Bigger Belly, Same Weight? TCM on Bloating, Constipation, and Fat
Stable weight but a more prominent belly does not always mean fat. Water retention, constipation, gastrointestinal bloating, posture, reduced muscle mass, and central obesity can all make the abdomen appear larger. This article uses TCM perspectives on digestion, phlegm-damp, qi stagnation, and constipation to help you distinguish situations and decide next steps.
Medical review: Dr. Au Kwok Po, Arthur,Registered Chinese Medicine Practitioner #009884
1-Minute Quick Answer
A more prominent belly with stable weight isn't always fat — water retention, constipation, gas, posture, and weak core muscles can all enlarge the abdomen. This guide (reviewed by Dr Au, CMCHK 009884) helps you tell water retention, constipation, and fat apart, and flags urgent signs like one-sided calf swelling or blood in stool.
Weight Stable but Belly Fat Visible? Distinguishing Water Retention, Constipation, and Real Fat in TCM
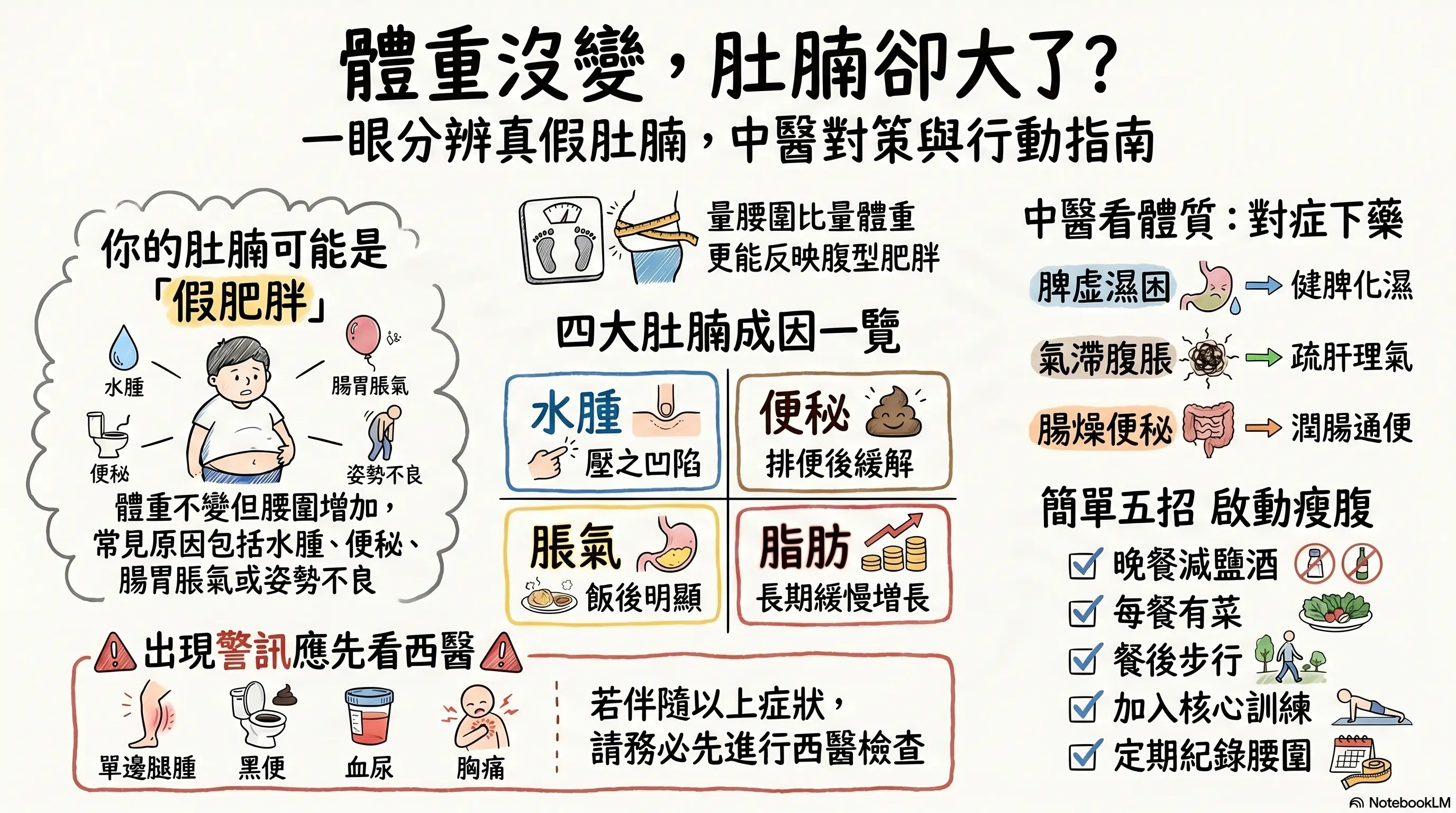 To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, this image was generated by NotebookLM. Some Chinese characters may not render correctly.
