Back Pain in Older Adults: Osteoporosis, Degeneration, or Sciatica?
Back pain in older adults may arise from muscular strain, lumbar degeneration, sciatica, osteoporotic fracture, falls, or other medical conditions. This article compares common causes, red-flag signs, when investigation is needed, and how TCM may help once urgent problems are excluded.
Medical review: Dr. Wong Ka Fai,Registered Chinese Medicine Practitioner #009985
1-Minute Quick Answer
Back pain in older adults can stem from muscular strain, lumbar degeneration, sciatica, or osteoporotic fracture — not just kidney deficiency. Osteoporosis itself may be painless; the pain usually comes from fracture. Severe pain after a fall, leg numbness or weakness, bladder-bowel changes, or fever need medical review first. Reviewed by Dr Wong, CMCHK 009985.
Back Pain in Older Adults: Osteoporosis, Lumbar Degeneration, or Sciatica? Common Causes and When to Investigate
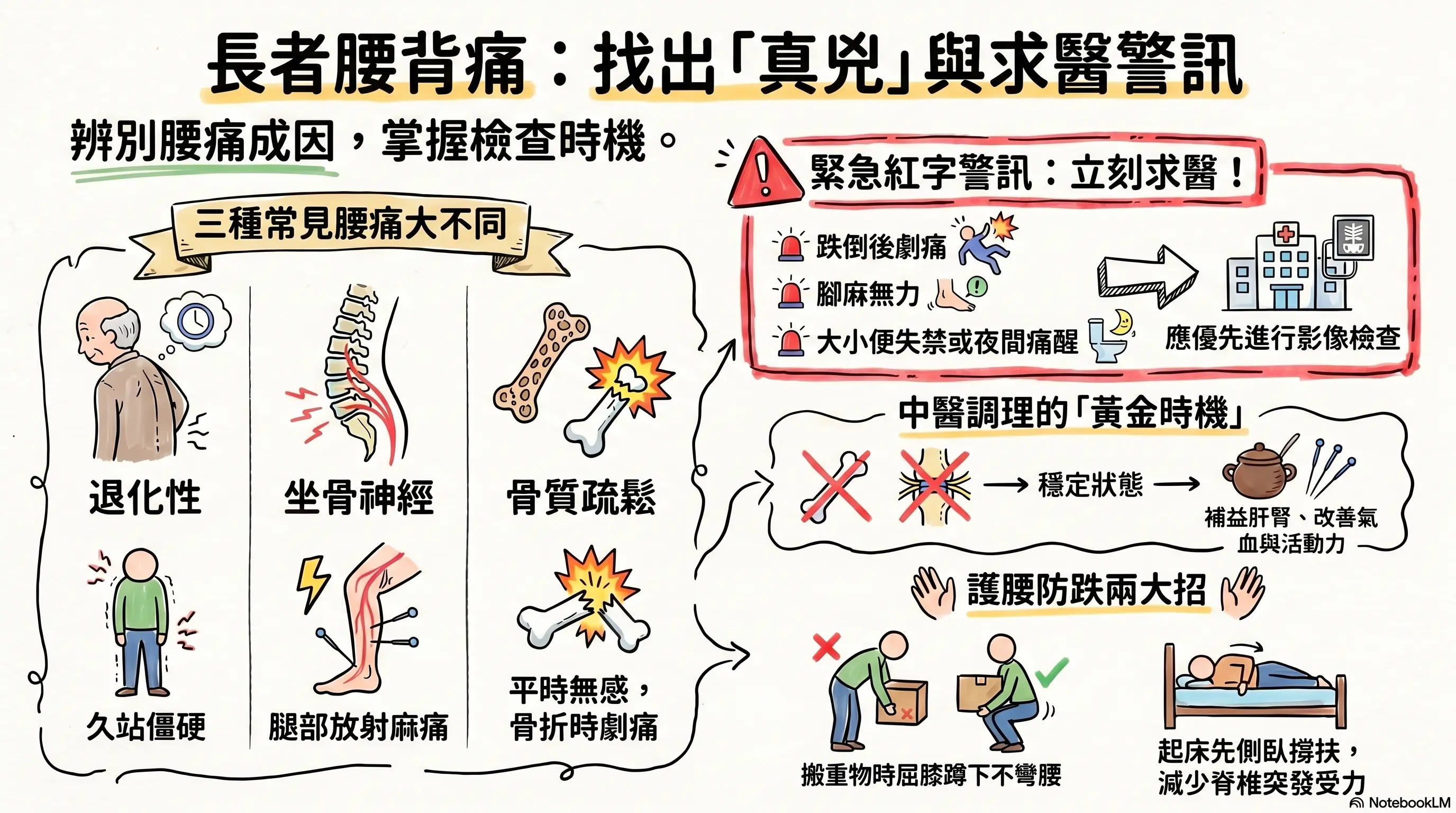 To help readers quickly grasp the content, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
Back pain is common in older adults, but the label “back pain” can hide very different problems. Some pain follows prolonged sitting, bending, or lifting and is mainly muscular. Some reflects lumbar degeneration or nerve compression. Some appears after a fall and is due to fracture. Some patients have osteoporosis in the background and only discover a vertebral compression fracture when sudden pain begins.
