Acupuncture for Parkinson's Disease? Combining TCM and Medication
Parkinson's patients on long-term dopaminergic medication such as Madopar are often asked by family members whether acupuncture and Chinese herbs can help with tremor, stiffness, constipation or insomnia. This article compares the roles of Western medication and acupuncture-based TCM care across disease stages and TCM patterns, lays out where the two combine well, and lists the warning signs that must go to neurology or emergency care first.
Medical review: Dr. Chan Wing Kiu, Joanne,Registered Chinese Medicine Practitioner #009463
1-Minute Quick Answer
Acupuncture and Chinese herbs can't replace levodopa-based medication in Parkinson's disease — diagnosis, staging, drug adjustment, and deep brain stimulation evaluation must be neurology-led. TCM (reviewed by Dr Chan, CMCHK 009463) may still help with rigidity, constipation, insomnia, and fatigue. Sudden motor deterioration, post-fall confusion, severe swallowing difficulty, or hallucinations need emergency care immediately.
Can Acupuncture Help in Parkinson's Disease? A Guide to Sharing the Load Between Western Medicine and TCM
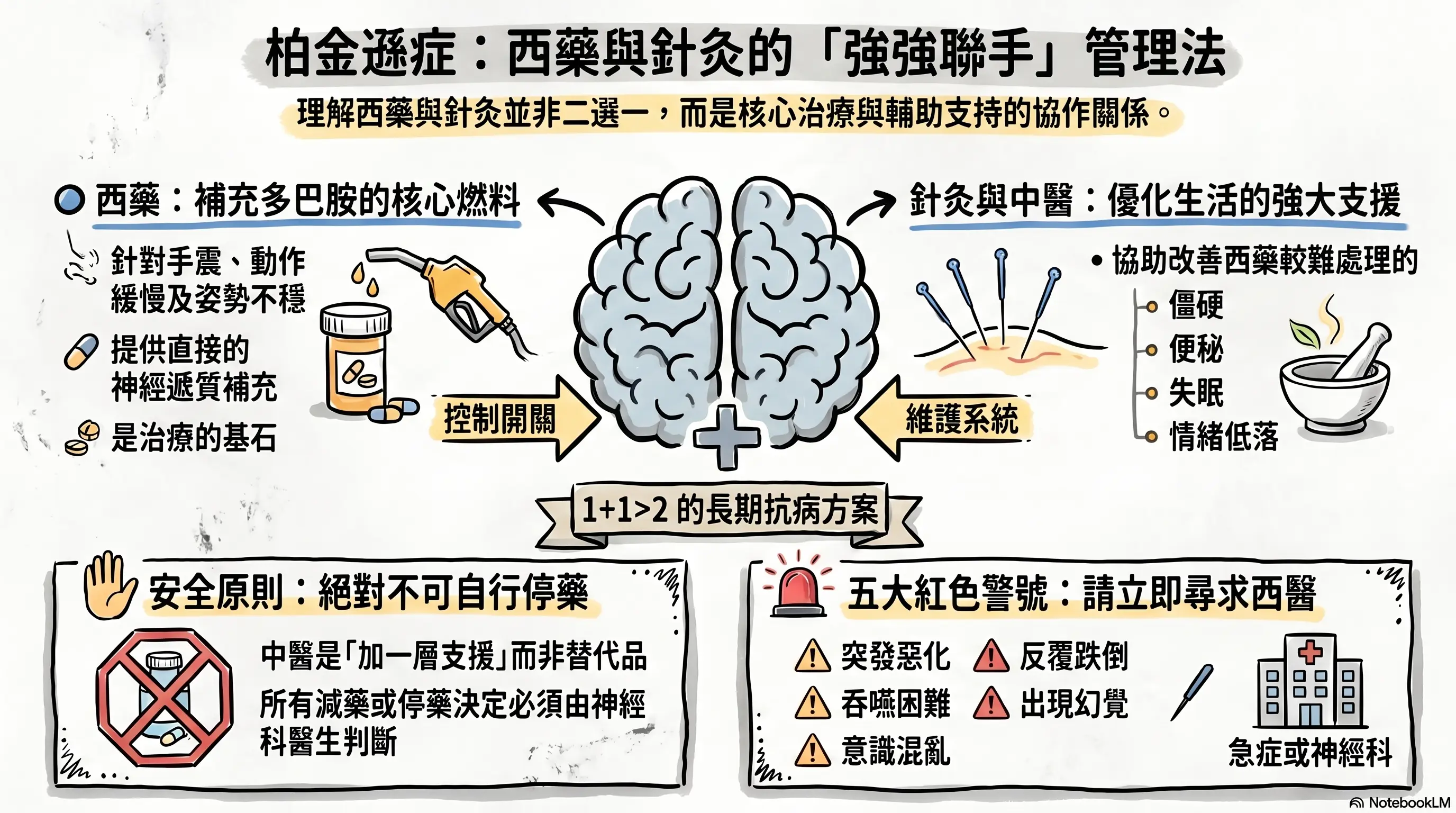 For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
For quick reference, this image was generated by NotebookLM. Some Chinese characters may not render perfectly; we appreciate your understanding.