"My weight is roughly the same — why is my belly more prominent?"
When the waist expands, many people assume it must be fat. In fact, abdominal expansion can stem from several causes: water retention, constipation, gastrointestinal bloating, premenstrual fluid retention, posture and weakened core musculature, or genuine accumulation of abdominal fat.
This article helps you distinguish: when weight is stable but the belly is visibly larger, how to observe water retention, constipation, and fat accumulation; how TCM understands the situation through digestion, phlegm-damp, qi stagnation, and bowel function; and which abdominal or oedema findings warrant Western evaluation first.
Look at Waist Circumference, Not Just Weight
Total body weight is influenced by hydration, bowel state, salt intake, post-exercise muscle repair, and the menstrual cycle. Waist circumference reflects abdominal change more directly — particularly central-obesity risk.
Hong Kong's Department of Health notes that for ethnic Chinese adults, BMI 23.0 to under 25.0 is overweight, and 25.0 or above is obesity. Change4Health adds that for most Asian adults including Chinese, a waist of 90 cm or more in men, or 80 cm or more in women, indicates central obesity.
If your belly seems larger, also track:
- Weekly weight at a consistent time
- Weekly waist measurement at a consistent location
- Whether bloating relates to meals, constipation, or the menstrual cycle
- Whether calves, ankles, or face are puffy
- Bowel frequency, stool form, and whether evacuation feels complete
Distinguishing Water Retention, Constipation, and Fat
| Situation | Common Features | Key Observations |
|---|---|---|
| Water retention | Morning facial puffiness, afternoon ankle swelling, improves with low salt or rest | Short-term weight fluctuations; calf may pit when pressed |
| Constipation | Stools every few days, abdominal fullness, lower-abdominal distension, incomplete evacuation | Bloating eases after a bowel movement |
| Gastrointestinal bloating | Post-meal bloating, frequent burping, increased gas, worse under stress | Linked to eating speed, dairy, legumes, or stress |
| Fat accumulation | Waist gradually increases over weeks to months | Linked to total intake, sedentary time, sleep, alcohol, and activity |
| Muscle and posture | Modest weight but soft lower abdomen, anterior tilt | Often paired with weak core, sedentary lifestyle, low exercise |
A single person can have several at once. People who eat out frequently, sit for long periods, and live with high stress may simultaneously have phlegm-damp, water retention, constipation, and abdominal fat.
How TCM Reads "A More Prominent Belly"
TCM does not just look at belly size — it asks how it appears: is the bloating post-meal, morning puffiness, premenstrual swelling, post-constipation distension, or gradual waist expansion?
| TCM Direction | Common Features | Treatment Priority |
|---|---|---|
| Spleen deficiency with damp accumulation | Heaviness, post-meal fatigue, soft stools, thick tongue coating | Strengthen spleen, resolve damp; reduce sweet and cold drinks |
| Phlegm-damp accumulation | Thick belly, phlegm, chest tightness, sticky mouth | Resolve phlegm-damp alongside activity and dietary adjustment |
| Qi stagnation with bloating | High stress, fluctuating bloating, frequent burping, premenstrual distension | Soothe liver, regulate qi; adjust stress and meal rhythm |
| Intestinal dryness with constipation | Hard, dry stools, dry mouth, lower-abdominal fullness, dry skin | Moisten the bowels; increase water and fibre |
| Spleen-kidney yang deficiency | Cold sensitivity, oedema, low-back soreness, soft stools, fatigue | Warm yang and strengthen spleen; avoid overly cold "damp-resolving" approaches |
The TCM priority is to identify the dominant cause first. Constipation requires bowel-focused work; oedema requires distinguishing damp accumulation, yang deficiency, or Western-defined cardiac/renal/hepatic issues; persistent waist expansion requires combined fat-loss and metabolic-risk management.
