TCM on Blood Thinners: Herbs and Acupuncture in Atrial Fibrillation
The most common question from elderly atrial fibrillation patients on blood thinners is whether they can also take Chinese herbal medicine or have acupuncture. The answer is yes, but with three prerequisites: both practitioners must know about each other; blood-activating and tonifying herbs must be assessed by a registered TCM doctor; and the safety principles for acupuncture, cupping and gua sha must be strictly observed. This article focuses on that single question.
Medical review: Dr. Chan Wing Kiu, Joanne,Registered Chinese Medicine Practitioner #009463
1-Minute Quick Answer
Elderly atrial fibrillation patients on blood thinners can still take Chinese herbs or have acupuncture (reviewed by Dr Chan, CMCHK 009463), if three things hold: both doctors know each other's prescription, a registered TCM doctor vets the herbs, and needling and cupping safety rules are followed. TCM never advises stopping the blood thinner.
Can Elderly Patients on Blood Thinners Take Chinese Medicine or Have Acupuncture? Three Prerequisites for Safe TCM Coordination in Atrial Fibrillation
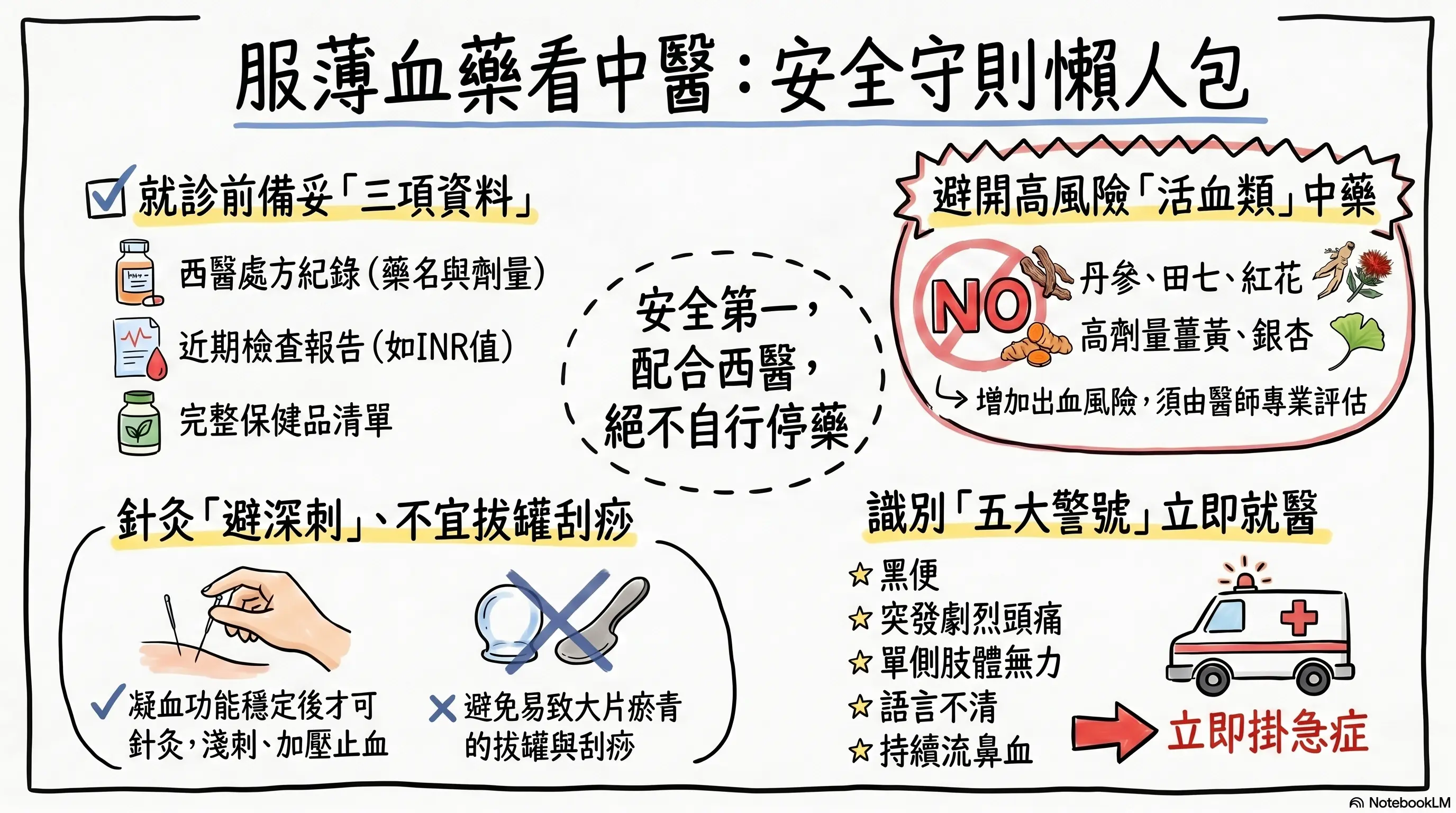 For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
Medical review: Dr Chan Wing-kiu (CMCHK 009463; geriatric gynaecology and internal medicine)
"My elderly relative has been diagnosed with atrial fibrillation. The doctor prescribed warfarin or Xarelto and they have been on it for over a year — can they also see a TCM practitioner?" "Will Chinese herbs make the bruising worse?" "Will ginger soup, ginseng or danshen interfere?" These are questions Aspira TCM Clinic receives every month.
What family members worry most about is the bleeding risk from herbs or acupuncture clashing with the blood thinner — and at the same time, leaving a tired, palpitating, sleep-deprived elderly relative without any TCM support. This article does not repeat the basics already covered by the prescribing doctor; it focuses on one core question: can someone on a blood thinner also see a TCM practitioner?
The short answer: yes, provided three things are in place — both practitioners are aware of each other's prescription; blood-activating and tonifying herbs are assessed by a registered TCM doctor; and the safety principles for acupuncture, cupping and gua sha are strictly observed. Any suspected bleeding, post-fall confusion or stroke-like symptom calls for Western medical attention or the emergency department immediately, not TCM.