Medical review: Dr Chan Wing-kiu (CMCHK 009463; geriatric gynaecology and internal medicine)
"My father is on Madopar but his hand still trembles in the afternoon — can acupuncture help?" "He has just been diagnosed with Parkinson's disease — should we get him to a TCM practitioner as early as possible?" "His on-time is shrinking — can TCM help with that?" These are the kinds of family enquiries Aspira TCM Clinic receives every month.
The two biggest misconceptions families bring are treating TCM as a "replacement for Western medication" or as a "miracle anti-degeneration tonic". This article sets out three things clearly: what each side does, where the two combine well, and what must be led by neurology or the emergency department.
Two Different Goals
Western medicine: replacing dopamine. Parkinson's disease (PD) is a neurodegenerative disorder caused by the loss of dopamine-producing cells in the substantia nigra of the basal ganglia, leading to slowed movement initiation and reduced fluency. Typical features include resting tremor, limb rigidity, bradykinesia and postural instability. The main medications are levodopa-based (Madopar, Sinemet), dopamine receptor agonists, MAO-B inhibitors and others, all aiming to replenish or preserve dopamine. They improve symptoms but do not reverse the underlying degeneration. Over time, some patients develop "on–off" fluctuations, "wearing-off" effects and dyskinesias. For mid-to-late stage patients, deep brain stimulation (DBS) surgery may be discussed.
Distinguish Parkinson's disease from Parkinson's syndrome. Parkinson's disease is primary neurodegeneration and usually responds to levodopa. Parkinson's syndrome is secondary — possible causes include side effects of psychiatric medication, post-encephalitis, head trauma, vascular disease, Alzheimer's disease and Lewy body dementia — and it tends to respond poorly to levodopa. Diagnosis is the responsibility of a neurologist; TCM should not lead this part.
Hoehn & Yahr staging — a simple way for families to locate themselves.
| Stage | Features | TCM role |
|---|---|---|
| Stage 1–2 (early) | Unilateral or bilateral symptoms without balance impairment; daily life still independent | Better window for adding TCM |
| Stage 3 (middle) | Bilateral symptoms with impaired walking balance and frequent falls | Useful for constipation, insomnia and muscle tightness |
| Stage 4–5 (late) | From needing help with daily activities to wheelchair-bound or bedridden | Focus on quality of life and complication management |
TCM perspective: strengthen the root, supplement what is deficient and drain what is in excess. Classical Chinese medical texts include conditions resembling PD under "tremor disorders" (zhan bing, zhen diao). The picture is typically linked to age-related weakness, liver-and-kidney deficiency, spleen-and-kidney deficiency and undernourished tendons, with wind, fire, phlegm and stasis sometimes adding to it. Common patterns include internal liver wind (worsening tremor with stress and emotion), qi-and-blood deficiency (slow movements, easy fatigue), liver-and-kidney yin deficiency (dizziness, dry mouth, nocturia, insomnia), and phlegm and stasis blocking the channels (rigidity, constipation, thick greasy tongue coating). The role of TCM is not to "replace dopamine", but to help with symptoms, ease side effects of Western medication and improve quality of life — so that patients can live with the condition more comfortably over the long term.