Does Constipation Make the Belly Look Larger?
Yes. Stool retention, intestinal gas, and incomplete evacuation can all push out the lower abdomen. Common features:
- Bowel movement once every few days
- Hard, dry, or pellet-like stools
- Sense of incomplete evacuation
- Dry mouth, acne, poor sleep
- Insufficient hydration, low vegetable intake, prolonged sitting
Long-term reliance on laxatives or "detox products" is not advised. If constipation worsens suddenly, accompanied by blood in stool, black stools, rapid weight loss, increasing abdominal pain, or anaemia, see a Western doctor first.
What to Watch For with Water-Retention-Type Belly
Fluid retention causes a sense of fullness, heaviness, and swelling, with short-term weight fluctuations. TCM evaluates through spleen deficiency with damp accumulation, phlegm-damp, yang deficiency, or qi stagnation with fluid retention.
However, not all oedema can be classified as "dampness". The following warrant Western evaluation first:
- Rapid weight gain with marked leg or facial swelling
- Sudden one-sided calf swelling with pain, redness, or heat
- Oedema with breathlessness, chest pain, palpitations, or inability to lie flat
- Markedly reduced urine output, foamy urine, or blood in urine
- Existing heart, kidney, liver, or thyroid disease
- Sudden oedema with headache or hypertension during pregnancy
TCM can support constitutional and fluid-metabolism improvement (the body's capacity to circulate and clear excess fluids), but acute, unilateral, or red-flag oedema must not be delayed.
If It Really Is Fat — How to Approach It
If your waist has expanded over months, the abdomen has gone from soft to thick, and you frequently eat out, drink alcohol, exercise little, and sleep poorly, treat it as central obesity.
Six practical starting points:
- Track waist circumference weekly, not daily weight — waist change is more meaningful than scale fluctuations
- Reduce high-fat, high-salt meals and alcohol at dinner — alcohol, late-night eating, and heavy restaurant fare drive abdominal fat and fluid retention
- Protein and vegetables at every meal — improve satiety and reduce post-meal sweets and snacks
- Moderate staple-food portions — rice and noodles need not be eliminated, but avoid combining them with sugary drinks in excess
- Walk after meals — 10–20 minutes is far better than sitting still
- Add strength training — improving core, lower-body, and back strength benefits abdominal contour and daily energy expenditure
How Aspira TCM Evaluates a More Prominent Belly
We review weight, waist, diet, alcohol, sleep, bowel function, oedema location, menstrual cycle, exercise, and tongue and pulse. Dr Au identifies whether the dominant cause is water retention, constipation, gastrointestinal bloating, phlegm-damp obesity, or central fat accumulation.
Where TCM is appropriate, herbal medicine, acupuncture, ear-point therapy, nutritional guidance, and lifestyle adjustments are combined. Where abdominal pain, oedema red flags, abnormal weight changes, or suspected internal-medicine disease appear, Western investigation is recommended first.
If you are unsure whether your belly is water, constipation, or fat, track 7 days of waist, weight, bowel movements, diet, and oedema before booking a TCM weight-management consultation.
FAQ — Belly Bloating, Water Retention, and Abdominal Fat
Q1: If my weight is stable but my waist is increasing, is it always fat?
Not always. Water retention, constipation, bloating, premenstrual fluid retention, posture, and reduced muscle mass all affect appearance. If the waist increases consistently over months, address central fat and metabolic risk seriously.
Q2: Can damp-resolving teas reduce belly size?
