Dizziness in Older Adults: ENT, Cardiology, or TCM?
Dizziness in older adults can mean vertigo, near-blackout on standing, unsteady walking, or a heavy foggy head. Causes range from BPPV and blood-pressure fluctuation to arrhythmia, anaemia, low blood sugar, medication effects, stroke warning signs, and qi-blood deficiency. This article explains which situations suit ENT, cardiology, general medicine, emergency care, or TCM.
Medical review: Dr. Chan Wing Kiu, Joanne,Registered Chinese Medicine Practitioner #009463
1-Minute Quick Answer
Dizziness in older adults isn't always weakness: spinning vertigo often suggests BPPV or a vestibular problem, while slurred speech, one-sided weakness, chest pain, or a head injury after fainting needs emergency care first. This guide (reviewed by Dr Chan, CMCHK 009463) covers dizziness types, ENT/cardiology/internal-medicine triage, and fall risk.
Dizziness in Older Adults: ENT, Cardiology, or TCM? A Clear Guide to Triage, Blood Pressure, Vertigo, and Fall Risk
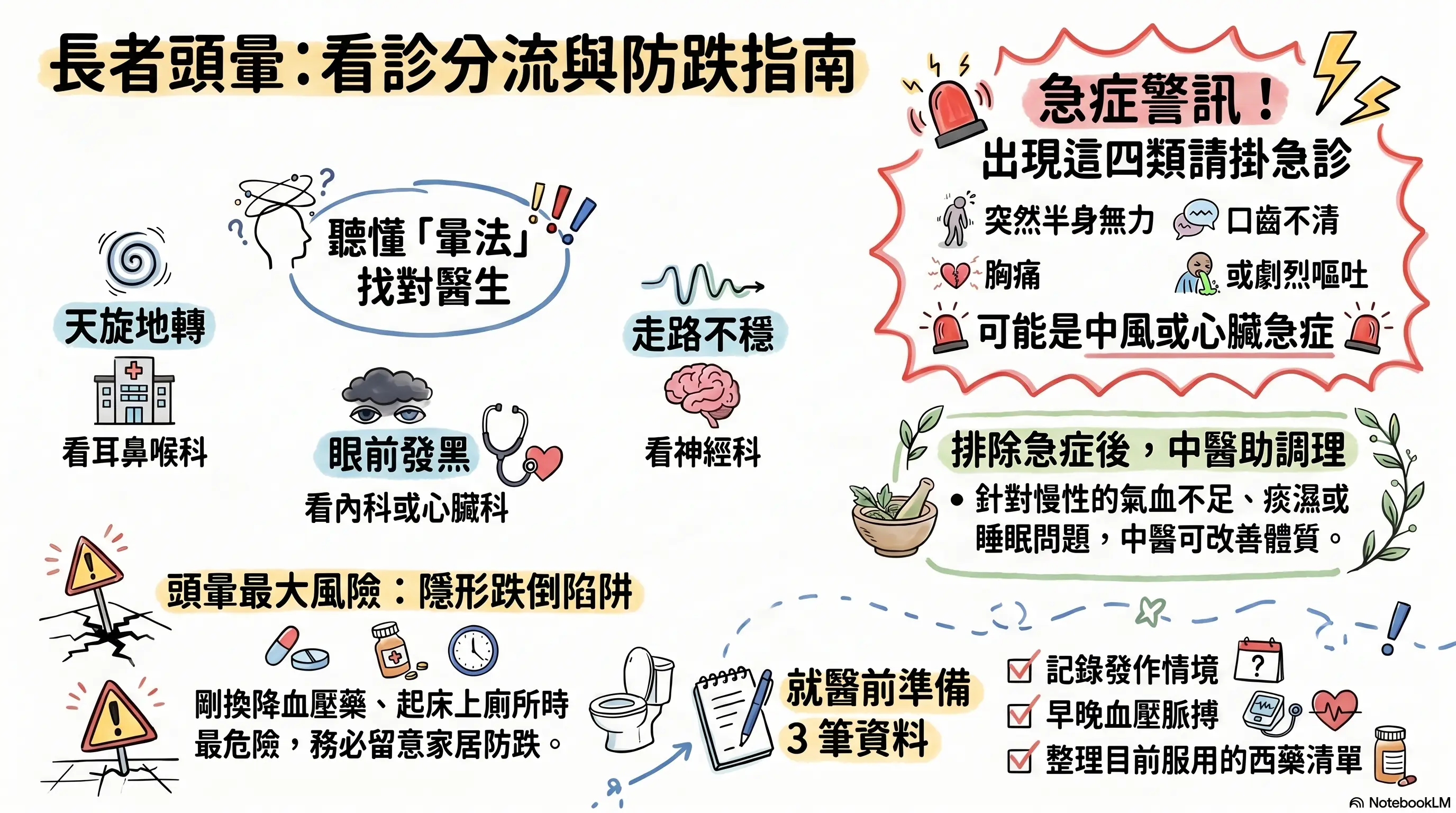 To help readers quickly grasp the content, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
To help readers quickly grasp the content, the cover image was generated with NotebookLM. Some Chinese characters may not render correctly.