If every case is explained away as “kidney deficiency” or “osteoporosis”, misjudgment becomes easy. Sudden severe pain, inability to move after a fall, numb or weak legs, bladder or bowel changes, cancer history, long-term steroid use, or known osteoporosis all require more than massage, patches, or TCM care alone.
This article explains the common differences between osteoporotic pain, lumbar degeneration, and sciatica, when testing should come first, and how TCM may help once safety has been established.
Common Causes of Back Pain in Older Adults
| Cause | Common pain pattern | What deserves extra attention |
|---|---|---|
| Muscular strain | Aching after bending, lifting, long sitting, or long standing | Should gradually improve with rest; worsening needs assessment |
| Lumbar degeneration | Pain after prolonged standing, walking, or poor posture | May come with stiffness and reduced movement range |
| Sciatica | Pain radiating from the low back to buttock, thigh, calf, or foot | Numbness, weakness, or bladder-bowel changes need urgent review |
| Osteoporotic fracture | Sudden back pain, pain on turning in bed or getting up, loss of height | Osteoporosis itself may be painless; the pain often comes from fracture |
| Falls or impact injury | Sharp local pain after a fall, inability to bear weight | Fracture must be excluded, especially in the hip or spine |
| Other medical disease | Night pain, fever, weight loss | Infection, tumour, or internal disease must be excluded |
The key is not to diagnose by pain location alone, but to ask how it began, whether trauma occurred, whether nerve symptoms are present, and whether whole-body warning signs have appeared.
Does Osteoporosis Itself Cause Back Pain?
Osteoporosis may produce no obvious symptoms by itself. What usually causes pain is fracture, especially vertebral compression fracture. If an older adult develops sudden back pain after a minor fall, turning movement, or even without clear trauma, and the pain is severe enough to make turning, coughing, or getting out of bed difficult, Western assessment should come first.
Situations that deserve greater attention to osteoporosis-related risk include:
- Confirmed osteoporosis or low bone mass
- Previous low-trauma fracture
- Loss of height or worsening stooped posture
- Postmenopausal women, small build, or long-term lack of weight-bearing activity
- Long-term use of high-dose steroids
- Back, hip, or wrist pain after a fall
TCM may support soreness, pain, qi-blood recovery, and function, but it does not replace bone-density testing, imaging, fracture diagnosis, or necessary medication.
How Can Lumbar Degeneration and Sciatica Be Distinguished?
Lumbar degeneration is commonly linked to ageing, postural strain, and reduced muscle strength. It may cause stiffness, aching, and limited movement in the low back. Sciatica more often produces radiating pain that travels from the low back or buttock down the thigh, calf, and sometimes into the foot, with numbness, pins-and-needles, or weakness.
| Feature | More like local lumbar or muscular pain | More concerning for nerve compression |
|---|---|---|
| Pain location | Mainly localised in the low back | Travels from the back or buttock into the leg or foot |
| Sensation | Ache, tightness, stiffness | Numbness, electric-shock pain, pins-and-needles |
| Activity effect | Worse after sitting, standing, or bending | Coughing, bending, or walking may trigger radiating pain |
| Risk | Restricts movement and posture | Leg weakness or bladder-bowel changes need urgent attention |
If an older adult has numb or weak legs, foot dragging, loss of bladder or bowel control, or numbness around the saddle area, this is not ordinary back pain and requires urgent medical review.
When Should Investigations Come First?
Western or emergency assessment should come first, with X-ray, MRI, bone-density, or other tests as indicated, if any of the following is present:
- Severe back pain after a fall, impact, or even a seemingly minor knock
- Sudden intense back pain made worse by turning, coughing, or getting up
- Back pain with leg numbness, leg weakness, or clearly unstable walking
- Loss of bladder or bowel control, or numbness around the groin and anus
- Fever, night pain, or unexplained weight loss
- History of cancer, long-term steroid use, or known osteoporosis
- Pain that lasts for weeks without improvement, or steadily worsens
- Use of anticoagulants with pain or bruising after a fall
For older adults, early clarification of fracture or nerve compression can prevent a cycle of pain-related inactivity, loss of strength, and higher fall risk.
How Does TCM Understand Back Pain in Older Adults?
TCM assessment of back pain begins with respect for modern diagnosis and test results, then considers pain quality, functional ability, tongue and pulse, sleep, appetite, bowel and bladder function, nocturia, chronic illness, and medication use.
| TCM pattern | Common features | Treatment focus |
|---|---|---|
| Liver-kidney deficiency | Sore back and knees, weaker legs, nocturia, tinnitus | Support liver-kidney function and strengthen the sinews and bones |
| Cold-damp obstruction | Aching heaviness after cold or damp weather, or air-conditioning | Warm the channels, dispel cold and damp, free the collaterals |
| Blood stasis in the collaterals | Fixed stabbing pain, old injury, local pain after a fall | Invigorate blood carefully, especially if anticoagulants are used |
| Qi-blood deficiency | Fatigue, pale complexion, poor stamina, slow recovery | Tonify qi and nourish blood, support repair capacity |
| Spleen-kidney yang deficiency | Cold sensitivity, low energy, loose stools, back soreness | Warm and support spleen-kidney function after internal risks are excluded |
TCM may help with pain, muscle tension, soreness, sleep, and functional recovery once fracture, nerve compression, infection, or tumour have been properly excluded.