What Must Be Done Before Adding TCM Care
To add TCM safely to long-term management, do not skip the following at or before the first visit: bring the Western prescription record (the type and dose of blood thinner, the start date, and recent INR or other test results); compile a full medication list (including rhythm drugs, antihypertensives, antidiabetics, lipid-lowering drugs, painkillers, supplements, and herbal soup ingredients); let the prescribing doctor know that TCM is now part of the care, either through the family member or by passing on a copy of the TCM prescription; tell the TCM practitioner about any history of falls, bruising or bleeding (including menstruation, gum bleeding, nosebleeds, recent surgery or dental extraction); and avoid self-purchased "heart-tonic" soups, "vessel-clearing pills" or "blood-activating ointments". Aspira TCM Clinic does not advise patients to stop, reduce or switch their blood thinner on their own — any change must be made by the prescribing doctor.
Which Chinese Medicines and Supplements Need Particular Care?
While on blood thinners, certain Chinese medicines and supplements can affect coagulation or drug metabolism. A registered TCM doctor will avoid or use the following with caution:
| Category | Common items / reason for caution |
|---|---|
| High-dose blood-activating herbs | Danshen, safflower, peach kernel, chuanxiong, leech, ground beetle, tianqi, sanqi — taken alongside a blood thinner, the risk of bruising and bleeding rises |
| Salicylate-containing or coagulation-affecting botanicals | Asarum, dahurica (containing salicylates); ginkgo leaf, turmeric (high-dose), garlic extract, Coenzyme Q10 — may potentiate the blood thinner or affect platelet aggregation |
| Tonifying herbs | Ginseng, American ginseng, ling zhi, dang gui, fo-ti — some literature suggests effects on coagulation or warfarin metabolism |
| Folate / vitamin K supplements | Some multivitamins and "wellness" pills — particularly relevant to warfarin, may shift the INR |
| Topical blood-activating products and online purchases | Hit-injury liniments and ointments (absorbed through the skin); products marketed as "vessel-clearing" or "meridian-clearing" with unknown contents are best avoided altogether |
A registered TCM doctor will choose milder herbs that are less likely to affect coagulation, in line with the patient's pattern, and will keep the prescribing doctor informed of the herbal direction.