When an older adult says “I feel dizzy,” the most difficult question for family is often not whether the symptom is real, but where to seek help first. Some people feel the room spinning when they turn in bed. Some feel their vision going dark on standing. Some walk as if floating or unsteady. Others mainly feel heavy-headed, foggy, or tight around the neck.
These different “types” of dizziness can point in very different directions. Benign positional vertigo, inner-ear disorders, blood-pressure fluctuation, arrhythmia, anaemia, low blood sugar, medication effects, stroke warning signs, and chronic qi-blood deficiency may all be involved. The real danger is mistaking stroke, cardiac disease, or a serious fall risk for “just weakness.”
This article explains the common types of dizziness in older adults, what ENT, cardiology, general medicine, emergency care, and TCM each do, and in which stable situations TCM may be used as a complement.
First Clarify: What Kind of Dizziness Is It?
| Sensation | Common description | Possible direction |
|---|---|---|
| Spinning vertigo | The room is turning; triggered by turning in bed or moving the head | BPPV, inner-ear, or vestibular problem |
| Blacking out on standing | Feels close to fainting when getting up | Postural hypotension, dehydration, medication, anaemia |
| Unsteady gait | Feels floaty, shaky, or afraid of falling | Balance problem, neurological issue, medication, muscle weakness |
| Heavy or foggy head | Head feels heavy, dull, tight, low in energy | Sleep, blood pressure, phlegm-damp, qi-blood deficiency |
| Sudden dizziness with neurological signs | Slurred speech, facial droop, one-sided weakness | Stroke must be excluded urgently |
In older adults, the issue is not only whether dizziness exists, but whether it is sudden, whether it increases fall risk, and whether it comes with chest pain, palpitations, neurological signs, or altered awareness.
When Should Emergency Care Come First?
Do not wait for TCM or routine outpatient review first if any of the following occurs:
- Sudden weakness, numbness, facial droop, or slurred speech
- Sudden change in vision, marked unsteady walking, or a fall
- Severe headache, repeated vomiting, or confusion
- Chest pain, chest pressure, breathlessness, or cold sweating
- Collapse, blackout, or head injury
- Very fast, very slow, or irregular heartbeat with dizziness
- Extremely high or low blood pressure with significant symptoms
Stroke and cardiac emergencies are time-sensitive. When dizziness appears with sudden neurological or cardiopulmonary warning signs, “rest first,” “drink some water,” or “see Chinese medicine later” is not safe enough.
How Are ENT, Cardiology, General Medicine, and TCM Different?
| Situation | Better first choice | Why |
|---|---|---|
| Sudden spinning when turning, bending, or looking up | ENT or family doctor | BPPV, vestibular, or ear-related causes may need assessment |
| Vision going dark on standing | Family doctor, general medicine, or cardiology | Lying-sitting-standing blood pressure, dehydration, and medication may need checking |
| Dizziness with palpitations, chest tightness, or fainting | Cardiology or emergency care | Cardiac rhythm or circulation problems must be excluded |
| Dizziness with slurred speech, one-sided weakness, or sudden imbalance | Emergency care | Stroke or acute neurological illness must be ruled out |
| Chronic heavy-headedness with poor sleep, fatigue, and phlegm | TCM may be considered | TCM may help once emergencies are excluded |
| Recurrent dizziness in a patient with hypertension | Western monitoring plus TCM support | Blood pressure and medication remain under Western supervision; TCM may help with constitution and symptom pattern |
TCM does not replace medical triage. Its role becomes clearer after urgent and obvious structural causes have been excluded.
Why Must Dizziness and Fall Risk Be Considered Together?
The most practical danger of dizziness in older adults is falling. Hong Kong Elderly Health Service notes that falls usually result from several interacting factors, including poor vision, reduced balance, gait problems, dizziness or faintness, medication effects, and hazards in the home.
Pay extra attention when:
- The person needs to hold walls or furniture after dizziness
- The worst episodes happen when getting up to use the toilet
- A new antihypertensive, sleeping pill, or painkiller has recently been added
- There have already been near-falls or actual falls
- Knee pain, numb feet, poor vision, or nocturia are also present
Families should treat dizziness as a fall-prevention issue, not only as a “supplement problem.”
How Does TCM Understand Dizziness?
TCM first asks whether urgent Western assessment is needed, then looks at the pattern of dizziness, sleep, mood, appetite, phlegm-damp tendency, blood pressure, blood sugar, bowel and bladder habits, tongue and pulse, and medication background.
| TCM pattern | Common features | Treatment focus |
|---|---|---|
| Qi-blood deficiency | Dizziness, pale complexion, fatigue, palpitations, worse on standing | Tonify qi and nourish blood, improve overall reserve |
| Phlegm-damp obstruction | Heavy head, chest oppression, much phlegm, body heaviness, bloating | Strengthen digestion, transform phlegm, clear dampness |
| Liver yang rising | Head pressure, irritability, bitter taste, light sleep | Calm liver yang, while blood pressure continues to be monitored |
| Liver-kidney deficiency | Dizziness with tinnitus, sore back and knees, nocturia, low vitality | Support liver-kidney function and improve frailty pattern |
| Blood stasis obstructing the clear orifices | Fixed headache, dark tongue colour, limb numbness | Invigorate circulation cautiously after stroke risk and anticoagulant issues are considered |
If the patient is taking antihypertensives, glucose-lowering drugs, anticoagulants, sleeping pills, or multiple long-term medicines, TCM herbs and acupuncture must be planned with extra care. Any change to Western medication should remain under the treating doctor.