Comparison Table: Roles of Western Medication and Acupuncture-Based TCM Care
| Item | Western medication (mainly levodopa-based) | Acupuncture and TCM care |
|---|---|---|
| Main mechanism | Replenishing or preserving dopamine to control motor symptoms | Pattern differentiation; adjusting liver wind, qi and blood, liver and kidney, phlegm and stasis |
| Main targets | Tremor, rigidity, bradykinesia, postural instability | Constipation, insomnia, rigidity, muscle tightness, mood, fatigue |
| Common side effects | Nausea, dizziness, hypotension, hallucinations, dyskinesia, on–off fluctuations | Occasional bruising, post-needling soreness; herbs may cause diarrhoea or allergy |
| Key monitoring | Neurology follow-up, drug adjustment, cognition and mood assessment | Tongue and pulse, constitutional change, sleep, bowel and urine, fall risk |
| Cannot replace | Neurology follow-up and prescription | Emergency care and neurology lead |
When Western Medicine and TCM Combine Well
The following situations are well-suited to TCM care alongside Western medication:
| Symptom | Common TCM direction | Combination focus |
|---|---|---|
| Limb rigidity and muscle tightness | Soothing liver, calming wind, moving qi and blood | Combine with daily stretching and physiotherapy |
| Constipation | Moistening the bowels, replenishing qi and blood | Adequate fluids, fibre and activity |
| Insomnia, vivid dreams, mid-night waking | Nourishing blood and yin, calming the spirit | Mind nocturia and caffeine intake |
| Low mood and anxiety | Soothing the liver, calming the heart-spirit | Severe depression must be assessed by psychiatry first |
| Fatigue and on-time fluctuation | Replenishing qi and blood, strengthening spleen and kidney | Does not replace medication; align with meal timing |
| Unsteady gait and falls | Tonifying liver and kidney, strengthening tendons and bones | Fall-prevention setup and physiotherapy take priority |
Acupuncture and Chinese herbs serve as "an extra layer of support on top of Western medication", not a substitute for Madopar. Clinically, an initial intensive phase of 2–3 sessions a week is common, gradually moving to once a week or once every two weeks as symptoms improve; herbs are reviewed every 1–2 weeks based on pattern.
When Western Medicine or Emergency Care Must Lead
The following are red flags requiring immediate neurology contact or emergency care:
- Diagnosis and staging, drug selection and adjustment, and DBS evaluation must all be decided by a neurologist
- Sudden motor deterioration, inability to stand up, repeated falls, post-fall confusion
- Severe swallowing difficulty, choking, coughing fits or recurrent aspiration pneumonia
- Sudden confusion, disorientation, hallucinations or delusions
- Severe hypotensive fainting, palpitations, chest pain
- Acute severe constipation with abdominal distension, pain or vomiting
- Any suspected stroke or severe drug side effect
Aspira TCM Clinic does not advise patients to stop or reduce Madopar or to skip neurology follow-up on their own. Any change in medication must be made by the prescribing doctor.
How Aspira TCM Clinic Approaches Parkinson's Patients
At the first visit, Dr Chan asks Parkinson's patients to bring along:
- The Western prescription list (levodopa-based, other Parkinson's medications and any comorbidity drugs)
- Recent neurology follow-up notes, MRI or other reports
- Any history of falls, swallowing difficulty or infections
- The neurologist's name and clinic contact for ongoing communication
- Any Chinese medicines and supplements currently used
The doctor decides — based on pattern differentiation — whether Chinese herbs and acupuncture are appropriate, and assesses for DBS implants, cognition and home safety. The whole programme runs on the principle of supporting the Western prescription and is never marketed as "stopping the medication" or "reversing Parkinson's". If dyskinesia worsens, "on-time" suddenly shortens or new symptoms appear during acupuncture, neurology contact is advised immediately.
FAQ
1. Can acupuncture replace Madopar?
No. The core treatment of Parkinson's disease remains Western medication and neurology-led care. Acupuncture's role is to improve quality of life and support symptoms, not to substitute for medication; any decision to stop a drug must be made by the neurologist.