Practical Back-Care and Fall-Prevention Tips
-
Avoid sudden bending and twisting.
When lifting, keep the load close, bend the knees, and avoid using the waist alone. -
Slow the getting-up movement.
Roll to the side first, place both feet over the edge of the bed, then use the arms to push up. This reduces sudden load through the spine. -
Choose a suitable chair.
Seats that are too low, too soft, or too deep make standing harder and may worsen back strain. -
Stay active within your ability.
Long periods of bed rest or complete inactivity weaken the muscles further. In stable stages, stretching and strength work can be introduced under advice. -
Review bone health and fall risk.
Anyone with previous falls, loss of height, worsening stoop, or known osteoporosis should manage fracture risk proactively with their doctor.
How Aspira TCM Evaluates Back Pain in Older Adults
At Aspira TCM, Dr Wong will first ask about pain location, any fall or impact, whether pain radiates into the leg, whether leg numbness or weakness is present, walking ability, history of osteoporosis or fracture, medication use, and any previous imaging reports.
If the case is stable and suitable for integrative care, treatment may focus on liver-kidney deficiency, cold-damp obstruction, blood stasis, qi-blood deficiency, or muscle imbalance, using acupuncture, herbs, manual care, topical treatment, and lifestyle guidance. If fracture, nerve compression, or another serious cause is suspected, Western or specialist assessment will be recommended first.
If you or an older family member has recurrent back pain, concerns about osteoporosis, lumbar degeneration, or sciatica, it helps to bring bone-density results, X-rays, MRI reports, medication lists, and any fall history to the consultation.
FAQ — Common Questions About Back Pain in Older Adults
Q1: Does back pain in older adults always mean osteoporosis?
No. Back pain may come from muscle strain, posture, lumbar degeneration, sciatica, falls, or other disease. Osteoporosis itself may be silent; the pain often comes from fracture.
Q2: Can sciatica be treated with TCM?
In stable cases, yes, after assessment. Acupuncture, herbs, and lifestyle guidance may help. But leg weakness, bladder-bowel changes, saddle numbness, or rapidly worsening pain require Western care first.
Q3: Does every older person with back pain need an X-ray?
Not necessarily. Mild and short-lived pain without trauma or neurological warning signs may not need immediate imaging. But severe pain after a fall, known osteoporosis, leg numbness or weakness, or steadily worsening symptoms should be assessed by a doctor.
Q4: Is massage safe for back pain?
It depends on the cause. If fracture, acute injury, severe nerve compression, or osteoporotic fracture is suspected, strong self-massage is not appropriate. The cause should be clarified first.
Q5: What should I prepare before seeing a TCM doctor?
Bring bone-density, X-ray, or MRI reports, a medication list, fall history, the pain location, and whether there is leg numbness or weakness.
Related reading:
- Low Back Pain Is Not Just “Kidney Deficiency”: 6 Common Causes and TCM Treatment Approaches →
- Sciatica Recovery — Combined Acupuncture and Bone-Setting Treatment →
- Complete TCM Guide to Pain Treatment →
Disclaimer: This article is for health education only and cannot replace personal consultation, imaging, bone-density testing, medication, or treatment advice. Seek urgent medical attention for severe pain after a fall, inability to stand, sudden severe back pain, leg numbness or weakness, bladder-bowel changes, fever, weight loss, head injury, or confusion. Any medication adjustment should first be discussed with the treating doctor.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Recurrent Knee Pain in Older Adults: Is It Just Degeneration?
Recurrent knee pain in older adults is not always simple degeneration. Osteoarthritis, muscle weakness, cold-damp patterns, qi-blood deficiency, old injuries, and fall risk may all contribute. This article explains common causes, red-flag signs, TCM patterns, and practical ways to reduce recurrence.

Dizziness in Older Adults: ENT, Cardiology, or TCM?
Dizziness in older adults can mean vertigo, near-blackout on standing, unsteady walking, or a heavy foggy head. Causes range from BPPV and blood-pressure fluctuation to arrhythmia, anaemia, low blood sugar, medication effects, stroke warning signs, and qi-blood deficiency. This article explains which situations suit ENT, cardiology, general medicine, emergency care, or TCM.

Bigger Belly, Same Weight? TCM on Bloating, Constipation, and Fat
Stable weight but a more prominent belly does not always mean fat. Water retention, constipation, gastrointestinal bloating, posture, reduced muscle mass, and central obesity can all make the abdomen appear larger. This article uses TCM perspectives on digestion, phlegm-damp, qi stagnation, and constipation to help you distinguish situations and decide next steps.