Safety Principles for Acupuncture, Cupping, Gua Sha and Trauma Liniments
While on blood thinners, the chance of bruising in the subcutaneous and muscular layers rises noticeably, and external therapies must be adjusted accordingly. A useful timing distinction: at the start of blood-thinner therapy — when warfarin dosing is still being titrated, the INR is not yet stable, or a NOAC is still in its side-effect observation window — acupuncture is best deferred. Once the prescribing doctor confirms a stable coagulation index, coordinated acupuncture can be considered. For long-term users with consistently stable INR, a registered TCM doctor can usually proceed with acupuncture under strict safety principles.
For acupuncture itself: the practitioner will choose safer points, avoid deep needling, prolong post-needle pressure, avoid sites with dense vessels or lymph nodes, and not perform multiple bleeding or pricking points within the same session. Any large bruise or persistent bleeding after a session should be reported to both the TCM and prescribing doctors. Cupping and gua sha tend to leave large bruises and local bleeding while on blood thinners and are generally not recommended as routine; if used at all, the registered TCM doctor will adjust the force, area and frequency. Trauma liniments may contain blood-activating components — disclose them to the TCM and prescribing doctors before use, and do not apply them over large skin areas or broken skin. In short, the "deeper and stronger is better" logic of external therapies does not apply to blood-thinner patients — safety outranks intensity.
How TCM Can Support Atrial-Fibrillation-Related Symptoms
TCM is not in the business of "curing atrial fibrillation"; it supports the related symptoms and quality of life. Common patterns include heart-qi deficiency or heart-blood deficiency (palpitations, easy fatigue), qi-and-yin deficiency (palpitations, dry mouth, night sweats), heart-spleen deficiency (insomnia, forgetfulness, poor appetite) and phlegm-turbidity obstructing the channels (chest oppression, copious phlegm, thick greasy tongue coating). Because the blood thinner already occupies the "anti-thrombotic" role, the TCM prescription tends to focus on replenishing qi and blood and nourishing yin to calm the spirit, with blood-activating herbs reduced or omitted — to avoid stacking bleeding risk.
When Must a Western Doctor or Emergency Department Take Over?
The following are red flags. TCM alone is not enough:
- Sudden severe headache, sudden visual change, unilateral limb weakness or slurred speech (suspected stroke)
- Sudden chest pain, shortness of breath, fainting (suspected cardiac event or pulmonary embolism)
- Persistent severe bleeding: black stools, blood in stool, coughing or vomiting blood, large amounts of blood in urine
- Confusion, drowsiness or vomiting after a fall
- Sudden large bruising, uncontrollable bleeding, or nosebleeds lasting over 15 minutes
- Markedly abnormal heart rate (sustained over 120 or under 50 bpm) with dizziness or fainting
- Sudden swelling, breathing difficulty, inability to lie flat (suspected heart failure)
TCM cannot replace emergency care. For any suspected stroke, cardiac event or major bleed, the first step is the emergency department.
How Aspira TCM Clinic Assesses Blood-Thinner Patients
At the first visit, Dr Chan asks elderly atrial fibrillation patients on blood thinners to bring along: the full Western prescription list; INR, ECG, ultrasound and other recent reports from the past 3–6 months; the prescribing doctor's contact; any history of bleeding, falls, bruising or surgery; and any Chinese medicines, soups or supplements currently used. The whole programme runs on the principle of supporting the Western prescription; Aspira TCM Clinic does not promote it as "stopping the medication" or "curing atrial fibrillation".
FAQ
1. Can elderly patients on blood thinners really see a TCM practitioner?
Yes — provided three things are in place: bringing the prescription record and recent test results; having blood-activating and tonifying herbs assessed by a registered TCM doctor; and using safer acupuncture sites with no deep needling. Any change in medication must be made by the prescribing doctor; TCM will not advise stopping the blood thinner.