If the main cause is water retention or dampness, some experience short-term improvement. But if the main cause is fat, constipation, or stress-driven eating, damp-resolving teas alone may not help. Patients with cold constitutions, stomach pain, or soft stools should not self-administer them long-term.
Q3: Should I take laxatives for constipation-type belly?
Long-term self-administration is not advised. Address hydration, fibre, healthy fats, activity, and bowel habits first. Sudden worsening, blood in stool, black stools, or weight loss require Western evaluation first.
Q4: At what waist measurement should I be concerned?
For most Asian adults including Chinese, a waist of 90 cm or more in men, or 80 cm or more in women, indicates central obesity. Even below those thresholds, ongoing waist expansion deserves attention.
Q5: Does TCM belly-reduction only mean acupuncture?
Not necessarily. TCM differentiates phlegm-damp, water retention, constipation, qi stagnation, spleen deficiency, or appetite issues first, then determines whether herbal medicine, acupuncture, ear-point therapy, dietary, or lifestyle adjustments are appropriate.
— Dr Au Kwok Po, Arthur | Registered Chinese Medicine Practitioner (Certified Nutritionist) Reg. No.: 009884 Aspira TCM Clinic | TCM Weight Management, Nutrition, Influenza, Hair Loss
Cannot Tell If Your Belly Is Water, Constipation, or Fat? Book a Consultation
How to book:
- WhatsApp: Book here
- Phone: 2110 9337
- Address: Unit 2706, 27/F, Saxon Tower, 7 Cheung Shun Street, Lai Chi Kok
Further reading:
- 168 Fasting, Low-Carb, Keto — How TCM Decides Who Should Be Cautious →
- Water Retention, Bloating, and Heaviness — Is It Dampness? TCM on Phlegm-Damp Obesity →
- Eating Less but Still Not Losing Weight? TCM on Weak Digestion and Slow Metabolism →
- A Complete Guide to TCM Acupoint Embedding for Weight Loss →
References
- Centre for Health Protection: Obesity — https://www.chp.gov.hk/tc/healthtopics/content/25/8802.html
- Change4Health: Waist Size, Body Shape and Health — https://www.change4health.gov.hk/en/whats_new/ncd_watch/20250211.html
- CDC: Steps for Losing Weight — https://www.cdc.gov/healthy-weight-growth/losing-weight/index.html
- NIDDK: Choosing a Safe & Successful Weight-loss Program — https://www.niddk.nih.gov/health-information/weight-management/choosing-a-safe-successful-weight-loss-program
Disclaimer: This article is for health education only. It does not replace individual consultation, examination, nutritional assessment, or treatment advice. Seek medical attention promptly for sudden severe abdominal distension, abdominal pain, vomiting, blood in stool, black stools, rapid weight gain, breathlessness, or one-sided calf swelling and pain.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Bloating, Fatigue, Insomnia After 168 Fasting? A TCM View
168 fasting does not suit everyone. Bloating, fatigue, cold intolerance, insomnia, dizziness, constipation, or appetite rebound after starting may signal that the eating window, nutrient distribution, digestion, or qi-blood state is not aligned. This article explains how TCM distinguishes digestive burden, qi-blood deficiency, phlegm-damp with qi stagnation, and yin deficiency with internal heat — and flags situations where pushing through is unwise.

Can I See a TCM Practitioner While on a GLP-1 Injection?
GLP-1 weight-loss injections are now a major talking point in Hong Kong. This article compares the roles of prescribed GLP-1 medication and TCM care across three phases — before treatment, during treatment and after stopping — covering medical monitoring, side-effect relief and post-discontinuation rebound, and identifying scenarios that should not be managed by TCM alone.

Eating Light but Not Losing Weight? A TCM Edema-Type Case Study
Eating light yet the scale will not budge — only the puffiness in the face, ankles and waistline persists? This case study follows Ya-lin (pseudonym), a 38-year-old office worker, through six months and explains how "eating clean but still not losing weight" often comes from a stack of small issues: salt, low protein, constipation, premenstrual fluid retention, phlegm-damp constitution, or internal disease. It also lists scenarios that warrant seeing a Western doctor first.