What Should Families Prepare Before the Consultation?
-
Record the context of attacks.
For example: on getting up, turning in bed, after meals, after bathing, outdoors, or after medication. -
Record blood pressure and pulse.
Morning and evening readings help; if advised, note the values before and after getting up or during a dizzy spell. -
Prepare a medication list.
Include prescription drugs, over-the-counter remedies, Chinese patent medicines, supplements, painkillers, sleeping pills, and medicated wine. -
Note falls or near-falls.
Include the time, place, whether the head was hit, and whether the person could stand up again. -
Review home fall prevention.
The bedside, toilet, corridor, and night lighting are particularly important.
How Aspira TCM Supports Older Adults with Recurrent Dizziness
At Aspira TCM, Dr Chan will first ask about the type of dizziness, attack timing, blood pressure and glucose, medication, chronic illness, sleep, appetite, bowel and bladder habits, tinnitus, palpitations, chest discomfort, numbness, fall risk, and tongue-pulse findings.
If stroke risk, heart disease, acute inner-ear disease, collapse, or head-injury risk is suspected, urgent medical review is recommended first. If the condition is stable and suitable for TCM support, treatment may focus on qi-blood deficiency, phlegm-damp, liver yang, liver-kidney deficiency, or blood stasis, using herbs, acupuncture, ear-point therapy, and practical lifestyle advice.
If you or an older family member has recurrent dizziness and you are unsure which specialty to see, prepare a dizziness diary, blood pressure and pulse readings, medication list, and fall history before booking an assessment. If any acute warning sign appears, seek medical help first.
FAQ — Common Questions About Dizziness in Older Adults
Q1: Should an older adult with dizziness see TCM or Western medicine first?
If dizziness is sudden or comes with slurred speech, one-sided weakness, chest pain, collapse, or head injury, emergency or Western assessment must come first. If the dizziness is recurrent, stable, and urgent causes have been excluded, TCM may be considered as part of care.
Q2: Does spinning vertigo always mean BPPV?
No, but brief spinning triggered by turning or rolling in bed often raises BPPV or vestibular problems as possibilities. Medical or ENT assessment is still recommended before self-diagnosis.
Q3: Can dizziness occur even when blood pressure is normal?
Yes. Dizziness may relate to inner-ear disease, anaemia, low blood sugar, medication effects, sleep problems, neck issues, phlegm-damp patterns, qi-blood deficiency, or reduced balance. One normal blood-pressure reading does not rule out everything.
Q4: Can TCM help with dizziness?
It may help in stable situations, after urgent ear, brain, heart, and collapse-related causes have been considered. TCM works by pattern differentiation rather than replacing emergency or specialist assessment.
Q5: If an older adult feels dizzy on getting up, can they stop blood-pressure medicine on their own?
No. Antihypertensive medication should not be stopped or reduced without medical advice. Record the dizziness timing, blood pressure readings, and medication details, then ask the treating doctor whether adjustment is needed.
Related reading:
- TCM Wisdom for Stroke Prevention: A Complete Guide to Warning Signs, Daily Care & 4 Key Acupoints for Seniors →
- Older Adults Waking Easily at Night, Dreaming More, or Waking Too Early: How TCM Distinguishes Causes and Sleep Patterns →
- Book a consultation →
Disclaimer: This article is for health education only and cannot replace personal consultation, examination, medication, or treatment advice. Seek immediate medical attention if dizziness comes with one-sided weakness, slurred speech, facial droop, chest pain, breathlessness, collapse, severe headache, confusion, head injury after a fall, or extreme blood-pressure abnormality. Any medication adjustment should first be discussed with the treating doctor.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Recurrent Knee Pain in Older Adults: Is It Just Degeneration?
Recurrent knee pain in older adults is not always simple degeneration. Osteoarthritis, muscle weakness, cold-damp patterns, qi-blood deficiency, old injuries, and fall risk may all contribute. This article explains common causes, red-flag signs, TCM patterns, and practical ways to reduce recurrence.

Back Pain in Older Adults: Osteoporosis, Degeneration, or Sciatica?
Back pain in older adults may arise from muscular strain, lumbar degeneration, sciatica, osteoporotic fracture, falls, or other medical conditions. This article compares common causes, red-flag signs, when investigation is needed, and how TCM may help once urgent problems are excluded.

Bigger Belly, Same Weight? TCM on Bloating, Constipation, and Fat
Stable weight but a more prominent belly does not always mean fat. Water retention, constipation, gastrointestinal bloating, posture, reduced muscle mass, and central obesity can all make the abdomen appear larger. This article uses TCM perspectives on digestion, phlegm-damp, qi stagnation, and constipation to help you distinguish situations and decide next steps.