but also replenishing what the body lacks.
4. Damp-Heat Pouring Downward
Common signs include increased yellow discharge, bright-red or dark-red blood with odor, a burning sensation with pain, constipation, thirst, acne, and a greasy yellow tongue coating.
This pattern is often linked to rich, greasy, spicy, or heavily seasoned food, frequent eating out, and an imbalanced routine. The usual approach involves clearing heat, resolving dampness, and improving diet and daily habits.
A Quick Self-Check Table
| What to observe | Liver qi stagnation with blood stasis | Cold congealing | Qi and blood deficiency | Damp-heat |
|---|---|---|---|---|
| Nature of pain | Distending or stabbing | Cold, cramping pain | Dull aching | Burning pain |
| Typical timing | 1–2 days before menstruation | Before and at the start of menstruation | Later in the period or after it ends | Throughout the whole period |
| Response to heat | Some relief | Clear relief | Partial relief | Heat may not help |
| Menstrual blood | Dark purple, more clots | Dark, with clots | Pale, scanty | Brighter or darker red, sometimes with odor |
| Common accompanying signs | Breast fullness, irritability | Feeling cold, back soreness | Tiredness, dizziness | Acne, more discharge, constipation |
Many people show a mixed pattern rather than a single textbook type. In practice, the main and secondary features need to be weighed together.
Five Red Flags That Need Medical Review
The following situations should not be dismissed as “just bad period pain”:
- Menstrual pain starts only after age 25, or suddenly becomes much worse
- Pain lasts throughout the whole period, or continues afterwards
- Very heavy bleeding, such as needing to change sanitary protection hourly, or passing large clots
- Bleeding between periods, including post-coital bleeding
- Pain during intercourse
These features may point to endometriosis, fibroids, adenomyosis, pelvic inflammatory disease, ovarian cysts, or other gynecological conditions. Depending on the case, medical evaluation may include pelvic ultrasound, hormone testing, or MRI. TCM cannot replace these investigations.
Everyday Relief Strategies
Whatever the pattern, the following steps help many people:
- Keep the lower abdomen warm with a warm pack or hot-water bag for 15 to 20 minutes
- Reduce cold food and drinks in the week before the period, especially iced drinks, raw salads, and excess coffee
- Keep a regular sleep schedule, because sleep deprivation often worsens both pain and mood changes
- Stay gently active with walking, light stretching, or yoga in the week before the period
- Use painkillers with awareness: short-term use can be reasonable, but needing larger or more frequent doses each month should prompt reassessment
How Does TCM Usually Treat Menstrual Pain?
| Treatment | When it is often used | Common arrangement |
|---|---|---|
| Chinese herbal medicine | All pattern types, tailored to presentation | Often taken from 7 to 10 days before the period until day 2 or 3 of menstruation |
| Acupuncture | Many pattern types, especially stagnation and stasis | Usually 1 to 2 sessions in the week before menstruation |
| Moxibustion | Often used for cold-type patterns | Applied to warm the lower abdomen and lower back |
| Acupoint support | Mild pain or daily maintenance | Arranged according to the doctor’s assessment |
In most cases, TCM regulation of the cycle is assessed over two to three menstrual cycles rather than after only one or two visits.
How Aspira TCM Clinic Approaches Menstrual Pain
Dr. To begins by reviewing the timing of pain, pain quality, menstrual flow, cycle length, lifestyle, stress, sleep, diet, and any existing gynecological reports. Tongue and pulse findings are then considered together with the symptom pattern.
If secondary dysmenorrhea is suspected, we would usually advise gynecological investigation first. Once structural disease has been ruled out or properly managed, Chinese herbal medicine, acupuncture, or moxibustion may be considered to support functional improvement.
If menstrual pain is already affecting your work, sleep, mood, or daily routine, it is helpful to track at least two cycles of symptoms, bleeding, and related changes before consultation.
FAQ
1. Does menstrual pain always mean “cold in the womb”?
No. Menstrual pain can arise from qi stagnation, blood stasis, cold, deficiency, or damp-heat. It should not be labelled “cold” purely because heat feels comforting.
2. When should I see a gynecologist before trying TCM?
If the pain starts after age 25, suddenly becomes worse, lasts the whole period, comes with very heavy bleeding, irregular bleeding, or painful intercourse, arrange gynecological assessment first.
3. Will painkillers become less effective over time?
Not necessarily, but if you need them more frequently or in larger doses each month, it may suggest that the underlying pattern is changing and needs reassessment.
4. Do clots always mean blood stasis?
Not always. Clots are common in blood stasis and cold patterns, but they must be judged together with pain type, bleeding volume, timing, and other symptoms.
5. Is heat therapy enough on its own?
Heat helps many people, especially in cold-type patterns, but it is not a full assessment. If you rely on heat every cycle just to get through the day, further evaluation is still worthwhile.
Related reading:
Disclaimer: This article is for general health education only and does not replace individual diagnosis, prescription, or treatment. If menstrual pain is worsening, affecting daily life, or accompanied by unusual bleeding, fever, fainting, or other concerning symptoms, seek medical attention promptly.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

TCM on Blood Thinners: Herbs and Acupuncture in Atrial Fibrillation
The most common question from elderly atrial fibrillation patients on blood thinners is whether they can also take Chinese herbal medicine or have acupuncture. The answer is yes, but with three prerequisites: both practitioners must know about each other; blood-activating and tonifying herbs must be assessed by a registered TCM doctor; and the safety principles for acupuncture, cupping and gua sha must be strictly observed. This article focuses on that single question.

Does Black Coffee Help with Weight Loss? Timing and Side Effects
Black coffee may briefly raise metabolism and suppress appetite, but for those with acid reflux, palpitations, insomnia, chronic fatigue or premenstrual symptoms, it can do more harm than good. This article looks at the evidence and the TCM perspective, identifies five body types that should drink with care, and explains how to arrange timing and quantity sensibly.

Worried About Weight-Loss Injection Side Effects? A TCM Guide to Obesity Patterns, Acupuncture for Weight Loss, and Who It Suits
Many people in Hong Kong are interested in GLP-1 weight-loss injections but worried about side effects, rebound, and prescription safety. This article explains the common risks of weight-loss injections, then explores obesity patterns in TCM, how acupuncture may support weight management, and who may be more suitable for a TCM weight-loss assessment first.