2. Do Chinese herbs clash with warfarin, Xarelto or Eliquis? Should ginger soup be avoided?
Some herbs — danshen, safflower, sanqi, ginseng, dang gui, ginkgo, ling zhi — can affect coagulation or drug metabolism, and a registered TCM doctor will assess before deciding the prescription direction. Small amounts of ginger as a seasoning usually have limited impact; large, concentrated ginger soups should be discussed with the prescribing doctor. The key principle is steady amounts — avoid sudden large increases. Self-prescribed herbs and "heart-tonic" soups from non-clinical sources are not advised.
3. Will acupuncture make bruising worse? Is cupping or gua sha still possible?
While on blood thinners, bruising and local bleeding after acupuncture are more likely; the registered TCM doctor selects safer points, avoids deep needling and applies appropriate post-needle pressure. Any large bruise or persistent bleeding should be reported. Cupping and gua sha are not recommended as routine; if needed, the TCM doctor will adjust force, area and frequency.
4. Can TCM "cure" atrial fibrillation?
No. The core management of atrial fibrillation remains rate or rhythm control and stroke prevention by the Western team. The TCM role is to support symptoms, constitution, sleep and quality of life — not to "cure" or "wean off the medication".
5. If a patient is on aspirin alongside a blood thinner, can TCM still help?
Aspirin is an antiplatelet agent, and combined with a blood thinner it further raises bleeding risk. TCM does not handle the medication itself; it assesses the constitution, sleep, bowel and other associated issues and strictly avoids blood-activating herbs. All decisions about drug combinations and adjustments rest with the prescribing doctor.
6. A relative has just had a stroke and is on heparin in hospital. Can TCM acupuncture be added now?
Acupuncture is not advised in the acute phase. A stroke in its acute stage is an emergency, and management must remain led by the hospital's neurology or cardiology team. Whether and when acupuncture is appropriate is a decision for the prescribing doctor once the patient and the coagulation index are stable. The TCM role belongs to the rehabilitation phase and chronic-disease management — not to the acute lead.
7. Why do some TCM doctors say acupuncture is fine while others say no?
Each patient's coagulation stability, bleeding history, fall history, comorbidities and concurrent medications affect the judgement. A registered TCM doctor needs to see that particular patient's prescription record, recent investigations and current state before making an individualised call — "my friend on a blood thinner can have acupuncture" does not mean you can, and vice versa.
Related reading:
- TCM Wisdom for Stroke Prevention: A Complete Guide to Warning Signs, Daily Care & 4 Key Acupoints for Seniors →
- Can TCM Cure Everything? 5 Situations Where You Should See a Western Doctor First →
- Acupuncture treatment →
Disclaimer: This article is for general health education only and does not replace individual diagnosis, prescription or emergency care. For persistent black stools, large bruising, severe headache, sudden limb weakness or slurred speech, attend the emergency department immediately. Any change in medication should first be discussed with the prescribing doctor.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

A Self-Check Guide to 4 Types of Menstrual Pain and Relief Tips
Menstrual pain is not something you simply have to endure. This guide explains the difference between primary and secondary dysmenorrhea, outlines four common TCM patterns, highlights five warning signs that need medical review, and offers practical relief strategies for everyday care.

Does Black Coffee Help with Weight Loss? Timing and Side Effects
Black coffee may briefly raise metabolism and suppress appetite, but for those with acid reflux, palpitations, insomnia, chronic fatigue or premenstrual symptoms, it can do more harm than good. This article looks at the evidence and the TCM perspective, identifies five body types that should drink with care, and explains how to arrange timing and quantity sensibly.

Worried About Weight-Loss Injection Side Effects? A TCM Guide to Obesity Patterns, Acupuncture for Weight Loss, and Who It Suits
Many people in Hong Kong are interested in GLP-1 weight-loss injections but worried about side effects, rebound, and prescription safety. This article explains the common risks of weight-loss injections, then explores obesity patterns in TCM, how acupuncture may support weight management, and who may be more suitable for a TCM weight-loss assessment first.