2. How long does acupuncture take to show effect?
Responses vary widely. A typical starting frequency is 2–3 sessions a week, with 4–8 sessions forming an observation period before adjusting (e.g., once a week or once every two weeks). The goal is steady improvement of symptoms and quality of life — not a "one-shot fix".
3. Can Chinese herbs interfere with the absorption of Madopar?
Some herbs and foods — particularly high-protein foods or certain tonifying soups — can interfere with levodopa absorption. The registered TCM doctor avoids prescriptions that obviously affect drug metabolism and keeps the neurologist informed.
4. Is acupuncture still possible after deep brain stimulation (DBS) surgery?
For some patients, yes — but only after assessment by both the neurologist and a registered TCM doctor. Acupuncture must avoid the area of the implanted device; strong magnetic or electrotherapy modalities are not recommended.
5. Can the family give "brain-tonic" or "kidney-tonic" soups to a Parkinson's patient?
Self-prescribing such soups is not advised. Many of them contain ginseng, lingzhi, fo-ti (he shou wu), dang gui and similar herbs, which can interact with Parkinson's medications or other comorbidity drugs. Any long-term dietary therapy should first be discussed with a registered TCM doctor and the prescribing physician.
6. Do tai chi and qigong help Parkinson's patients?
A 2014 study published in Cell Transplantation reported that regular tai chi practice was associated with an increase in circulating progenitor cells in the bloodstream. Clinical experience also suggests tai chi benefits motor coordination, breathing and balance. Within a patient's physical capacity, these gentle activities can form part of long-term lifestyle management — but they are not treatment, and they cannot replace a Western prescription.
7. Can TCM "cure" or "reverse" Parkinson's disease?
No. Parkinson's disease is a neurodegenerative condition, and at present no Chinese or Western therapy can reverse the underlying degeneration. The TCM role is to support symptoms and quality of life on top of Western care; honest goals are more important than exaggerated promises.
Related reading:
- TCM Wisdom for Stroke Prevention: A Complete Guide to Warning Signs, Daily Care & 4 Key Acupoints for Seniors →
- Acupuncture vs Physiotherapy: Which Is Better for Your Pain? →
- Acupuncture treatment →
Disclaimer: This article is for general health education only and does not replace individual diagnosis, prescription or emergency care. It is not advice to stop, reduce or switch any medication. For sudden motor deterioration, post-fall confusion, severe swallowing difficulty or major mood changes, contact neurology or the emergency department immediately.
Disclaimer: This article is for health education and reference purposes only and does not constitute medical advice, diagnosis, or treatment. Each patient's condition is unique and treatment outcomes vary. Please consult a registered TCM practitioner or qualified healthcare professional for health concerns.
Want to learn more? WhatsApp us for a free consultation
Book via WhatsAppExplore our full range of treatments: Traditional TCM Services
Related Articles

Can I See a TCM Practitioner While on a GLP-1 Injection?
GLP-1 weight-loss injections are now a major talking point in Hong Kong. This article compares the roles of prescribed GLP-1 medication and TCM care across three phases — before treatment, during treatment and after stopping — covering medical monitoring, side-effect relief and post-discontinuation rebound, and identifying scenarios that should not be managed by TCM alone.

168 Fasting vs Low-Carb vs Keto: A TCM Guide to the Differences
168 fasting, low-carb diets, and keto are all popular weight-loss approaches, but they restrict different things — and their effects on digestion, sleep, blood glucose, bowels, menstruation, and mood differ accordingly. This article compares the three, explains which TCM constitutions need extra caution, and flags situations that warrant prior assessment by a Western doctor or registered dietitian.

TCM Embedding vs Weight-Loss Injections vs Medical Aesthetics vs Liposuction — A Complete Comparison of 4 Mainstream Approaches
With so many weight-loss options on the market, which is right for you — TCM embedding, weight-loss injections, fat-freezing, or liposuction? Dr Au compares all four mainstream approaches across mechanism, speed of results, side effects, price range, rebound rate, and suitability — helping you avoid the pitfalls of "stop the drug, gain it back" and "treat the symptom, not the root."